Case Report
Bochdalek Diaphragmatic Hernia Rupture in Pregnancy: A Case Report
Adriana Ioana Olaru*, I Uzochukwu, K Sheehan and R Greene
Department of Obstetrics and Gynecology, Cork University Maternity Hospital, Ireland
*Corresponding author: Adriana Ioana Olaru, Department of Obstetrics and Gynecology, Cork University Maternity Hospital, Wilton, Cork, Ireland
Published: 20 Feb, 2017
Cite this article as: Olaru AI, Uzochukwu I, Sheehan K,
Greene R. Bochdalek Diaphragmatic
Hernia Rupture in Pregnancy: A Case
Report. Ann Clin Case Rep. 2017; 2:
1275.
Abstract
Objective: Dyspnea in pregnancy and peri-partum period is a relatively common symptom,
potentially caused by a number of diseases, asthma, pulmonary infection, embolism and heart
disease. Diaphragmatic hernia is a rare cause, more likely to be misdiagnosed, with a high maternal
and fetal mortality risk; therefore, knowledge of this entity is very important.
Methods: We present the case of a nulliparous woman at 35+2 weeks gestation, with a history of
asthma, self-referred to the emergency room with upper and lower abdominal pain radiating to the
back, vomiting, tachycardia and fetal bradycardia. The ultimate diagnosis was a Bochdalek hernia
rupture.
Results: The patient was misdiagnosed initially with suspected placental abruption and underwent
an emergency caesarean section under general anesthesia, complicated by aspiration pneumonia.
Further investigations revealed the rupture of a congenital diaphragmatic hernia.
Conclusion: The differential diagnosis for severe dyspnoea in pregnancy should include
diaphragmatic hernia as a potential albeit rare cause.
Introduction
Congenital diaphragmatic hernia has an incidence of 1:2000-1:12,500 live births and accounts
for 8% of all the major congenital anomalies [1]. Bochdalek Hernia (BH) is the commonest form of congenital diaphragmatic hernia and usually a perinatal pathology. However, in the literature, there
are case reports of BH presenting in adults, with an incidence reported to be 0.17% [1]. Rupture
of a diaphragmatic hernia is a very rare, but significant complication, with an increased maternal
mortality rate (up to 10%) and fetal mortality rate (up to 13%). It normally occurs in the peripartum
period, generally because of a delayed diagnosis and requires a multidisciplinary team approach
involving obstetricians, cardiothoracic surgeons, anesthetists and radiologists [2].
Diaphragmatic hernia is classified as hiatal, congenital or traumatic, with the first being the most
common type [3]. The diaphragm development starts in the 4th weeks of gestation when the central tendinous area forms from the septum transversum, which separates the thoracic and abdominal
cavities and finishes by the 8th week with the fusion of the lumbar and costal muscle groups in the
posterolateral diaphragm. As this is the final stage of the development of the diaphragm, it represents
a vulnerable loci and it is at increased risk of a hernia formation. Complete closure occurs in the
right side before the left and this is a fact that may contribute to the left sided Bochdalek hernias [4]. Another theory would be that the liver protects the right side of the diaphragm and this is why these
hernias are more likely to occur on the left [5]. In a study by Mullins et al. a higher incidence of BH
was found in women (77%) and pregnancy was found to be the most common precipitating factor
in the rupture of a BH (34%) [6].
Adult patients presenting with BH may also have associated congenital anomalies (12%) [3].
These more common anomalies include malrotation and incomplete attachment of the caecum,
hepatic hypoplasia, bifid liver, pulmonary hypoplasia. The approach to repair the BH depends on the
presentation (emergency or elective), size and site of the defect and the presence of complications.
In recent years, there has been an increase in the use of the laparoscopic surgical approach in the
management of BH [1]. Surgical repair performed in an elective setting is the treatment of choice; the mortality in elective surgery is 5%, compared to 32% following emergency surgery.
Case Presentation
A 36 years old primiparous woman at 35+2 weeks gestation with a history of asthma using bronchodilators self referred to the emergency room with severe
generalized abdominal pain radiating to the back with vomiting.
Examination revealed a maternal heart rate of 130 beats/min and
respiratory rate of 24 cycles/min. Her abdomen was soft with nonspecific
tenderness. Fetal bradycardia of 80 beats/min was noted
on CTG. An emergency caesarean section for suspected placental
abruption was performed under general anesthesia. Significant
pulmonary aspiration occurred on induction of anesthesia and over
1 litre bilious fluid was aspirated through an oro-gastric tube. A live
male infant was delivered with no evidence of placental abruption.
Postoperatively, she was managed in the intensive care unit for
five days. A chest X-ray showed mediastinal shift to the right side with
consolidation/atelectasis of the right lower lobe (Figure 1). Initial
clinical deterioration led to increasing ventilation requirement. A
subsequent CT thorax showed jejunal and ileal loops and mesentery
displaced into the left hemithorax consistent with a large left-sided
diaphragmatic hernia (Figure 2). This was most likely congenital in
aetiology.
She was treated with broad-spectrum antibiotics for aspiration
pneumonia while intubated and sedated. Ventilatory support was
weaned over next 24 hours. Following extubation, high flow O2 and
intermittent BiPAP was commenced. Renal indices and electrolytes
remained normal. She was discharged from ICU on high flow O2.
Following review by the cardio-thoracic surgery and upper
gastro-intestinal surgery teams the decision was made to treat the
pulmonary aspiration first and the diaphragmatic hernia at a later
date. On day 12 postpartum, she was discharged home.
Ten weeks postpartum, an elective laparoscopic left hemidiaphragmatic
hernia repair was performed. There was a significant
5x5 cm posterolateral left diaphragmatic defect consistent with
Bochdalek hernia through which her entire small bowel, ascending
colon and transverse colon had herniated into the left hemithorax.
The small bowel and colon were successfully reduced into the
abdominal cavity. The defect was closed primarily and reinforced
with a Gore-Tex mesh.
Day 2 post laparoscopy, the chest X-ray demonstrated suboptimal
re-expansion of the left lung. A pigtail catheter was inserted and the
chest drain was placed on high-pressure suction. A week following
her laparoscopy, chest X-ray showed the left upper lobe had fully
re-expanded but the left lower lobe was trapped and there was a
persistent postero-lateral space which was air and fluid filled (Figure 3). Since the procedure her breathing has much improved, but the
persistent hydro-pneumothorax places her at increased risk of
pulmonary infections in the future.
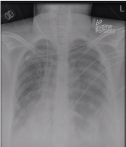
Figure 1
Figure 1
AP Portable Chest X-ray Endotracheal tube, right central venous
access in situ. Day 1 post caesarean section. Mediastinal shift to the right
side. Right lower lobe atelectasis/consolidation with patchy opacification
involving both lungs likely due to aspiration.
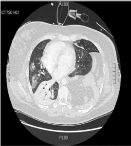
Figure 2
Figure 2
CT Thorax day 1 post caesarean section. Jejunal, ileal loops &
mesentery in left hemithorax consistent with left diaphragmatic hernia and
right mediastinal shift. Patchy ground glass opacification in both lungs with
right lower lobe consolidation likely due to aspiration.
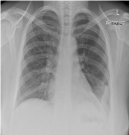
Figure 3
Figure 3
PA Chest X-ray day 7 post laparoscopic diaphragmatic hernia
repair. The left lung is now almost fully inflated with small residual loculated
hydropneumothorax in the left lower hemithorax.
Discussion
Dyspnoea in pregnancy and the peripartum period is a relatively
common symptom, potentially caused by a number of diseases
including respiratory tract infections, asthma, pulmonary embolism,
pulmonary oedema and heart disease including peripartum
cardiomyopathy. By contrast, BH is a far less common cause of peripartum
dyspnea, but its recognition is of utmost importance as it has
an increased risk of both maternal and perinatal mortality.
Pregnancy is a significant predisposing factor and when BH is
found incidentally in pregnant women, it may warrant an elective
repair, preferably in the second trimester. Frequently, these cases
present acutely with complications. CT and MRI are useful diagnostic
tools.
We present a case of a ruptured undiagnosed diaphragmatic
hernia in pregnancy. The presentation in this case suggested a
placental abruption. The clinical situation was complicated by a
pulmonary aspiration secondary to the general anesthesia, associated
with a bowel obstruction. Further investigations identified the rupture of a Bochdalek hernia and the presence of small bowel loops
in the thoracic cavity. In view of the post-operative complications,
the decision was made to stabilize the patient and treat the aspiration
pneumonia, followed by an elective laparoscopic hernia repair.
The primary repair and mesh reinforcement performed via
laparoscopy is in keeping with current practice with the associated
well established benefits. Pneumothorax has been recognized as a
potential complication following repair with a case incidence of 0.8%
[1]. In view of the high risk of complications, a multidisciplinary team
formed by obstetricians, radiologists, cardio-thoracic surgeons, upper
gastro-intestinal surgeons and anesthetists is required in these cases.
References
- Machado NO. Laparoscopic repair of Bochdalek diaphragmatic hernia in adults. N Am J Med Sci. 2016; 8: 65-74.
- Servais EL, Stiles BM, Finnerty BM, Paul S. Ruptured Diaphragmatic Eventration: A Rare Cause of Acute Postpartum Dyspnea. Ann Thorac Surg. 2012; 93: e143–e144.
- Kurzel RB, Naunheim KS, Schwartz RA. Repair of symptomatic diaphragmatic hernia during pregnancy. Obstet Gynecol. 1988; 71: 869- 871.
- Brown SR, Horton JD, Trivette E, Hofmann LJ, Johnson JM. Bochdalek hernia in the adult: demographics, presentation, and surgical management. Hernia. 2011; 15: 23.
- Dudley AG, Teaford H, Gatewood TS. Delayed traumatic rupture of the diaphragm in pregnancy. Obstet Gynecol. 1979; 53: 25-27.
- Mullins ME, Stein J, Saini SS, Mueller PR. Prevalence of incidental Bochdalek’s hernia in a large adult population. AJR Am J Roentgenol. 2001; 177: 363-366.