Case Report
A Unique 8 Fr Angled Sheath Thrombectomy System for Treating Proximal Inferior Vena Cava Thrombosis
Yusaku Shibata1, Nobuaki Kobayashi1*, Masato Matsushita2, Hirotake Okazaki1, Akihiro Shirakabe1, Masamichi Takano2, Yasushi Miyauchi2, Noritake Hata1 and Wataru Shimizu3
1Department of Intensive Care Unit, Nippon Medical School Chiba Hokusoh Hospital, Chiba, Japan
2Department of Cardiovascular Medicine, Nippon Medical School Chiba Hokusoh Hospital, Chiba, Japan
3Department of Cardiovascular Medicine, Nippon Medical School, Tokyo, Japan
*Corresponding author: Nobuaki Kobayashi, Department of Intensive Care Unit, Nippon Medical School Chiba Hokusoh Hospital, 1715 Kamagari, Inzai, Chiba 270-1694, Chiba, Japan
Published: 03 Apr, 2017
Cite this article as: Shibata Y, Kobayashi N, Matsushita
M, Okazaki H, Shirakabe A, Takano
M, et al. A Unique 8 Fr Angled
Sheath Thrombectomy System for
Treating Proximal Inferior Vena Cava
Thrombosis. Ann Clin Case Rep. 2017;
2: 1318.
Abstract
We report the case of a woman with nephrotic syndrome suffering from large thrombi at the proximal Inferior Vena Cava (IVC). A percutaneous thrombectomy on the worsening IVC thrombi following optimal anticoagulant therapy was performed. Temporary IVC filter placement and subsequent direct thrombectomy via an 8 Fr angled sheath (inner lumen area = 6.51 mm2) within a 10 Fr sheath were useful, although an 8 Fr guiding catheter (inner lumen area = 4.19 mm2) was ineffective. To aspirate the large thrombus burden, a catheter with a large lumen size, such as an 8 Fr sheath, was necessary.
Keywords: Thrombectomy; Inferior vena cava; 8 Fr angled sheath
Introduction
Venous thromboembolism including deep vein thrombosis and pulmonary embolism (PE) has been identified as a considerable cause of mortality [1]. In recent years, pharmacologic anticoagulants such as intravenous unfractionated heparin, an oral vitamin K antagonist (VKA; warfarin) and non-VKA oral anticoagulants for treating venous thrombus have been established. However, when adequate anticoagulation is ineffective, percutaneous transcatheter procedures are considered as an additional treatment strategy for deep vein thrombosis [2,3].
Case Presentation
A 44-year-old woman with nephrotic syndrome was admitted to our hospital due to sudden dyspnea. Urgent contrast-enhanced computed tomography (CECT) revealed proximal inferior vena cava (IVC) thrombosis (Figure 1A) and PE (Figure 1B). A repeat CECT on the 18th hospital day after optimal anticoagulant therapy with unfractionated heparin and warfarin showed worsening proximal IVC thrombosis (Figure 1C), although PE improved (Figure 1D). After the anticoagulants proved ineffective against the IVC thrombosis, a percutaneous catheter thrombectomy was performed on the 19th hospital day. Initially, a temporary IVC filter (New House Protect, Toray Ltd., Tokyo, Japan) was placed at the retrohepatic vena cava, proximal to the thrombi, from the right jugular vein (Figure 1E) to prevent the recurrence of PE during the subsequent thrombectomy procedure. We then performed anintravenous thrombectomy with an 8Fr multipurpose guiding catheter (inner lumen area = 4.19 mm2) in an 8 Fr sheath inserted from the right common femoral vein; however, only tiny thrombi were aspirated, presumably because of the relatively small lumen size compared with the large thrombus burden. Thereafter, to create a thrombectomy system with a large lumen, we used an 8 Fr angled sheath (inner lumen diameter = 2.88 mm, inner lumen area = 6.51 mm2) 75 cm in length (Medikit Co., Ltd., Tokyo, Japan)as the thrombectomy catheter within a 10 Fr sheath that was 25 cm long (Medikit) (Figure 1F). Using this arrangement, we successfully removed the massive thrombi from the proximal IVC. Only a small burden of residual intravenous thrombi was observed on the final venography (Figure 1G), after which the IVC filter was retrieved. A CECT performed 8 days after the procedure showed that the IVC thrombi were resolved (Figure 1H) without recurrent PE (Figure 1I).
Figure 1
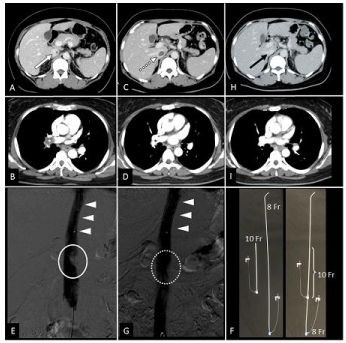
Figure 1
Contrast-enhanced computed tomography (CECT) on admission
shows (A) tiny thrombi (white arrow) at the proximal inferior vena cava (IVC)
and (B) large thrombi (white asterisk) at the proximal right pulmonary artery.
Repeat CECT on the 18th hospital day revealed (C) worsening proximal IVC
thrombosis (white dotted arrow), although (D) thrombi at the pulmonary artery
(black asterisk) were resolved. (E) Venography after placing the temporary
IVC filter (white arrowheads) showed a large thrombus burden (white circle)
at the proximal site of the IVC. (F) The percutaneous thrombectomy system
with an 8 Fr angled sheath within a 10 Fr sheath. (G) After the thrombectomy,
the thrombi decreased (white dotted circle). CECT on the 26th day revealed
(H) resolved IVC thrombi (black arrow), (I) without any evidence of pulmonary
embolism.
Discussion
In the current case, a patient with nephrotic syndrome had PE and deep vein thrombosis extending
from the renal vein to the proximal IVC. Although deep vein thrombosis is a common disease, the frequency of IVC thrombosis is relatively rare. In a previous largescale
registry including 2,119 patients with venous thromboembolism,
only 50 (2.6%) had IVC thrombosis [4]. According to US data
from 2000 to 2005, the population-based incidence of vena cava
thrombosis (either superior or inferior) diagnosis was 1.7 in 100,000
[5]. Congenital IVC abnormalities are considered the major cause of
IVC thrombosis. In patients without congenital IVC thrombosis, IVC
thrombosis is usually a result of a predisposing hypercoagulable state,
such as thrombophilia, malignancy or nephrotic syndrome [6]. In a
report investigating 512 patients with nephrotic syndrome, PE was
frequently observed (30%) and even renal vein thrombosis was not
rare (22%) in that cohort [7].
According to the European Society of Cardiology guidelines,
patients with objectively confirmed recurrent PE, despite adequate
anticoagulation treatment, are recommended to be treated with an
IVC filter, which is usually placed in the infrarenal portion of the
IVC [8]. Conversely, the latest randomized clinical trial suggested
that using a retrievable IVC filter in PE patients treated with
anticoagulation did not reduce the risk of symptomatic recurrent PE
[9]. In the present case, the patient had worsening IVC thrombosis
despite adequate anticoagulant therapies. Although IVC filter
implantation was considered as one option to prevent recurrent PE,
we decided to perform transcatheter intravenous thrombectomy
due to the lack of appropriate space to place an IVC filter (i.e. IVC
thrombi was extending proximal to the renal veins). Previous reports
described that implantation of an IVC filter at the suprarenal IVC had
a potential risk of decline in renal function [10], filter migration [11]
and fracture [12]. The temporary IVC filter was used only to prevent
procedure-related recurrent PE [2].
Several transcatheter techniques and devices have been used to
remove large IVC thrombosis. The Angio Jetthrombectomy system
(Possis Medical, Minneapolis, MN),which consists of a 6 Fr catheter,
a pump set, and a pump drive unit, was used to aspirate thrombus
debris in accordance with the Bernoulli effect [3]. The EKOS Endo
Wave infusion catheter system (EKOS Corporation, Bothell, WA),
which consists of a 5.2 Fr infusion catheter, an ultrasound core
wire, and a control unit with catheter interface cable, was used
for ultrasound-enhanced thrombolysis [13]. Another option for
the treatment of IVC thrombosis was the AngioVac aspiration
thrombectomy system (AngioDynamics, Latham, NY), which
consists of 22 Fr suction cannula, extracorporeal venovenous bypass
circuit (AngioVac circuit: an aspiration line, filter, and pump head),
and a reinfusion line [14,15]. Although some advantages have been
reported, these techniques have not been widely adopted because
the systems require specific and high-priced devices. Among devices
widely available in the clinical setting, we currently selected an 8Fr
multipurpose guiding catheter (inner lumen diameter = 2.31 mm and
inner lumen area = 4.19 mm2) and an 8Fr angled sheath (inner lumen
diameter = 2.88 mm and inner lumen area = 6.51 mm2) to aspirate
IVC thrombi. Previous reports have used an 8Fr thrombectomy
catheter (inner lumen diameter = 1.35 mm and inner lumen area =
1.43 mm2) and a 6Fr guiding catheter (inner lumen diameter = 1.80
mm and inner lumen area = 2.54 mm2) for venous thrombectomy
[16]. However, catheters with larger inner lumen size theoretically
have more advantages for treating thrombectomy, which was
demonstrated in a previous in vitro evaluation system [17]. Indeed,
an8Fr angled sheath was more effective than an 8 Fr guiding catheter
in the current case. However, using the catheter with larger lumen
might include potential risk associated with bleeding complication.
In conclusion, a catheter with a large inner lumen size, such as an 8
Fr sheath, is necessary to aspirate large IVC thrombi. A percutaneous
thrombectomy with this unique “8 Fr angled sheath within a 10 Fr
sheath” system is one option for treating large proximal IVC thrombi.
References
- Beckman MG, Hooper WC, Critchley SE, Ortel TL. Venous thromboembolism: a public health concern. Am J Prev Med. 2010;38(4):S495-501.
- Kishima H, Fukunaga M, Nishian K, Saita T, Horimatsu T, Sugahara M, et al. Aspiration thrombectomy in a patient with suprarenal inferior vena cava thrombosis. Case Rep Cardiol. 2015;2015:495065.
- El Sayed HF, Kougias P, Zhou W, Lin PH. Utility of retrievable vena cava filters and mechanical thrombectomy in the endovascular management of acute deep venous thrombosis. Vascular. 2006;14(5):305-12.
- Agnelli G, Verso M, Ageno W, Imberti D, Moia M, Palareti G, et al. The MASTER registry on venous thromboembolism: description of the study cohort. Thromb Res. 2008;121(5):605-610.
- Stein PD, Matta F, Yaekoub AY. Incidence of vena cava thrombosis in the United States. Am J Cardiol. 2008;102(7):927-9.
- Alkhouli M, Morad M, Narins CR, Raza F, Bashir R. Inferior Vena Cava Thrombosis. JACC Cardiovasc Interv. 2016;9(7):629-43.
- Zhang LJ, Zhang Z, Li SJ, Meinel FG, Nance JW, Zhou CS, et al. Pulmonary embolism and renal vein thrombosis in patients with nephrotic syndrome: prospective evaluation of prevalence and risk factors with CT. Radiol. 2014;273(3):897-906.
- Konstantinides SV, Torbicki A, Agnelli G, Danchin N, Fitzmaurice D, Galič N, et al. 2014 ESC guidelines on the diagnosis and management of acute pulmonary embolism. Eur Heart J. 2014;35(43):3033-69, 3069a-3069k.
- Mismetti P, Laporte S, Pellerin O, Ennezat PV, Couturaud F, Elias A, et al. Effect of a retrievable inferior vena cava filter plus anticoagulation vs anticoagulation alone on risk of recurrent pulmonary embolism: a randomized clinical trial. JAMA. 2015;313(16):1627-1635.
- Marcy PY, Magne N, Frenay M, Bruneton JN. Renal failure secondary to thrombotic complications of suprarenal inferior vena cava filter in cancer patients. Cardiovasc Intervent Radiol. 2001;24(4):257-259.
- Matchett WJ, Jones MP, McFarland DR, Ferris EJ. Suprarenal vena caval filter placement: follow-up of four filter types in 22 patients. J Vasc Interv Radiol. 1998;9(4):588-93.
- Ganguli S, Tham JC, Komlos F, Rabkin DJ. Fracture and migration of a suprarenal inferior vena cava filter in a pregnant patient. J Vasc Interv Radiol. 2006;17(10):1707-11.
- Owens CA. Ultrasound-Enhanced Thrombolysis: EKOS EndoWave Infusion Catheter System. Semin Intervent Radiol. 2008;25(1):37-41.
- Smith SJ, Behrens G, Sewall LE, Sichlau MJ. Vacuum-assisted thrombectomy device (AngioVac) in the management of symptomatic iliocaval thrombosis. J Vasc Interv Radiol. 2014;25(3):425-430.
- Behrens G, Bjarnason H. Venous Thromboembolic Disease: The Use of the Aspiration Thrombectomy Device AngioVac. Semin Intervent Radiol. 2015;32(4):374-378.
- Zhang QQ, Xu H, Zu MH, Gu YM, Shen B, Wei N, et al. Strategy and long-term outcomes of endovascular treatment for Budd-Chiari syndrome complicated by inferior vena caval thrombosis. Eur J Vasc Endovasc Surg. 2014;47(5):550-7.
- Hara H, Nakamura M, Komatsu H, Ikeda N, Shinji H, Makino K, et al. Comparison of the in vitro performance of 6 and 7 French aspiration catheters. Euro Intervention. 2007;2(4):487-492.