Case Report
Laparoscopic Entry, But How?
Baris Mulayim*
Department of Obstetrics and Gynaecology, Saglik Bilimleri University, Turkey
*Corresponding author: Barıs Mulayim, Department of Obstetrics and Gynecology, Saglik Bilimleri University, Antalya Education and Research Hospital, Varlık Mh, Kazım Karabekir Caddesi, 07100 Antalya-Turkey
Published: 08 Feb, 2017
Cite this article as: Mulayim B. Laparoscopic Entry, But
How?. Ann Clin Case Rep. 2017; 2:
1262.
Abstract
Background: Safe abdominal entry in laparoscopic surgery is still debated. In patients known or
suspected to have periumbilical adhesions, open entry technique (Hasson method) or alternative
sites other than umbilicus for insertion may be chosen, Palmer’s point is the most preferred.
Method: A 27-year-old G0 P0 married women admitted to our infertility clinic for achieving
pregnancy. She had infraumbilical midline laparotomy for perforated appendicitis. On physical
exam, she had midline incision scar from umbilicus to symphysis, external genitalia, vagina,
and cervix were unremarkable. Trans-vaginal ultrasound was unremarkable, either. Blood cell
count, serum chemistry and day 3 hormonal profiles, spermiogram were within normal range.
But Hysterosalpingogram rev
ealed bilateral occlusion at tubal distal ends. For further work-up,
laparoscopy was performed.
Results: Due to midline incision and suspicion of periumbilical adhesions, open entry technique
(Hasson method) for pneumoperitoneum was preferred. No complications were occurred. After
penuemoperitoneum was achieved, laparoscopy revealed that Douglas pouch was obliterated,
bilateral fimbrial ends were not seen, whole surface of the peritoneum is covered by omentumand
the transvers colon was attached to the upper abdomen from side to side. The operation was ended
without any intervention and considered to send the patient to the ART department. The patient
was discharged at the same day.
Conclusion: The safety of laparoscopic techniques depends more on skill, education, and a clear
appreciation of the anatomy and physics of the abdominal wall than on the technique itself. It is
important that surgeons should choose the laparoscopic entry technique they are familiar with and
feel most comfortable with.
Keywords: Laparoscopy; Entry; Palmer’s point; Hassonmethod; Adhesions
Introduction
This video shows adhesions after having lower abdomen midline laparotomy. Transvers colon is attached to the upper abdomen from side to side and whole surface of the peritoneum is covered by omentum. Laparoscopic entry is tricky in this case. Abdominal entry is a prime concern for laparoscopic surgeons because at least 50% of major complications occur prior to commencement of the intended surgery hence; abdominal entry in laparoscopic surgery is still debated.The last word hasn’t said yet about the optimal way of laparoscopic entry because there are no adequate randomized clinical trials; very large numbers of patients would required in each arms and this looks impossible to be achieved. So, it is said that there is no superiority of any laparoscopic entry technique over another. We discuss the laparoscopic entry techniques especiallyin case of known or suspected periumbilical adhesions.
Case Presentation
A 27-year-old G0 P0 married women admitted to our infertility clinic for achieving pregnancy. She had infraumbilical midline laparotomy for perforated appendicitis. On physical exam, she had midline incision scar from umbilicus to symphysis, external genitalia, vagina, and cervix were unremarkable. Trans-vaginal ultrasound was unremarkable, either. Blood cell count, serum chemistry and day 3 hormonal profiles, spermiogram were within normal range. But Hysterosalpingogram revealed bilateral occlusion at tubal distal ends. For further work-up, laparoscopy was performed. Due to midline incision and suspicion of periumbilical adhesions, open entry technique (Hasson method)for pneumoperitoneum was preferred. A transverse incision is made in the sub umbilical region and the upper skin flap is retracted with Allis forceps. The lower flap is retracted using a small right-angled retractor. Subcutaneous tissue is dissected till the lineaalba and the rectus sheath is visualized. Stay sutures are taken on either side of the midline. Rectus sheath is incised in the midline along the line of lineaalba pointing upwards. A haemostat is stabbed into the peritoneum, holding the stays up. The give-way of the peritoneum can be felt as peritoneum is perforated and then the haemostat is opened to widen the opening. Finger is inserted to feel all around inside the abdominal cavity to feel any possible adhesion. Then blunt trocar-cannula inserted for the first port after visualizing the intra-peritoneal viscera. No complications were occurred. After penuemoperitoneum was achieved, laparoscopy revealed that Douglas pouch was obliterated, bilateral fimbrial ends were not seen, whole surface of the peritoneum is covered by omentum and the transvers colon was attached to the upper abdomen from side to side (Figure 1A-C). The operation was ended without any intervention and considered to send the patient to the ART department. The patient was discharged at the same day.
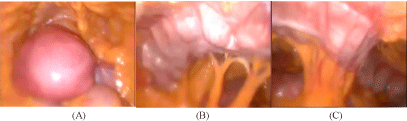
Figure 1
Figure 1
(A-C) Douglas pouch was obliterated, bilateral fimbrial ends were not seen, whole surface of the peritoneum is covered by omentum and the transvers
colon was attached to the upper abdomen from side to side.
Discussion
In our case if you had chosen Palmer’s point, you might have
injured bowel because transverse colon was attached to the upper
abdomen from side to side.
Safe abdominal entry in laparoscopic surgery is still debated.
Abdominal access of any laparoscopic surgery carries a significant risk
of bowel and vascular injuries. At least 50% of major complications
occur prior to commencement of the intended surgery [1-3]. Thus,
preventing the complications associated with initial abdominal entry
is a prime concern for laparoscopic surgeons.
The umbilicus is least likely to have omentum or bowel adhesions,
perhaps because it is usually spared at laparotomy by circumscribing
the incision to one of its sides. Also because the peritoneum is dimpled
upward in a cone-shaped configuration at the base of the umbilicus,
it is less likely that omentum and intestine will become attached and
adheres to its peritoneal surface [4].
Adhesions at the umbilical area are found in approximately 10%
of all laparoscopies. In women with no previous abdominal surgery,
umbilical adhesions are found in 0% to 0.68% of laparoscopies. 0% to
15% in women with prior laparoscopic surgery, 20% to 28% in those
who had previous laparotomy with horizontal suprapubic incision,
50% to 60% in those who had previous laparotomy with longitudinal
incision [5-8]. Current mostly used procedures are: open technique
(Hasson method), closed technique (Veress needle) and direct trocar
entry without pre-existing pneumoperitoneum.
In patients known or suspected to have periumbilical adhesions,
open entry technique (Hasson method) or alternative sites other than
umbilicus for insertion may be chosen (Palmer’s point is the most
preferred) [5,9-11].
The left upper quadrant or Palmer’s point was developed by Raoul Palmer in 1974who advocated the insertion of the Veress needle at a
range of 3 cm below the left subcostal in the midclavicular line [12].
Open entry technique (Hasson method), which is first described in
1971 by Hasson, is mainly used in high-risk patient populations such
as patients with multiple abdominal surgeries, severe endometriosis,
a history of pelvic inflamma- tory disease, or a prior tubo-ovarian
abscess.Compared with other access methods, the Hasson technique
is relatively time consuming and tends to cause a greater difficulty in
maintaining a pneumoperitoneum due to gas leakage [5,13,14].
Dingfelder first describes direct trocar entry in 1978. Direct
trocar entry is a one blind step instead of three when compared to
Veress entry, faster than any other method, near exclusion of entry
failure compared to Veress entry and above all, there is possibility of
immediate recognition of intra-abdominal iatrogenic injuries [5,15].
The Society of Obstetricians and Gynecologists of Canada
practice guideline recommends left upper quadrant (LUQ, Palmer’s)
laparoscopic entry in patients with suspected or known periumbilical
adhesions or history or presence of umbilical hernia, or after threefailed
insufflation attempts at the umbilicus. The open entry technique
may be utilized as an alternative to the Veress needle technique [5].
Also Royal College of Obstetricians and Gynecologists say that
the umbilicus may not be the most appropriate site for insertion
following previous abdominal surgery. The most usual alternative
site is the left upper quadrant, where adhesions rarely form, although
even this may be inappropriate if there had been previous surgery in
this area or splenomegaly. The Hasson method of open laparoscopic
entry is an alternative to closed laparoscopy that avoids the use of
sharp instruments after the initial skin incision [5,9].
In the regard of laparoscopic entry techniques, latest Cochrane
review says there is insufficient evidence to recommend one
laparoscopic entry technique over another. An open-entry technique
is associated with a reduction in failed entry when compared to
a closed-entry technique, with no evidence of a difference in the
incidence of visceral or vascular injury. An advantage of direct trocar
entry over Veress needle entry is noted for failed entry and vascular
injury [16].
Conclusion
This is a dilemma whether to choose Palmer’s point entry or
Hasson method entry in case of known or suspected periumbilical
adhesions. We just want to emphasize or take into consideration that
as in our case Palmer’s point is not 100% safe like the other methods,
as well. The surgeons all over the world should keep in mind this case.
Although several articles have been written on the safest, quickest,
and easiest method, the current literature fails to provide a fail-proof
or risk-free method of entering the peritoneal cavity at laparoscopy.
The safety of these techniques depends more on skill, education, and
a clear appreciation of the anatomy and physics of the abdominal
wall than on the technique itself. It is important that surgeons should
choose the entry technique they are familiar with and feel most
comfortable with.
References
- S Krishna Kumar, P Tambe. Entry Complications in Laparoscopic Surgery. J Gynecol Endosc Surg. 2009; 1: 4-11.
- Jansen FW, Kapiteyn K, Trimbos-Kemper T, Hermans J, Trimbos JB. Complications of laparoscopy: a prospective multicentre observational study. Br J Obstet Gynaecol. 1997; 104: 595-600.
- Jansen FW, Kolkman W, Bakkum EA, de Kroon CD, Trimbos-Kemper TC, Trimbos JB. Complications of laparoscopy: an inquiry about closed versus open-entry technique. Am J Obstet Gynecol. 2004; 190: 634-638.
- Roy GM, Bazzurini L, Solima E, Luciano AA. Safe technique for laparoscopic entry into the abdominal cavity. J Am Assoc Gynecol Laparosc. 2001; 8: 519- 528.
- Vilos GA, Ternamian A, Dempster J, Laberge PY, The Society of Obstetricians and Gynaecologists of Canada. Laparoscopic entry: a review of techniques, technologies, and complications. J Obstet Gynaecol Can. 2007; 29: 433-465.
- Audebert AJ, Gomel V. Role of microlaparoscopy in the diagnosis of peritoneal and visceral adhesions and in the prevention of bowel injury associated with blind trocar insertion. Fertil Steril. 2000; 73: 631-635.
- Levrant SG, Bieher EJ, Barnes RB. Anterior abdominal wall adhesions after laparotomy or laparoscopy. J Am Assoc Gynecol Laparosc. 1997; 4: 353- 356.
- Brill A, Nezhat F, Nezhat CH, Nezhat C. The incidence of adhesions after prior laparotomy: A aparoscopic appraisal. Obstet Gynecol. 1995; 85: 269- 272.
- Royal College of Obstetricians and Gynecologists. Green-top Guideline No. 49. Preventing Entry-Related Gynecological Laparoscopic Injuries. London: RCOG; 2008.
- Frappell J. Laparoscopic entry after previous surgery. The Obstetrician & Gynecologist. 2012; 14: 207-209.
- Jongrak Thepsuwan, Kuan-Gen Huang, Muliati Wilamarta, Aizura- Syafinaz Adlan, Vahan Manvelyan, Chyi-Long Lee. Principles of safe abdominal entry in laparoscopic gynecologic surgery. Gynecology and Minimally Invasive Therapy. 2013; 2: 105-109.
- Palmer R. Safety in laparoscopy. J Reprod Med. 1974; 13: 1-5.
- Hasson HM. A modified instrument and method for laparoscopy. Am J Obstet Gynecol. 1971; 110: 886-887.
- Dingfelder JR. Direct laparoscopic trocar insertion without prior pneumoperitoneum. J Reprod Med. 1978; 21: 45-47.
- Molloy D, Kalloo PD, Cooper M, Nguyen TV. Laparoscopic entry: a literature review and analysis of techniques and complications of primary port entry. Aust NZJ Obstet Gynaecol. 2002; 42: 246-254.
- Ahmad G, Gent D, Henderson D, O'Flynn H, Phillips K, Watson A. Laparoscopic entry techniques. Cochrane Database Syst Rev. 2015; 8: CD006583.