Case Report
Ulcerative Colitis Associated with Cholangiocellular Carcinoma: A Case Report and Literature Review
Lei Li1, Ying Fang1, Ruofan Sheng2, Yujen Tseng1, Xizhong Shen1 and Jiyao Wang1*
1Department of Gastroenterology and Hepatology, Zhongshan Hospital, Fudan University, Shanghai 200032, China
2Department of Radiology, Zhongshan Hospital, Fudan University, Shanghai 200032, China
*Corresponding author: Jiyao Wang, Department of Gastroenterology and Hepatology, Zhongshan Hospital, Fudan University, Shanghai 200032, China
Published: 06 May, 2017
Cite this article as: Li L, Fang Y, Sheng R, Tseng Y, Shen
X, Wang J. Ulcerative Colitis Associated
with Cholangiocellular Carcinoma: A
Case Report and Literature Review.
Ann Clin Case Rep. 2017; 2: 1351.
Abstract
A 24-year-old female patient has a history of Ulcerative colitis (UC) for 14 years and was treated with mesalazine. Her UC symptoms were alleviated after administration of mesalazine, however, she was repeatedly found to have abnormal liver function. The diagnosis of Cholangiocellular Carcinoma (CCC) was made via ultrasound and magnetic resonance imaging. Clinical data of the patient was retrospectively analyzed and relevant literature was reviewed to investigate the possibility for Ulcerative Colitis (UC) to progress to Cholangiocellular Carcinoma (CCC). A review of the literature suggested that UC is commonly associated with concomitant primary sclerosing cholangitis, which progresses to CCC in 11% of cases. Clinicians should be aware that UC may progress to CCC. UC patients with recurrent abnormal liver function, especially in those with serum alkaline phosphatase elevation, should undergo relevant examinations to clarify diagnosis.
Keywords: Ulcerative colitis; Primary sclerosing cholangitis; Cholangiocellular carcinoma
Introduction
Primary Sclerosing Cholangitis (PSC) is the most common hepatobiliary complication related to ulcerative colitis (UC). The majority of PSC cases ultimately progress to end-stage liver disease, and ~11% are associated with concomitant Cholangiocellular Carcinoma (CCC). This study provides a clinical analysis of a UC patient with concomitant CCC and a review of relevant literature was conducted to raise awareness regarding possible progression of UC to CCC.
Case Presentation
General data
A 24-year-old female patient was admitted to Zhongshan hospital due to recurrent abnormal
liver function over a period of 14 years and upper abdominal pain for over 1 month. She was treated
with mesalazine after the diagnosis of UC in 1999. Several follow-up examinations revealed elevated
Alanine Aminotransferase (ALT), Aspartate Aminotransferase (AST), Alkaline Phosphatase
(ALP), and γ-Glutamyl Transpeptidase (GGT). Specifically, ALP and GGT were elevated to
2–3-fold of the Upper Limit of Normal (ULN). During regular follow-ups, the patient did not
report any symptoms of discomfort such as bloating or abdominal pain; no nausea, vomiting or
anorexia; no fever, rash or xanthochromia of the skin and sclera. No further diagnosis or treatment
was commenced. In 2009, her UC was well controlled and the dose of mesalazine was gradually
reduced to withdrawal. Six months after withdrawal of mesalazine, repeat liver function tests
showed elevated liver enzymes, especially ALP and GGT, which were 1–2-fold of ULN. The patient
sought medical attention, but the subsequent liver biopsy did not reveal any obvious abnormalities.
She was given intermittent, symptomatic treatment for liver dysfunction. In February 2015, the
patient experienced postprandial upper abdominal pain. The patient denied acid reflux, belching,
nausea, vomiting, diarrhea, fever, rash, jaundice, joint pain and other discomforts. She visited a
local hospital and liver function tests showed: total bilirubin 21 μmol/L, conjugated bilirubin 14
μmol/l, albumin 42 g/l, ALT 117 IU/l, AST 131 IU/l and ALP 962 IU/l. She tested negative for
hepatitis A, B, C and E viral markers. Gastroscopy showed superficial gastritis, polypoid bulge, and
erosion in the gastric antrum, and cardiac polyp (most likely inflammatory). Gastric antral mucosal
biopsy showed severe active chronic superficial inflammation with mucosal erosion. Abdominal
ultrasound showed hepatomegaly, diffuse liver lesion, hypoechoic mass in the left hepatic lobe, and
gallbladder wall edema. Abdominal contrast-enhanced CT showed focal liver lesions, suspicious for
neoplastic lesions, likely atypical hemangioma or bile-duct-derived tumors. To clarify the nature of focal liver lesions, the patient was admitted to the Department of
Gastroenterology of Zhongshan hospital. Since the onset of disease,
she maintained a clear state of consciousness with normal mental
health and appetite, sufficient sleep, normal urination and defecation,
and denies significant weight fluctuation. The patient is allergic to
cephalosporin. She denied a history of hepatitis, tobacco smoking or
alcohol consumption, and toxicant exposure. She was single and has
no children, and has a normal menstrual cycle. Her parents were in
good health.
Physical examination
Upon admission, her body temperature was 36.8ºC, pulse rate
was 78 beats/min, respiratory rate was 18 breaths/min, and blood
pressure was110/78 mmHg. She was conscious, mentally normal,
physically active and cooperative upon examination. Her skin and
sclera showed xanthochromia with no evident hemorrhagic spots,
liver palm, or spider angioma. She had no palpable enlargement of
superficial lymph nodes. The percussion and breath sounds of both
lungs were clear. She had no precordial bulge and the border of cardiac
dullness was within normal limits. Her heart rhythm was regular and
no pathological murmurs were auscultated in the auscultatory sites.
Her abdomen was flat and soft, with right upper quadrant tenderness
but no rebound tenderness, muscle tension or abnormal mass. Her
liver was palpable with one finger under the costal margins, while
the spleen was not palpable. Her renal and hepatic regions were not
sensitive to percussion. Shifting dullness was negative. Bowel sound
frequency was 3 times/min. Neurological examination was negative.
No pitting edema was observed on either lower extremities.
Laboratory tests
Blood: erythrocyte count 3.60 × 1012/l, hemoglobin 104 g/l,
platelet count 501 × 109/l, leukocyte count 9.67 × 109/l, percentage
of neutrophils 71.3%, percentage of lymphocytes 16.2%; erythrocyte
sedimentation rate: >120 mm/H. Urine: bilirubin ++, without any
other abnormalities; stool: normal; fecal occult blood: negative. Liver
function: total bilirubin 64.4 μmol/l, direct bilirubin 59.7 μmol/l,
albumin 33 g/l, globulin 38 g/l, ALT 55 U/l, AST 61 U/l, ALP 561 U/l,
GGT 382 U/l, lactate dehydrogenase 201 U/l, cholinesterase 4132 U/l,
prealbumin 0.12 g/l; kidney function: urea 1.8 mmol/l, creatinine 39 μmol/l, uric acid 139 μmol/l. Coagulation: prothrombin time 12.2 s,
international normalized ratio 1.05, activated partial thromboplastin
time 36.5 s, D-dimer 2.17 mg/l. Tumor markers: carbohydrate antigen
(CA)125 451.3 IU/ml; α fetoprotein, carcinoembryonic antigen,
CA199 was within the normal range. Ferritin >2 μg/ml. Electrolyte
and autoantibodies were within the normal range.
Auxiliary examination
Upper abdominal contrast-enhanced magnetic resonance
imaging (Figure 1) revealed a space-occupying lesions in the left
hepatic lobe, with a tubercle in the caudal lobe involving blood
vessels of the left lobe, suspicious for atypical hemangioma or bile
duct Malignant Tumor (MT); other features included mild porta
hepatis lymphadenopathy and edema, as well as thickening of the
gallbladder wall. Contrast-enhanced ultrasound for liver imaging
showed multiple solid lesions in the left lobe, highly suspicious for
MT (cholangiocyte-derived); embolization of the left portal vein;
and porta hepatis lymphadenopathy. Computed Tomographic
Angiography (CTA) of the hepatic artery and Computed Tomography
Venography (CTV) of the portal vein, hepatic vein and inferior vena
cava revealed invasion of the left hepatic artery, left and middle hepatic
veins, and left portal vein. Nuclear medicine imaging of systemic
cancer by Positron Emission Tomography (PET)/CT indicated high
suspicion for MT in the left lobe with intrahepatic metastasis, and
porta hepatis, retroperitoneal and thoracic lymph node metastases,
as well as abdominal and pelvic implantation metastases, with a small
amount of peritoneal fluid.
Figure 1
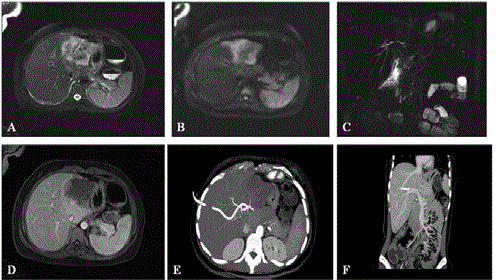
Figure 1
(A) Large liver lesion onthe left hepatic lobe with in distinct
boundary, measured approximately 7.1 × 5.1 cm in size; heterogeneous
high signal on T2-weighted imaging and (B) high signal on diffusion-weighted
imaging; (C) MRCP revealed irregular intrahepatic bile duct stricture; (D)
contrast-enhanced arterial phase lesions presented with peripheral irregular
enhancement; (E,F) CTA of the hepatic artery and CTV of the portal vein,
hepatic vein and hepatic artery indicated invasion of the left hepatic artery,
left and middle hepatic veins, and left hepatic portal vein, with blurred
boundaries.
Diagnosis and Treatment
The patient presented with progressive jaundice after admission. A Percutaneous Transhepatic Cholangial Drainage (PTCD) was performed on March 17, 2015. Intra-operative cholangiography revealed a slight right intrahepatic bile duct dilatation and irregular right hepatic duct stricture. Jaundice was alleviated following PTCD.
Discussion
Inflammatory Bowel Disease (IBD) is an immune-mediated and
non-specific inflammatory condition of the gastrointestinal tract
characterized by repeated recurrence and chronicity, including UC
and Crohn’s disease. It is reported that 21–47% of IBD cases are
associated with extra intestinal manifestations [1,2]. Extra intestinal
manifestations involving the skin, eyes, and joints are often presented
in parallel with disease activity of IBD, while hepatobiliary system
diseases such as PSC, small-duct PSC, primary biliary cirrhosis,
non-alcoholic fatty liver diseases, and cholelithiasis are inconsistent
with IBD progression but generally occur independent of intestinal
inflammation. PSC is an unexplained chronic cholestatic liver disease
characterized by progressive inflammation, fibrosis and multiple
stenosis of the intrahepatic and extrahepatic bile duct systems. PSC
is currently well recognized as the most common hepatobiliary
complication of IBD. The relationship between PSC and IBD has been
reported mainly in Western countries. Up to 80% of PSC cases are
associated with IBD in Northern Europe and the United States. The
incidence of IBD–PSC is 50% in Southern Europe and 35% in Asia,
reported mainly in Japan and Korea. Few studies have been reported
in China, of which, recent reports on the incidence of IBD-PSC were
single-center studies with small sample size. Despite large differences
in the results, the incidence of IBD-PSC is significantly lower in
China compared to that of Europe and the United States [3,4]. In
other countries, 1.4–7.5% of IBD patients develop concomitant PSC during disease progression, with a UC incidence of 2.0–7.5% and a CD incidence of 1.4–3.4% [5]. Similar results have been obtained by
recent studies in China [6].
The pathogenesis of PSC–IBD remains unclear. From a
microbiology viewpoint, IBD is diagnosed when permeability of the
intestinal-mucosal barrier increases, allowing bacterial endotoxins
and toxic cholic acids concentration to increase in the blood,
then transported to the liver to activate Kupffer cells, triggering
inflammatory mediators (eg. tumor necrosis factor), facilitating bile
duct damage and hyperplasia resembling the pathological changes
in PSC. This point of view is supported by the finding of intestinal
bacilli in the portal veins of an animal model, although the exact
pathogenesis remains unclear [7].
Significantly diverse clinical manifestations can be found in
PSC, which may range from asymptomatic to recurrent episodes of
jaundice, fatigue, anorexia, weight loss, abdominal pain, pruritus,
hepatosplenomegaly, ascites, fever and diarrhea. Most PSC patients
are asymptomatic upon diagnosis, but merely presents with elevation
of serum ALP or other biochemical indices of hepatic function.
Thus, PSC is easily over looked, leading to clinical misdiagnosis.
Clinical awareness should be stressed in IBD patients with persistent
abnormalities of liver function, especially those with persistent
ALP elevation, for possible diagnosis of concomitant PSC. Current
diagnosis of PSC is based primarily on imaging studies. Although
Endoscopic Retrograde Cholangiopancreatography (ERCP)
remains the gold standard [8] for diagnosis, its invasive nature can
lead to serious complications. Owing to its non-invasiveness and
ease of operation, Magnetic Resonance Cholangiography (MRCP)
is increasingly used for diagnosis of PSC, with a sensitivity of 80%
and specificity of 90% [9]. The typical pathological feature of PSC
is the “onion-skin” type bile duct fibrosis. This pathological change
can be used as the basis for diagnosis and determination of lesion
severity. However, such pathological feature only applies to 10% of
PSC patients, thus limits its diagnostic value. Research has shown
that liver biopsy cannot provide additional diagnostic information
for IBD patients after being examined by cholangiography [10].
Therefore, liver biopsy is not recommended for patients with
typical lesions evident on cholangiography [11]. Liver biopsy
needs to be further considered only when the diagnosis by ERCP
is inconclusive. The patient reported in this study had a 14-years
history of UC and previously treated with mesalazine for an extended
period of time. During the course of disease, her liver function
was repeatedly found to be abnormal, with prominent elevation of
ALP and GGT, without obvious clinical manifestations. She was
misdiagnosed with mesalazine-induced liver damage, without further
relevant examinations. After admission to our hospital, MRCP
showed irregular intrahepatic biliary stricture (Figure 1E and 1F).
Cholangiography during PTCD showed right intrahepatic bile duct
dilatation and irregular right hepatic duct stricture. No abnormalities
was reported by the liver biopsy. However, as previously discussed,
liver biopsy poses limitations and therefore, the patient was still
considered to have UC with concomitant development of PSC.
PSC has a poor prognosis, with an average survival period of
9.6–18 years. The risk ratio of PSC associated with various malignant
tumors is 13–14%; most commonly CCC (11%) followed by
colorectal carcinoma (9%). Other concomitant malignancies include
hepatocellular carcinoma, gallbladder carcinoma and pancreatic
carcinoma [9]. Progression of PSC into CCC occurs mainly in patients with history of IBD of over 15 years, or patients who have pancolitis,
regardless of disease severity [12]. CCC–PSC is present in adolescents
as well as adults [13]. After admission to our hospital, MRCP,
contrast-enhanced ultrasound and PET–CT all suggested bile-ductderived
malignancy in our patient. Hence, she was considered to have
developed concomitant PSC during the course of UC, which further
progressed to CCC. Since the patient evident distant metastases, she
was diagnosed with end-stage CCC.
Currently, there are no available treatment that can alter disease
progression or the natural course of PSC. Studies have shown that lowdose
ursodeoxycholic acid (UDCA; 13–15 mg/kg/day) has a positive
role in improving liver function in patients with PSC, while high-dose
UDCA (28 mg/kg/day-30 mg/kg/day) does not provide additional
benefits [14]. Recent clinical follow-up studies with large samples
have indicated that although UDCA can improve biochemical indices
for PSC patients, it has no effect on liver histology and no significant
impact on mortality, need for liver transplantation, and prognosis
of CCC [15]. Endoscopic intervention and surgical procedures can
alleviate biliary obstruction and reduce liver damage to a certain
extent, however, liver transplantation is still preferred for endstage
PSC or CCC–PSC. Liver transplantation is the only effective
treatment, with 5- and 10-year survival rates of 85% and 70% posttransplantation,
respectively. Unfortunately, our patient had distant
metastases and liver transplantation was contraindicated, thus, only
interventional therapy was applied to alleviate her symptoms.
AN Ananthakrishnan “et al.” [16] reported that patients
with IBD–PSC had significantly increased overall risk of cancers
including cholangiocarcinoma compared to patients without PSC.
Tsuchiya “et al.” [17] reported a case of concomitant colitic cancer
and intrahepatic cholangiocarcinoma in a patient with history of
UC recently. Clinicians should be aware of the disease and closely
monitor UC patients who repeatedly have abnormal liver function
test results. Specifically, in patients with persistent ALP elevation,
MRCP or ERCP should be employed to clarify diagnosis and provide
timely intervention when necessary.
Research Funding
National Natural Science Foundation of China (No. 81370549).
References
- Lichtenstein DR. Hepatobiliary complications of inflammatory bowel disease. Curr Gastroenterol Rep. 2011;13(5):495-505.
- Bernstein CN, Blanchard JF, Rawsthorne P, Yu N. The prevalence of extraintestinal diseases in infl ammatory bowel disease: a population-based study . Am J Gastroenterol. 2001;96(4):1116-22.
- Luo KF, Su X, Zhang XM, Li W. Primary sclerosing cholangitis: A clinical analysis of 26 cases. Aca J Chinese PLA Med School. 2014;35(5):404-7.
- Liu X, Du ZG, Jia JD. Detection rate of primary sclerosing cholangitis in 160 cases of ulcerative colitis. Chinese J Hepatol. 2005;13(8):614.
- Boonstra K, van Erpecum KJ, van Nieuwkerk KMJ, Drenth JP, Poen AC, Witteman BJ, et al. Primary sclerosing cholangitis is associated with a distinct phenotype of inflammatory bowel disease. Inflamm Bowel Dis. 2012;18(12):2270-6.
- Zhang KG, Yin BS, Yang RS, Wang SM, Zheng BH, Jia Y, Wu ZX. Study of clinical features in patients with ulcerative colitis accompanied by primary sclerosing cholangitis. J Rare Uncom Dis. 2001;8(2):7-8.
- Aron JH, Bowlus CL. The immunobiology of primary sclerosing cholangitis. Semin Immunopathol. 2009;31(3):383-97.
- Lee YM, Kaplan MM. Primary sclerosing cholangitis. N Engl J Med. 1995;332(14):924-933.
- Lutz H, Trautwein C, Tischendorf JW. Primary sclerosing cholangitis: diagnosis and treatment. Dtsch Arztebl Int. 2013;110(51-52):867-74.
- Burak KW, Angulo P, Lindor KD. Is there a role for liver biopsy in primary sclerosing cholangitis? Am J Gastroenterol. 2003;98(5):1155-8.
- Chapman R, Fevery J, Kalloo A, Nagorney DM, Boberg KM, Shneider B, et al. Diagnosis and management of primary sclerosing cholangitis. Hepatology. 2010;51(2):660-678.
- Moreno Luna LE, Gores GJ. Advances in the diagnosis of cholangiocarcinoma in patients with primary sclerosing cholangitis. Liver Transpl. 2006;12(S2):S15-S19.
- Liu R, Cox K, Guthery SL, Book L, Witt B, Chadwick B, et al. Cholangiocarcinoma and high-grade dysplasia in young patients with primary sclerosing cholangitis. Dig Dis Sci. 2014;59(9):2320-4.
- Triantos CK, Koukias N, Nikolopoulou V, AK Burroughs. Ursodeoxycholic acid in primary sclerosing cholangitis. Aliment Pharmacol Ther. 2012;35(5):622-3.
- Triantos CK, Koukias NM, Nikolopoulou VN, Burroughs AK. Meta-analysis: ursodeoxycholic acid for primary sclerosing cholangitis. Aliment Pharmacol Ther. 2011;34(8):901-10.
- AN Ananthakrishnan, A Cagan, VS Gainer, Su-Chun Cheng, Tianxi Cai, Peter Szolovits, et al. Mortality and extra intestinal cancers in patients with primary sclerosing cholangitis and inflammatory bowel disease. J Crohn’s Colitis. 2014;8(9):956-963.
- Tsuchiya K, Nanashima A, Ikeda T, Minami S, Nagano M, Hamada T, et al. A case of concomitant colitic cancer and intrahepatic cholangiocarcinoma during follow-up for ulcerative colitis. Clin J Gastroenterol. 2017;10:157.