Case Report
Acquired Lumbar Spinal Stenosis as a Consequence of a Spinal Synovial Cyst Presenting with Paraparesis: A Case Report
Myron M. LaBan* and Douglas Boven
Department of Physical Medicine and Rehabilitation, Oakland University William Beaumont School of Medicine,
Michigan, USA
*Corresponding author: Myron M. LaBan, Department of Physical Medicine and Rehabilitation, Oakland University William Beaumont School of Medicine, 3601 W. 13 Mile Road, Royal Oak, Michigan 48073, USA
Published: 02 May, 2017
Cite this article as: LaBan MM, Boven D. Acquired Lumbar
Spinal Stenosis as a Consequence of
a Spinal Synovial Cyst Presenting with
Paraparesis: A Case Report. Ann Clin
Case Rep. 2017; 2: 1347.
Abstract
Synovial and/or ganglionic cysts of the lumbar spine usually present with complaints of radicular pain. Less often, larger cysts are also associated with complaints of ambulatory-associated “weakness”. Such was the case of a 60-year-old male initially clinically suspected of having lumbar spinal stenosis. The etiopathogenesis of large ganglion cysts is reviewed with reference to symptoms, clinical signs and pathogenesis.
Keywords: Ganglion cyst; Paraparesis; Spinal stenosis; Synovial cyst
Introduction
Intra-spinal synovial cysts and/or ganglion cysts in juxtaposition to a degenerative vertebral
facet joint can become a mechanical source of spinal root and/or cord compression [1]. In 40% of
these cases, they occur as a product of an “unstable” arthritic facet joint, i.e., degenerative spondylitis
[2]. They present most often in the sixth decade of life with a slight predominance of females [3].
Although occurring at all levels of the spine, 95 percent can be found at lumbar vertebral levels,
usually at the juncture of the L4-L5 vertebrae, the lumbar spine’s most unstable segment. The rest
occur in descending order of frequency at L5-S1 and at L3-L4 levels, rarely if ever in the sacrum [4].
Symptoms and clinical signs of nerve root and/or spinal cord compression by a synovial cyst are
consistent with the vertebral level of spinal root compromise.
At all spinal levels the most common presenting symptom of an enlarging ganglion is that of
radicular pain [5]. However, when occurring at the cervical and thoracic vertebral levels, 1-3 percent may initially present with signs and/or symptoms of spinal cord compression, i.e., myelopathy [6].
Case Presentation
A 60-year-old Caucasian male presented with a primary complaint of bilateral lumbosacral
and leg pain radiation, albeit predominately right-sided. Numbness on the plantar aspect of the
right foot was also present with additional complaints of ambulation-induced bilateral neurogenic
claudication. His peripheral pulses were all normal. Right straight-leg rising was limited to 30
degrees due to increasing sciatic radiculopathy. Bilateral iliopsoas muscle weakness was also
identified accompanied by reduced strength in the right foot dorsiflexors. The right ankle jerk was
absent. No long tract signs were observed. Bladder and bowel function were not impaired. Hip and
knee range of motion were both normal as well as pain-free.
A Magnetic Resonance Imaging study (MRI) was ordered, with a clinical diagnosis of spinal
stenosis and/or a midline herniated disk. Instead, the MRI revealed a large synovial cyst of the
lumbar spine, 7.0 mm x 6.7 mm x 19.0 mm, A-P and lateral as well as craniocaudal respectively,
which emerged from a degenerative right L4-L5 facet joint. The joint itself was also hypertrophic
with a minimal spondylolisthesis. Both, the ganglion cyst as well as the arthrogenic joint contributed
to the formation of severe spinal canal stenosis (Figure 1).
Figure 1
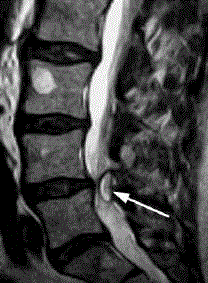
Figure 1
A 60-year-old male with an MRI of the lumbosacral spine
demonstrating a large ganglion cyst (arrow) producing a significant spinal
stenosis at L4-L5 adjacent to a degenerative, hypertrophic and unstable
right-sided facet joint.
Discussion
In 1876, Baker first described a synovial cyst in association with an adjacent vertebral
degenerative joint [6]. Although originally considered to be a relatively rare phenomenon, with
the present availability of MRI, it has proven to be a relatively more common entity. The terms
“synovial” and/or “ganglion cyst” are used interchangeably in referring to this entity. Although pathological differences between both have been described, their
slight differences, if any, are now attributed to a continuum of cyst
formation with subsequent degeneration. Synovial tissue herniation
through a weakened joint capsule forms the outer layer of the
ganglion cyst with its cavity filled with synovial joint fluid from the
adjacent vertebral joint. However, following a loss of communication
between the vertebral joint and the cyst’s cavity, myxoid degeneration
may occur [7]. The majority of patients with a symptomatic synovial
cyst experience a history of chronic lumbosacral pain preceding the
acute onset of radicular pain. Not infrequently, they may also present
without neurological deficits. Radicular pain and paresthesias, in
50-93 percent, are the most common presenting symptoms of a
synovial cyst, with neurogenic claudication the next most frequent
complaint occurring in 10-44 percent of patients [8]. A MRI is the
“gold standard” in identifying the presence of a synovial cyst [9]. This
neurodiagnostic modality can reveal both the presence of a cystic
lesion, as well its proximity to the vertebral facet joint.
Both conservative and surgical therapeutic options have been
recommended for treating a symptomatic ganglion cyst. Rest
and anti-inflammatory medication, as well as bracing, have been
recommended initially in the conservative treatment of patients
when an arthrogenic origin of pain is suspected [10]. Steroid-based
intervertebral joint injections have also been employed in treatment.
At best, these conservative measures, singularly and/or together, have
demonstrated mixed results. Slipman “et al.” [11], in a small series
of 14 patients reported that following intervertebral joint injections,
28.6 percent, i.e., four patients, had a good to excellent outcome.
However, half of the total number, i.e., seven patients, eventually
came to surgery. As Marion PJ and Kahanovitz N [12] quoting Eyster
EF and Scott WR [13] noted after a failed steroid injection in their patient with a ganglion cyst, “conservative medical treatments are
less efficacious when compared with surgical decompression and cyst
excision, which is the definitive treatment of choice” [13,14]. When
the aetiopathogenesis of this syndrome includes a significant amount
of segmental spinal instability, an arthrodesis is often considered.
However, when a surgical approach is recommended, it must always
be predicated on the individual’s symptoms, their subsequent imaging
findings and with attention to their overall health status.
References
- Métellus P, Fuentes S, Adetchessi T, Levrier O, Flores-Parra I, Talianu D, et al. Retrospective study of 77 patients harboring lumbar synovial cysts: Functional and neurological outcome. Acta Neurochir 2006;148(1):47-54.
- Freidberg SR, Fellows T, Thomas CB, Mancall AC. Experience with symptomatic spinal epidural cysts. Neurosurgery. 1994;34(6):989-93.
- Epstein NE. Lumbar synovial cysts: A review of diagnosis, surgical management and outcome assessment. J Spinal Disord Tech. 2004;17(4):321-5.
- Khan AM, Girardi F. Spinal lumbar synovial cysts. Diagnosis and management challenge. Eur Spine J. 2006;15(8):1176-82.
- Howington JU, Connolly ES, Voorhies RM. Intraspinal synovial cysts: 10-year experience at the Ochsner Clinic. J Neurosurg. 1999;91(2 Suppl):193-9.
- Baker WM. Formation of synovial cysts in connection with joints. St Bartholomews Hospital Reports 1885;21:177-90.
- Onofrio BM, Mih AD. Synovial cysts of the spine. Neurosurgery. 1988;22(4):642-7.
- Lyons MK, Atkinson JL, Wharen RE, Deen HG, Zimmerman RS, Lemens SM. Surgical evaluation and management of lumbar synovial cysts: the Mayo Clinic experience. J Neurosurg. 2000;93(1 Suppl):53-7.
- Jackson DE Jr, Atlas SW, Mani JR, Norman D. Intraspinal synovial cysts: MR imaging. Radiology. 1989;170(2):527-30.
- Mercader J, Muñoz Gomez J, Cardenal C. Intraspinal synovial cyst: diagnosis by CT. Follow-up and spontaneous remission. Neuroradiology. 1985;27(4):346-8.
- Slipman CW, Lipetz JS, Wakeshima, Howard B. Jackson. Nonsurgical treatment of zygoaphyseal joint cyst – induced radicular pain. Arch Phys Med Rehabil 2000;81(7):973-7.
- Marion PJ, Kahanovitz N. Lumbar-sacral radiculopathy secondary to intraspinal synovial cyst. Arch Phys Med Rehabil. 1995;76(11):1011-3.
- Eyster EF, Scott WR. Lumbar synovial cysts: report of eleven cases. Neurosurgery. 1989;24(1):112-5.
- Fischgrund JS, Mackay N, Herkowitz H. 1997 Volvo Award Winner in Clinical Studies: degenerative lumbar spondylolisthesis with spondylostenosis: a perspective, randomized study comparing decompressive laminectomy and arthrodesis with and without spinal instrumentation. Spine. 1997;22:2807-12.