Clinical Image
Complex Case of Methicillin Resistant Staphylococcus aureus Occipital Osteomyelitis and Subdural Empyema: Vancomycin or Linezolid?
Dalvir Gill1*, Natasha Sheikh2 and Waleed Javaid3
1Department of Internal Medicine, SUNY Upstate Medical University, USA
2Department of Internal Medicine, Ross University School of Medicine, USA
3Department of Infectious Disease, SUNY Upstate Medical University, USA
*Corresponding author: Dalvir Gill, Department of Internal Medicine, SUNY Upstate Medical University, 750 East Adams Street, Syracuse, NY, 13210, 60 Presidential Plaza, Apartment 1104, Syracuse, 13202, USA
Published: 03 Feb, 2017
Cite this article as: Gill D, Sheikh N, Javaid W. Complex
Case of Methicillin Resistant
Staphylococcus aureus Occipital
Osteomyelitis and Subdural Empyema:
Vancomycin or Linezolid?. Ann Clin
Case Rep. 2017; 2: 1256.
Clinical Image
Methicillin-resistant staphylococcus aureus (MRSA) is typically considered a nosocomial
pathogen, however it has now emerged to cause infections in the community. We report a case of
MRSA bacteremia with subdural empyema and occipital osteomyelitis in a female with a history of
significant intravenous drug use (IVDU). There are very few reports on MRSA bacteremia leading
to problems with central nervous system (CNS) involvement.
27-year-old female with past medical history significant for IVDU presented to emergency
department with neck pain, and occipital headache for 1 week. She admitted to recent heroin use.
Her vitals were significant for, blood pressure of 102/67 mm Hg, pulse of 116 beats per minute,
temperature 36.9°C (oral), respiratory rate of 19 breaths per minute, oxygen saturation of 96% on
room air. Physical exam was remarkable for left shoulder hematoma and track marks bilaterally on
arms. WBC count was with normal range. Blood cultures grew MRSA, susceptible to vancomycin.
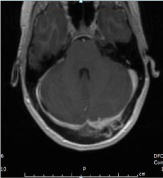
Trans-esophageal echocardiogram showed 6.9 mm tricuspid valve vegetation. MRI brain showed
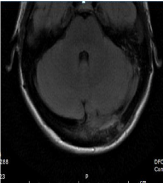
left subdural empyema (Figure 1) and associated osteomyelitis within the overlying occipital
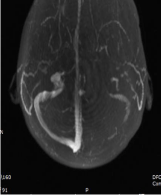
bone (Figure 2). MRI head showed left transverse sinus thrombosis extending superiorly into an
occipital lobe cortical vein with evidence of collateralization of flow within the overlying occipital
bone (Figure 3). Neurosurgery did not recommend any surgical intervention. Follow up head
MRI showed decrease in the size of the subdural empyema. Patient completed 6-week course of
vancomycin and her symptoms improved.
The patient in our case report developed bacteremia from MRSA due to significant IVDU and it
had disseminated into the central nervous system. Treating CNS disease due to MRSA is challenging
because of few therapeutic options, and difficulty in attaining therapeutic concentration of the
drug in cerebrospinal fluid (CSF). Vancomycin is the main treatment, however in some patients
vancomycin therapy fails because of its poor CSF penetration [1]. There are some cases where linezolid has been successful, due to its greater CSF penetration [2,3].
Even though there are many CNS diseases occurring from MRSA, it
is rare to find CNS disease development from community acquired
MRSA. Hence, clinicians should have a high index of suspicion
for subdural empyema in IVDUs who present with headaches and
neck pain. Recognition and treatment of subdural empyema as a
complication of bacteremia in IVDU is very important due to its
complication rate. As evident in this case, thrombosis of the venous
sinus can lead to venous occlusion and sometimes even brain
infarction. Surgical and/or medical treatment should not be delayed.
Figure 1
Figure 2
Figure 3
Figure 3
MRI head showing left transverse sinus thrombosis, extending
superiorly into an occipital lobe cortical vein with evidence of collateralization
of flow within the overlying occipital bone.
References
- Kessler AT, Kourtis AP. Treatment of meningitis caused by methicillinresistant Staphylococcus aureus with linezolid. Infection. 2007; 35: 271-274.
- Saito N, Aoki K, Sakurai T, Ito K, Hayashi M, Hirata Y, et al. Linezolid treatment for intracranial abscesses caused by methicillinresistant Staphylococcus aureus – two case reports. Neurol Med Chir (Tokyo). 2010; 50: 515-517.
- Naesens R, Ronsyn M, Druwé P, Denis O, Ieven M, Jeurissen A. Central nervous system invasion by community-acquired methicillinresistant Staphylococcus aureus. J Med Microbiol. 2009; 58: 1247-1251.