Case Report
Temporalis Muscle Rotation to Reconstruct the Palatal Defect Following Maxillectomy in a Three Months Old Infant
Devaraja K, Kapil Sikka*, Alok Thakar and Rachna Seth
Department of Otorhinolaryngology, All India Institute of Medical Sciences, India
*Corresponding author: Kapil Sikka, Department of
Otorhinolaryngology, All India
Institute of Medical Sciences, New
Delhi-110029, India/p>
Published: 27 Jan, 2017
Cite this article as: Devaraja K, Sikka K, Thakar A,
Seth R. Temporalis Muscle Rotation
to Reconstruct the Palatal Defect
Following Maxillectomy in a Three
Months Old Infant. Ann Clin Case Rep.
2017; 2: 1248.
Abstract
Background: Rehabilitation following maxillectomy has been a challenging aspect of surgical
management of sinonasal pathology. In here, we are reporting a novel technique of successful
rehabilitation of maxillectomy defect in a three months old infant in which neither obturator nor
could free flap have been useful for closure of the palatal defect.
Case Report: Three months old male infant with Melanotic Neurectodermal tumor of infancy
of maxilla underwent maxillectomy with excision of tumor and the resultant palatal defect was
closed primarily by rotation of mobilised temporalis muscle flap. Infant had uneventful and early
functional recovery with resumption of oral feeds on day four.
Conclusion: Temporalis muscle flap is a novel and promising technique for reconstruction after
maxillectomy, with advantages of early oral feeding. In addition, it may reduce the risk of recurrence
by enabling radical excision, which otherwise would not have been possible without reliable
rehabilitation.
Introduction
Rehabilitation following maxillectomy is intriguing. The altered anatomy and physiology following maxillectomy is likely to shackle the overall quality of life by vexing the swallowing and speech of the individual, if not appropriately rehabilitated. Though the present consensus is divided onto what remains ideal rehabilitative option following maxillectomy, the trend is slowly shifting from contemporary prosthetic obturators towards much promising free flaps. In this case report we present a unique scenario of successful rehabilitation of palatal defect following maxillectomy in a three months old infant, in which, neither obturator nor free flap could have been useful for closure of the palatal defect. Reconstruction of palate with temporalis muscle rotation flap has earlier been vastly described in adults, nevertheless, to our knowledge such a reconstruction in such young infant has not been done or reported in literature. Discussion also includes relevant literature review and detailed account into the need for such a reconstruction.
Case Presentation
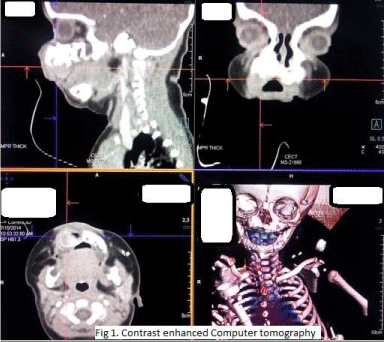
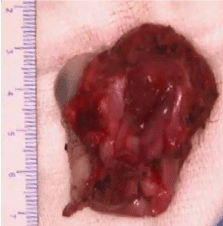
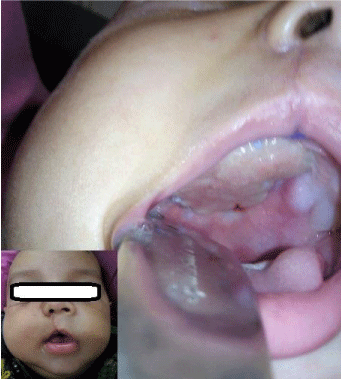
Three months old male infant was referred to our centre with a progressive swelling in the right cheek since birth. On examination, the infant had an ill-defined swelling in right canine fossa of size 3x3 cms, which was hard in consistency, with normal overlying skin and had extended into the right side of hard palate as mucosa covered bulge. Rest of head and neck examination was normal. Contrast enhanced computer tomographic scan showed heterogeneous enhancing solid tumor arising from anterior-lateral wall of maxilla, with dense calcification, destruction and scalloping of bone as in Figure 1. It was diagnosed as Melanotic Neuroectodermal tumor of infancy (MNTI), based on histological and immunohistochemical characteristics of the biopsy specimen. Patient underwent surgical resection under general anaesthesia. Taking adequate margins all around, total maxillectomy was performed with appropriate bony cuts to remove whole of the tumor, as in Figure 2. The resultant palatal defect was primarily reconstructed by temporalis muscle rotation flap. By a separate incision temporalis muscle flap was raised, rotated and tunnelled through the subcutaneous flap in order to cover the maxillectomy defect as depicted in Figure 3. Infant had an uneventful postoperative recovery with well healing of the wound as shown in Figure 4. ‘Oral sips on demand’ were resumed as early as day four following surgery. Feeding nasogastric tube was removed on postoperative day seven. The infant was able to maintain hydration and nutrition on oral feeds without any nasal regurgitation or suckling issues. Histopathology examination of surgical specimen showed negative margins.
Figure 1
Figure 2
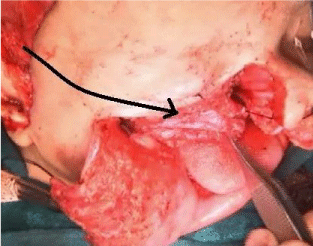
Figure 3
Figure 3
Intraoperative picture after excision of tumor, showing direction
and arc of rotation of temporalis muscle to cover palatal defect.
Figure 4
Discussion
“MNTI is a rare, benign but locally aggressive tumor including
gradual invasion of surrounding structures [1]’’ and “it is said to
have originated from neural crest [2]”. “Surgical excision is the
treatment of choice and the role of chemotherapy is limited to
some malignant and metastatic disease [3]”. Also, these tumors have
considerable recurrence rate that varies between 10-60% and “15% of
recurrence occurs within 4 weeks of surgery [2]”. There is a risk for
malignant transformation of 6.6%. Nevertheless, most of the reports
have mentioned either “sub-radical excision or curettage of these
tumors in order to minimise morbidity [4,5]” arising out of surgical
excision, which can be a principal reason for increased recurrence
rates. The idea behind the such an approach is to prevent the grievous
consequence of maxillectomy in an infant, which unrelentingly affects
feeding, and indirectly strangles the infant`s nutrition, immunity
as well as overall development. In general, infants are not ideal for
palatal obturators nor are they considered for composite free flaps,
the standard alternatives for reconstructing palatal defects in adults.
The essence of primary reconstruction of palatal defect lies in the
fact that not only it spares the infant from morbidity of maxillectomy,
but also snubs the recurrence rate by inculcating surgeon for radical excision of primary tumor, instead of mere curettage. In
the index case, planning of reconstruction with rotation flap was
made preoperatively; enabling the complete excision of tumor with
adequate margin by total maxillectomy and then, the resultant palatal
defect was reconstructed by temporalis muscle rotation flap based
on deep temporal artery. The current reconstruction option is much
preferable to either an obturator or a free flap both of which would
pose major difficulties in execution in an infant. With growth and
dentition it would be possible for the child to masticate and chew
from the contralateral side. Further, if future needs so demand, there
are always the options of subsequent obturator or of flap with dental
implants at a later date.
Primary reconstruction following surgical resection of tumor has
itself been debatable. It is said that primary closure of the surgical
defect can hamper an early detection of recurrence, but in a three
month old, clinical examination even with nasal endoscopy has little
bearing on decision making and “most of the surgeons or oncologists
rely on radiological evidence” [6]. One might as well go on to argue
that second stage reconstruction after histopathological confirmation
of free margins and a disease free follow up of few weeks can be good
alternative approach. Nevertheless, the present approach of primary
reconstruction possibly avoids second general anaesthesia in an
infant and can account for even those unfortunate ones, who might
not follow up in later date. Moreover as mentioned earlier, reliable
reconstruction ensures radical excision, minimising the possibility of
margins involvement and/or recurrence.
Another argument can question the need for any surgical reconstruction at all in these cases, considering the fact that the cleft
palate cases are managed conservatively until certain age and most of
these cases do well. Yet one must understand that the advocated delay
in cleft palate repair is due to development and maturation issues of
eustachian tube muscles, which is not the senario in a maxillectomee
infant. Also the pathophysiology in cleft palate is different from
palatal defect following maxillectomy and even so in cleft palate
cases, there is invariable need for surgical correction as earlier as the
conditions deemed feasible.
Conclusion
In conclusion, for rehabilitating maxillectomee infants, primary reconstruction of palatal defect with temporalis muscle rotation flap is a good option for early oral feeding, with specific advantages.
References
- Bangi BB, Tejasvi ML. Melanotic neuroectodermal tumor of infancy: A rare case report with differential diagnosis and review of the literature. rare case report with differential diagnosis and review of the literature. Contemp Clin Dent. 2012; 3: 108-112.
- Gaiger de Oliveira M, Thompson LD, Chaves AC, Rados PV, da Silva Lauxen I, Filho MS. Management of melanotic neuroectodermal tumor of infancy. Ann Diagn Pathol. 2004; 8: 207-212.
- Mendis BR, Lombardi T, Tilakaratne WM. Melanotic neuroectodermal tumor of infancy: a histopathological and immunohistochemical study. J Investig Clin Dent. 2012; 3: 68-71.
- Neven J, Kaa CH der, Groot-Loonen J, de Wilde PCM, Merkx MAW. Recurrent melanotic neuroectodermal tumor of infancy: a proposal for treatment protocol with surgery and adjuvant chemotherapy. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008; 106: 493-496.
- Tan O, Atik B, Ugras S. Melanotic neuroectodermal tumor in a newborn. Int J Pediatr Otorhinolaryngol. 2005; 69: 1441-1444.
- Hamilton S, Macrae D, Agrawal S, Matic D. Melanotic neuroectodermal tumour of infancy. Can J Plast Surg. 2008; 16: 41-44.