Case Report
Discussion of Acquired Long QT Syndrome in a Patient Being Treated for Non-Cardiac Disease
Emilio A Russo*, Hoangvy Le and Ahn-Linh D Bui
Department of Family Medicine, LSU Health Science Center New Orleans, USA
*Corresponding author: Emilio A Russo, Department of Family Medicine, LSU Health Science Center New Orleans 1542 Tulane Ave, New Orleans, LA 70112, USA
Published: 14 Feb, 2017
Cite this article as: Russo EA, Le H, Bui A-LD. Discussion
of Acquired Long QT Syndrome in a
Patient Being Treated for Non-Cardiac
Disease. Ann Clin Case Rep. 2017; 2:
1271.
Abstract
Long QT syndrome (LQTS) is a disorder that affects myocardial conduction, namely ventricular depolarization and repolarization, characterized by QT interval prolongation on an ECG. Long QT Syndrome may be either inherited or acquired with acquired being far more common. The normal QT interval is less than 440 milliseconds though this interval may be affected by both heart rate and gender. Etiologies of acquired, prolonged QT interval include electrolyte abnormalities, hypothermia, myocardial disease, elevated intracranial pressure, and prescription drugs. Many commonly used medications can cause prolongation of the QT interval, including anti-arrhythmic agents, anti-emetics, antibiotics, anti-psychotics, and anti-depressants of significance, prolongation of the QT interval may lead to Torsade de Pointes, ventricular tachycardia, and ventricular fibrillation. As such, early recognition, identification of reversible causes, including discontinuation of the offending agents, and prevention of adverse events are key to management. Beta blockers have been shown to prevent adverse cardiac events in patient who have Long QT Syndrome. Moreover, patients who are considered high risk of sudden cardiac death due to Long QT Syndrome may benefit from an implantable defibrillator.
Case Presentation
A 29-year-old Caucasian female with a history multiple prescription-drug overdoses was found
unresponsive by her family surrounded by a scattered bottle of diphenhydramine. Upon discovery
“flailing” seizure-like activity was noted by her family members. Upon arrival, EMS reported the
patient was cyanotic and hypoxic with a respiratory rate of 3-4 and oxygen saturation of 66%. In the
emergency department, she was still unresponsive and was promptly intubated. Electrocardiogram
(ECG) showed sinus tachycardia with a left bundle branch block (LBBB) and her troponin was
elevated at 0.09. At that time she was also given 6mg of lorazepam, 4 mg of ondansetron, 2 amps of
bicarbonate, and placed on a propofol drip prior to transfer to a tertiary care center.
Other findings included urine drug screen positive for benzodiazepines, cocaine, and
amphetamines, lactic acid of 10.4, and a repeat troponin of 0.21, likely due to oxygen demand and
supply mismatch. Patient was initially admitted to the ICU but was subsequently extubated shortly
thereafter. Troponin levels trended down to 0.11. Repeat ECGs showed normal sinus rhythm
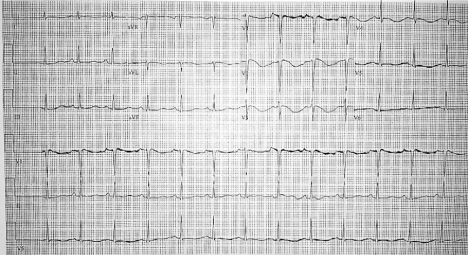
with resolution of the LBBB but persistently prolonged corrected QT interval (QTc) interval of
619 milliseconds (Figure 1). Echocardiogram showed left ventricular systolic dysfunction with an ejection fraction of 35-40% and grade 1 diastolic dysfunction. Brain natriuretic peptide was 391.
Patient was continued on ondansetron for nausea and vomiting throughout the hospital course.
Patient was confused, agitated, and both verbally and physically aggressive. She was initially
treated with lorazepam which was followed by haloperidol given persistence of above symptomology.
Soon after, ventricular complexes were noted on telemetry, followed by sustained ventricular
tachycardia and unresponsiveness. She was defibrillated twice at 200 Joules and given one dose of
amiodarone 150 mg IV. The patient subsequently converted to normal sinus rhythm, became alert,
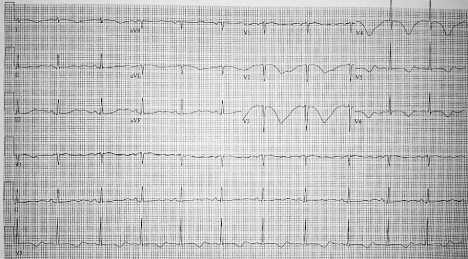
and was breathing spontaneously. Repeat ECG showed marked T wave abnormality with persistent
QT prolongation. When compared with previous ECGs, the QTc interval has lengthened to 746
milliseconds (Figure 2). Potassium level was noted to be 3.4. All medications known to prolong the QT interval were immediately discontinued.
Discussion
The QT interval on ECG represents ventricular depolarization and repolarization. This
mechanism is a complex balancing system of rapid inflow of positively charged sodium and calcium ions as well as outflow of potassium ions [1]. Malfunction and
interruptions of the flows of the ion channels can increase the time of
ventricular repolarization, which will result in prolongation of the QT
interval [2] potentially leading to life-threatening cardiac arrhythmias,
including torsade de pointes (TdP), ventricular tachycardia, and
ventricular fibrillation. Heart rate influences measurement of the QT
interval. As such, QTc is commonly used and is considered prolonged
if the interval is more than 440 ms in men and more than 460 ms in
women. Given this slight difference between sexes, women are at a
slightly higher risk of developing drug-induced LQTS and resultant
arrhythmias [2].
Many agents known to cause LQTS are commonly used, such
as ondansetron for nausea or vomiting, Macrolide antibiotics for
common bacterial infections, haloperidol for agitation, methadone
for pain or opioid abuse, and diphenhydramine or loratidine for
allergies. Anti-arrhythmics such as sotalol, amiodarone, and quinidine
have also been shown to prolong the QT interval. In the management
of LQTS, all medications that are known to prolong the QT interval
should be avoided or discontinued and electrolyte abnormalities
should be corrected. The drugs of choice for the treatment of
LQTS are beta-blockers including propranolol, natolol, atenolol,
and metoprolol. Beta-blockers have been shown to reduce the risk
of cardiac arrhythmias by blocking the adrenergic receptors, and
prevent adverse cardiac events in patients with LQTS. However, betablockers
should be used with caution in patients with bradycardia,
as this can worsen QT prolongation [3]. In high-risk patients, the
use of an implantable cardiac defibrillator (ICD) can help to prevent
sudden cardiac deaths in patients with LQTS [4]. Patients should also
be advised to refrain from competitive sports and strenuous physical activity to avoid triggering cardiac events particularly if a congenital or multifactorial LQTS is determined.
Figure 1
Figure 2
Conclusion
In our case, the following risk factors for developing prolonged QT syndrome were present prior to hospitalization: female sex and history of methadone use. During the course of her hospitalization, she received multiple agents further placing her at risk for LQTS: ondansetron, haloperidol, propofol, and, ironically, amiodorone. After the patient was coded, the above agents were discontinued and she was started on metoprolol 12.5 mg and ramipril 1.25 mg once daily. Repeat ECG showed persistent QT prolongation. It was unclear at this point whether this was congenital, drug-induced, or a combination. Patient was initially placed on a psychiatric hold at time of admission. Her psychiatric hold was subsequently lifted on the seventh day of hospitalization and patient left against medical advice two hours later. Cardiology recommended a wearable defibrillator upon discharge; however, she was lost to follow-up.
References
- Al-Khatib SM, Lapointe NM, Kramer JM, Califf RM. What clinicians should know about the QT interval. JAMA. 2003; 289: 2120-2127.
- Kannankeril P, Roden DM, Darbar D. Drug-Induced Long QT Syndrome. Pharmacological Reviews. 2010; 62: 760-781.
- Ayad RF, Assar MD, Simpson L, Garner JB, Schussler JM. Causes and management of drug-induced long QT syndrome. Proceedings (Baylor University. Medical Center). 2010; 23: 250-255.
- Khan IA. Long QT syndrome: diagnosis and management. American Heart Journal. 2002; 143.