Case Report
Peripheral Adenomatoid Odontogenic Tumor: A Rare Case Report
Sasankoti Mohan Ravi Prakash*, Gargi Vidisha, Kamarthi Nagaraju, Malik Sangeeta and Gupta Swati
Department of Oral Medicine and Radiology, Subharti Dental College, India
*Corresponding author: Sasankoti Mohan Ravi Prakash, Department of Oral Medicine and Radiology, Subharti Dental College, Meerut, Uttar Pradesh, India
Published: 13 Jan, 2017
Cite this article as: Prakash SMR, Vidisha G, Nagaraju
K, Sangeeta M, Swati G. Peripheral
Adenomatoid Odontogenic Tumor: A
Rare Case Report. Ann Clin Case Rep.
2017; 2: 1235.
Abstract
Odontogenic tumors are a group of heterogeneous lesions, features of which have been catalogued for several decades. Adenomatoid Odontogenic Tumor (AOT) is a relatively rare and distinct odontogenic tumor that is exclusively odontogenic epithelium in origin often misdiagnosed asanodontogenic cyst. It is slow growing, benign in nature that appears in the anterior portion of the jaws and more frequently in the anterior maxilla. Histogenesis of AOT is still unclear and is often considered as a hamartomatouslesion rather than a true neoplasm. It occurs in intraossoous as well as peripheral forms. Perepheralvariantis very rare and only few reports have been published. We report a rare case of AOT of the maxilla in a 19-year-oldfemale patient having both peripheral as well as central component, which is rare in literature.
Keywords: Adenomatoid odontogenic tumor; Benign; Peripheral; Dentigerous cyst
Introduction
Adenomatoid Odontogenic Tumor (AOT) is rightfully called master of disguise. It is a benign
(hamartomatous), non-invasive lesion, with a slow but progressive growth. It occurs in intraosseous
as well as extraosseous forms. AOT accounts for 2.2% to 7.1% of all odontogenic tumors [1].
The central AOT accounts for approximately 96% of all AOTs of which 71% are the follicular
type. It was first documented in literature by Steensland in 1905 as epitheliomaadamantinum
[2]. Unal et al. [3] produced a list containing all nomenclatures for AOT reported in the
literatures. A variety of term has been used to describe this tumor like adenoameloblastoma,
ameloblastoma, ameloblasticadenomatoid tumor, adamantinoma, epitheliomaadmentinum or
teratmatousodontoma. Philipsen and Birn proposed the widely accepted and currently used name
AOT, which was adopted by the World Health Organization classification of odontogenic tumors in
1971 [4]. In 2005, the histologic typing of odontogenic tumors, jaw cysts and allied lesions by World
Health Organization (WHO) has defined AOT as a tumor of odontogenic epithelium with duct like
structures and with varying degree of inductive changes in the connective tissue. The tumor may
be cysticin its presentation or solid areas in some lesion may be present as nodules in the capsule of
large cysts [5].
It usually affects young patients, mostly during their second decade of life. There is a tendency
to affect females (male : female ratio 1 : 2) and to occur in the anterior maxillary region [6]. It often causes expansion of surrounding bone and displacement of adjacent teeth [7]. However, due to the
slow-growing nature of the lesion the patients tolerate the swelling for years until it produces an
obvious deformity [8]. The tumor is usually associated with unerupted teeth, frequently canines or lateral incisors [9]. In this case report, we presented an AOT causing swelling in the anterior maxillary alveolar process with labial and palatal expansion on right side.
Case Presentation
A 19-year-old female presented with slow growing, painless swelling in the right upper jaw
for six months. The swelling had gradually increased in size with no associated pain, discharge
or numbness. There was no history of trauma, pain, discharge or any other swelling in the body.
Extra-oral physical examination revealed a single swelling in the left anterior maxillary region giving
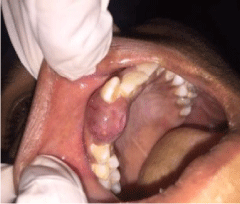
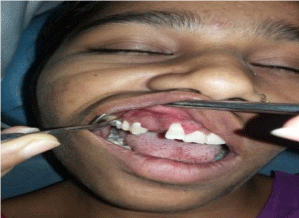
a local raised lip appearance. Intra-oral examination revealed a solitary well-circumscribed firm
growth measuring about 2 cm × 2 cm on right maxillary alveolus in relation to teeth 12 and 13
(Figure 1). There was spacing present between 12 and 13. Grade I mobility was present long with
labial displacement in relation to 12. On palpation, the swelling was firm and non-tender, showed no evidence of discharge on digital pressure. Based on the history and
clinical features, a provisional diagnosis of lateral periodontal cyst
was made. Differential diagnosis considered were peripheral giant
cell granuloma and peripheral variant of Keratocystic odontogenic
tumor and AOT.
The patient was subjected for radiographic investigations:
Intraoral peri-apical radiograph (IOPA) of the left maxillary anterior
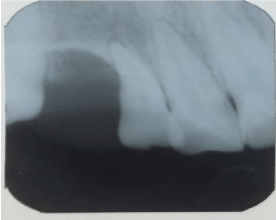
region. IOPA showed arch-like (cup-shaped) resorption of alveolar
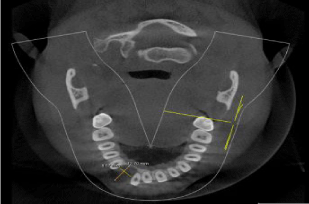
bone in relation to 12 and 13 (Figure 2). CBCT evaluation on the
axial section showed a well defined radiolucecy between 12 and 13,
measuring 8.57mm mesiodistally and 12. 70 mm buccolingually
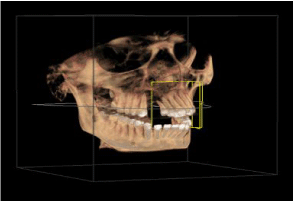
(Figure 3). Figure 4 showing the alveolar bone loss in 3D view.
Pre-operatively, a single fluid-filled sac was seen in right maxillary
alveolus. Fine needle aspiration yielded only blood. The patient
underwent surgical curettage (enucleation) under local anesthesia in
outpatient department of our institute and the samples were sent for histopatologic examination.
Gross examination of the specimen showed a single reddishbrown
soft tissue measuring 1.5 cm x 2 cm. Cut section revealed a cyst with
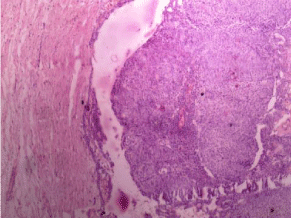
wall thickness of 0.1-0.5 cm. Microscopy revealed fibrous cyst wall
lined by solid nodules of cuboidal / columnar epithelial cells forming
nests / rosette like structure with minimal connective tissue stroma.
In between the rosette-like areas eosinophillic amorphous materials
suggestive of tumor droplets and several areas of calcification are
evident (Figure 5). The overall features were suggestive of AOT. Thus,
the final diagnosis of peripheral variant of AOT was obtained. Patient
is asymptomatic after 7 months of follw-up (Figure 6).
Figure 1
Figure 2
Figure 2
Intraoral periapicalradiograph showed radiolucency with arch
shape bone loss between 12 and 13.
Figure 3
Figure 4
Figure 5
Figure 5
H&E pictomicrograph 40X showing thinanastomosing strands of
epithelial cells plexiform pattern.
Figure 6
Discussion
Adenomatoid Odontogenic Tumors (AOTs) are unique odontogenic lesions located either centrally within the jaws or peripherally in the soft tissue overlying the tooth-bearing area. It represents 3-7 % of all odontogenic tumors [10]. Some authors consider AOTs to be true benign, non-aggressive noninvasive neoplasms, whereas others view them as developmental hamartomatous odontogenic growths. It is sometimes referred to as ‘two-third tumor’ because it occurs in the maxilla in about two-third cases, about two-third cases arise in young females, two-third cases are assoiated with an unerrupte tooth, and two-third affected teeth are canines [11].The peripheral AOT (PAOT) is still by far the most rare type constituting only 4.4% of all AOT cases [12]. According to Philipsen and Reichart, the AOT appears in three clinic- radiographic variants: follicular (pericoronal), extrafollicular (extracorporeal) and peripheral (extraosseous). The follicular and extrafollicular variants are both intrabony and account for approximately 96% of all AOTs [6,13,14]. The follicular type is a central intraosseus lesion associated with an impacted tooth, while extrafollicular intraosseus AOT has no relation with an unerupted tooth. The peripheral variant appears as a gingival fibroma or epulis attached to the labial gingival. PAOT has a surprisingly high female predilection in the ratio of 2:1 [15]. Maxilla is swven times more affected than mandible [15]. Peak incidence is seen at 12 years (9-17 years), these are mostly manifested on the labial aspect of maxillary teeth, more commonly in relation to the incisors [13]. The clinical differential diagnosis ranges from fibrous epulis, pyogenic granulomas, peripheral giant cell granulomas, and the peripheral ossifying fibromas to the rarer connective tissue neoplasm like fibromas, neurofibromas and peripheral odontogenic neoplasms. Although there are no pathognomonic radiographic findings, it has a tendency to cause periodontal bone loss or a well defined deep bony pocket, which was observed in the present case. It usually manifests with the displacement of the teeth that was evident in our case on the IOPA. AOT clinically appearing as epulis, show a deep punched out moat like bony defect of the periodontal space. Whether these are follicular/extrafollicular AOTs that originated intraosseously and erupted along with the related tooth and finally assumed a peripheral position or lesions with denovo peripheral origin, is still a question [16]. Our case also belongs to this category of un-identifiable origin, named by Philipsen as hybrid variant. Similar cases have been recently reported by Jham et al. [1] and N Lavanya et al. [17] having features of central lesion and peripheral presentation. AOTs macroscopically appear as a soft, roughly spherical mass with a distinct fibrous capsule. Upon gross sectioning, the cut surface shows a variegated appearance with small areas of hemorrhage in a grayish-white tissue. Small or large cystic spaces may be present and these may contain yellowish gelatinous material or blood-stained fluid. In some cases, the tumour may be almost entirely cystic. A tooth or teeth may be embedded in the tumour or attached to it [14,18].There is little variation in the histopathology of a peripheral AOT compared with an intraosseous AOT- proliferation of odontogenic epithelium with variable-sized duct-like structures and solid nodules of cuboidal or columnar cells that are encapsulated by thin connective tissue, with a vascular stroma and diffuse calcifications- although there is some evidence to suggest that extraosseous lesions are unencapsulated more frequently [16]. The peripheral odontogenic tumours are generally indolent. This benign biologic behaviour appears to be true for the PAOTs too. So, a conservative excision with adequate margins seems to be the treatment of choice. As reported in the literature, in the present case, the lesional tissue was also easily separated from the overlying mucosa [16,19]. The very few peripheral AOT cases have been reported to draw definite conclusions on biologic behaviour.
Immunhistological Features
During the last few years several studies have been published dealing with the immunhistological properties of AOT. Immunohistochemically, the classical AOT phenotype is characterized by a cytokeratin (CK) profile similar to follicular cyst and/or oral or gingival epithelium based on positive staining with CK5, CK17 and CK19 [13]. On the other hand the classical AOT is negative for CK4, 10, 13 and 18.
Conclusion
Thus, based on currently available evidence and the findings in the present case we emphasize that extraosseous/peripheral variant of AOT is very rare. Here, we have discussed the clinical, radiographic and histopathologic features of a case of peripherally occurring AOT, which involved right anterior maxilla of a young female. It was initially diagnosed as lateral periodontal cyst and was conservatively surgically enucleated. The final diagnosis of an AOT was arrived by histologic examination of the excised tissue specimen. Recurrence of AOT is exceptionally rare. Hence, the prognosis is excellent.
References
- Jham BC, Passos JB, Do Carmo MAV, Gomes CO, Mesquita RA. Oral Oncology EXTRA. 2006; 42: 268-271.
- Steensland HS. Epithelioma adamantinum. J Exper Med. 905; 6: 377-389.
- Unal T, Centingul E, GunbaynT. Periherladenomatoid odontogenic tumor: Birth of a term. J ClinPediatric Dent. 1995; 19: 139-142.
- Philipsen HP, Birn H. The adenomatoid odontogenic tumor, ameloblastic adenomatoid tumor or adeno-ameloblastoma. Acta Pathol Microbiol Scand. 1969; 75: 375-398.
- Philipsen HP, Reichart PA, Nikai H. The Adenomatoid Odontogenic Tumour (AOT): An Update. J Oral Pathol Med. 1997; 2: 55-60.
- Philipsen HP, Reichart PA. Adenomatoidodontogenictumour: Facts and Þ gures. Oral Oncol. 1999; 35: 125-131.
- Bravo M, White D, Miles L, Cotton R. Adenomatoid Odontogenic Tumor Mimicking a Dentigerous Cyst. Int J Pediatr Otorhinolaryngol. 2005; 69: 1685-1688.
- Olgae V, Koseoglu BG, Kasapoglu C. Adenomatoidodontogenic Tumor: A Report of an Unusual Maxillary Lesion. Quintessence Int. 2003; 34: 686- 688.
- Dayi E, Gurbuz G, Bilge OM, Ciftcioglu MA. Adenomatoid Odontogenic Tumor (Adenoameloblastoma): Case Report & Review of Literature. Aust Dent J. 1997; 42: 315-318.
- Kumar R, Singh RK, Pandey RK, Mohammad S. Peripheral Odontogenic Tumor:Report of a Rare Case. J Oral Biol Craniofac Res. 2012; 2: 57-60.
- Marx RE, Stern D. Oral and Maxillofacial Pathology a rationale for Diagnosis and Treatment. Quintessence Publishing. 2002.
- Balwani SR, Barpande SR, Tupkari J. Peripheral Adenomatoid Odontogenic Tumor. J Oral Maxillofacial Pathol. 2007; 11: 28-31.
- Philipsen HP, Samman N, Ormiston IW, Wu PC, Rcichart PA. Variants of the Adenomatoid Odontogenic Tumor with a Note on Tumor Origin. J Oral Pathol Med. 1992; 21: 348-352.
- Reichart PA, Philipsen HP. Adenomatoid Odontogenic Tumor and Allied Lesion, Quintessence Publishing. 2004.
- Ide F, Mishima K, Saito I, Kusama K. Rare Peripheral Odontogenictumours: Report of 5 Cases and Comprehensive Review of the Literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008; 106: e22-e28.
- Curran AE, Miller EJ, Murrah VA. Adenomatoid Odontogenic Tumor Presenting as Periapical Disease. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1997; 84: 557-560.
- Lavanya N, Rajeshwari MRC, Bharathi R, Shaheen A. Peripheral Adenomatoid Odontogenic Tumour - Is it Really Peripheral?: A Case Report. J Clin&Diag R. 2013; 7: 1524-1526.
- Rick GM. Adenomatoid Odontogenic Tumor. Oral Maxillofac Surg Clin North Am. 2004; 16: 333-354.
- Kearns GJ, Smith R. Adenomatoid Odontogenic Tumour: An Unusual Cause of Gingival Swelling in a 3-Year-Old Patient. Br Dent J. 1996; 181: 380-382.