Case Report
Oropharyngeal Metastasis from Papillary Thyroid Carcinoma: A Rare Event
Neyaz A, Husain N*, Shukla S, Arora A and Verma V
Department of Pathology, Dr. Ram Manohar Lohia Institute of Medical Sciences, India
*Corresponding author: Nuzhat Husain, Department of Pathology, Dr. Ram Manohar Lohia Institute of Medical Sciences, Lucknow-226010, India
Published: 05 Dec, 2016
Cite this article as: Neyaz A, Husain N, Shukla S, Arora A,
Verma V. Oropharyngeal Metastasis
from Papillary Thyroid Carcinoma: A
Rare Event. Ann Clin Case Rep. 2016;
1: 1201.
Abstract
Metastatic oral malignancy accounts for 1% of all oral cancers. Primary tumor sites are lung, kidney, liver, breast, female genital organs and colo-rectum. Metastasis from thyroid carcinoma to the oropharynx is very rare. Papillary thyroid carcinoma (PTC) favors lymphatic spread. Hematogenous spread rarely occurs to the lung, bones and brain. We report a rare case of a 36 year old female in whom metastatic lesion from papillary thyroid cancer presented 13 years after treatment of the primary, as an oropharyngeal mass clinically mimicking a second malignancy. CT scan revealed a mass lesion arising from posterior wall of oropharynx, partially extending over posterior wall of hypopharynx at the metastatic site, with a large primary in the left lobe of thyroid involving larynx. Histology showed a papillary adenocarcinoma which expressed CK7, thyroid transcription factor 1 (TTF1) and thyroglobulin. The review details metastasis in the oro-pharynx, metastatic sites of thyroid malignancies, more specifically differentiated thyroid carcinomas and their prognostic significance. Issues in histopathology, diagnosis of the lesion including distinguishing it from a primary PTC in a thyroglossal cyst or a lingual thyroid, differential diagnosis of other papillary lesions, interesting collision tumours are discussed. Furthermore the mechanism of lymphatic spread to oropharynx and the radiological diagnosis of metastasis and treatment strategies have been outlined.
Keywords: Oropharynx; Metastasis; Papillary thyroid carcinoma
Introduction
Metastatic oral malignancy accounts for 1% of all oral cancers [1]. Primary sites of metastasis are lung, kidney, liver, breast, female genital organs and colo-rectum [2-3]. Metastasis from thyroid malignancies to this area is very rare. Papillary thyroid carcinoma favors lymphatic spread [4]. Hematogenous spread rarely occurs to the lung, bones and brain [5]. We report a rare case where metastasis from papillary thyroid carcinoma presented as an oropharyngeal mass, partially extending over wall of hypopharynx.
Case Presentation
A 36 year old woman presented to her general medical practitioner with a five week long history of difficulty in solid food uptake and hoarseness of voice. She was referred to the Surgical Oncology department of King George’s Medical University. On initial examination a pharyngeal exophytic growth was identified on larygoscopy and a provisional diagnosis of a primary oropharyngeal epithelial malignancy was considered. A biopsy of the lesion was done and sent to our referral laboratory at Dr. Ram Manohar Lohia Institute of Medical Sciences, Lucknow for histopathological evaluation. Microscopic assessment of H&E stained sections showed a tumor predominantly arranged in a papillary architecture. Tumor cells showed high nucleo-cytoplasmic ratio, round to oval nuclei, vesicular chromatin, inconspicuous nucleoli and moderate of eosinophilic cytoplasm (Figure 1A). A differential diagnosis of a primary papillary adenocarcinoma or a metastatic lesion was considered. Initial immunohistochemistry (IHC) for the unknown primary was done for relatively commoner metastatic stites including lung, gastrointestinal tract, breast, female genital organs and kidney. A primary immunohistochemistry panel comprising of CK-7, CK-20, p40, p16, CDX-2, TTF-1 and WT-1 was applied. In view of a strong positive expression of TTF-1 (Figure 1B) and CK-7 (Figure 1C) with negative p40, p16, CK-20, CDX-2 and WT1 a possibility of a primary papillary adenocarcinoma of the lung and papillary thyroid carcinoma were considered. Thyroglobin showed cytoplasmic expression in all cells clinching the diagnosis of a papillary thyroid carcinoma (Figure 1D). On retrospect the patient gave a history of thyroid surgery 13 years back. No documented proof of type of surgery and histopathological diagnosis was available and the patient was not able to provide any details. An axial contrast enhanced CT scan revealed a mass lesion arising from posterior wall of oropharynx, partially extending over posterior wall of hypopharynx at the metastatic site (Figure 2a). CT slice at the level of thyroid cartilage showed involvement of left lateral and posterior aspect of larynx by thyroid mass (Figure 2b). A separate hypo-enhancing mass arising from the left lobe of thyroid was also identified. Final diagnosis of a metastatic papillary thyroid carcinoma was rendered. Patient was given palliative therapy addressing the issue of dysphagia and breathlessness and a tracheostomy was done.
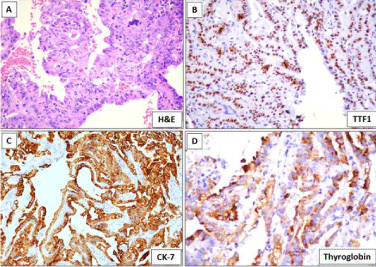
Figure 1
Figure 1
Histological and Immunohistochemical features of index case. A)
Tumor cells are arranged in a papillary architecture. B-D) Strong expression
of TTF-1, CK-7 and Thyroglobin.
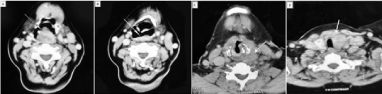
Figure 2
Figure 2
A) Axial contrast enhanced CT scan reveals a mass lesion (arrow) arising from posterior wall of oropharynx. B) Inferiorly, mass is partially extending
over posterior wall of hypopharynx. C) Section at the level of thyroid cartilage shows involvement of left lateral and posterior aspect of larynx by thyroid mass. D)
Hypo-enhancing mass arising from the left lobe of thyroid.
Discussion
The oral cavity is an uncommon site for metastatic disease.
Metastatic disease, when present, involves jaw bones primarily the
mandible followed by maxilla [6] Soft tissue and mucosal metastasis
is rare. Major primary sites in males are usually the lung, kidney, liver,
and prostate while in women oral metastases may come from the
breast, female genital organs, kidney, and colo-rectum [7]. A recent
study by Thiele et al. [8] have reported incidence of distant metastasis
at 2.39% of all malignancies in the oral and cranio-maxillofacial area,
which is twice as high as previous published data.
The tissue involved in the oral cavity varies with the primary site
and in men metastases from the lung go to the mandible and maxilla
followed by oral mucosa (22% and 31.3%, respectively) whereas
the prostate adenocarcinoma metastasizes to jawbones (11%) and
kidney to the oral soft tissues (14%). In women, breast primaries
affect jawbones and soft tissues (41% and 24.3%, respectively),
followed by adrenal and female genital organs in the jawbones (7.7%
and 14.8% respectively) [6]. The primary site considered initially in the current case was also lung in view of the papillary morphology
and immuoreactivity for TTF1. The classical nuclear morphology
of papillary thyroid carcinoma in terms of clear nucleoplasm,
intranuclear inclusions and grooves was not evident in our case at the
metastatic site. However positive thyroglobulin in the second line of
immunostaining confirmed the primary as a PTC.
PTC usually shows lymphatic invasion and frequently
metastasizes to regional lymph nodes, although distant metastases are
considerably less frequent [4]. Thyroid carcinoma metastasis to the
jaws is rare with only a limited number of cases previously reported
in the literature. Nikitakis in 2011 reported a case of mandibular
metastasis from PTC and summarized a review of 36 previously
reported cases of metastases from malignant thyroid neoplasms
including 33 to the jaw bones and three to the mucosa which included
one to the dorsal tongue and lower lip, right maxillary gingiva and
anterior mandibular gingival [9-10]. PTC accounted for 8 (22.2%)
cases. Single cases of metastasis from Hurthle cell, medullary, and
poorly differentiated carcinoma have been reported. In their review,
the vast majority of oral metastases from thyroid cancer were located
in the mandible (32/37; 86.5%). Further in a fair number of cases of
metastatic thyroid cancer to the oral cavity reviewed,there was also
involvement of adjacent structures such as the parotid, infratemporal
fossa, and masticator space and sinus. In our case also an extensive
spread of the primary thyroid mass to left lateral and posterior aspect
of larynx was evident in CT scan.
Recently Siddique et al. [11] reported a PTC with sarcomatoid
transformation metastasizing to the gingival mucosa. Nawale et al.
[12] reported 12 cases of metastatic neoplasms to the jaw bones and
observed 4/12 to be cases as PTC. However, none of their cases had
mucosal involvement. Summarizing, oral soft tissue metastasis from
PTC appear to have been reported in 6 cases only and these were
located mostly in the gingiva.
Parapharyngeal region metastasis from PTC thyroid is also rare.
Parapharyngeal lesions are often nonspecific or asymptomatic when
the tumor does not exceed 3.0 cm in size. Cases with larger lesions
frequently complain of a mass in the neck or oropharynx that causes
dysphagia [13], as was present in our case. Most parapharyngeal
metastases are unilateral; whereas some rare cases are bilateral.
Integrated 131I-SPECT/CT is a useful tool for the screening patients
with differentiated thyroid carcinoma, especially early lesions [14].
Parapharyngeal metastasis usually present as cystic lesions in the
parapharyngel region and retropharyngeal space, sometimes cystic
metastasis in lymphnodes or masquerading as a deep lobe parotid
mass. A transoral approach has been used to approach these lesions
both for FNAC and surgical ressection but they may rarely involve
the as oro-pharyngeal mucosa. Our case presented with an exophytic
mass in the oropharynx which was visualized on laryngoscopy.
Subsequent CT evaluation showed the lesion involving the posterior
wall of oropharynx, partially extending over posterior wall of
hypopharynx. Calcification has also been reported at metastatic sites.
Other proximal sites of metastasis include the larynx and pharynx
[15].
Differentiated Thyroid Cancer (DTC) is usually indolent with
good prognosis and long-term survival. However, DTC distant
metastasis is often a grave event and accounts for most of its diseasespecific
mortality. Metastasis in DTC occur in only 2.2% cases and
independent factors associated with distant metastases include male
gender, older age, single status, black and other non white races,
follicular and Hurthle cell histology, large tumor size, and positive
regional lymph nodes [16]. The major sites of distant metastases
are the lung and bone. Metastases to the brain, breast, liver, kidney,
muscle, parapharyngeal, parotid, adrenal, ovaries and skin are rare.
Recognizing rare metastases from DTC has a significant impact on the
clinical decision making and prognosis of patients. 131I single photon
emission computed tomography/computed tomography (131I-SPECT/
CT) can provide both metabolic and anatomic information about
metastatic lesions. Care should be taken to determine whether 131I
uptake found at an unexpected site is DTC metastasis or false-positive
uptake [17]. Prognostic factors in DTC include tumor size, multifocal
or bilateral occurrence, angioinvasion, and extra capsular growth,
presence of cervical lymph node metastases, distant metastases and
early local relapse.
Primary thyroid malignancies may also arise in the oropharynx
from thyroglossal duct remnants and in thyroglossal cyst. Occurrence
of primary carcinoma is reported to be present in 1% cases in
thyroglossal cyst of which 94% are histologically papillary thyroid
carcinoma [18]. Hoffman et al. [19] observed PTC in a thyroglossal
cyst along with a small thyroid carcinoma and three positive lymph
nodes. These authors argue the case of whether the cystic carcinoma is
primary or a metastasis from thyroid carcinoma in their case report.
It is interesting to note that the location of oral foramen caecum of
the thyroglossal duct is anatomically in a proximal relation to the
vallecula. A possiblity of a primary from thyroglossal duct remants
in the oral cavity was considered in our case initially, however the
presence of a large mass in the left lobe of the thyroid along with
extensive involvement of adjacent tissues and lymphnodes in CT
scan supported a primary in thyroid with metastatic lesion in the
oropharynx. In rarer instances primary thyroid malignancy may arise
in an ectopic lingual thyroid.
Clinical suspicion of a second primary tumour possibly Oral
Squamous Cell Carcinoma (OSCC) with a past history of a thyroid
carcinoma was considered in our case and the biopsy was sent as
an oropharyngeal carcinoma. Multiple synchronous head and neck
cancers are known to occur [20]. Collision metastases have also
been reported in the cervical lymphnodes from PTC and OSCC
simultaneously [21]. Collision tumors pose a diagnostic as well as
therapeutic challenge Squamous elements may occur in the process
of a dedifferentiation of papillary thyroid carcinoma and may appear
at metastatic site rather than the primary site and the diagnosis of a
collision metastasis should be given with caution [21]. In the current
case a well differentiated papillary lesion lined by a single layer of
neoplastic columar epithelium with focal clustering and solid areas
was evident at the metastatic site.
Papillary pattern in metastatic lesions is encountered frequently
in primaries from lung, renal papillary carcinoma, papillary thyroid carcinoma, papillary GI lesions, ovaries, urothelial neoplasms.
Differential diagnosis can be resolved using a panel of IHC including
CK 7, 20, TTF1, Napsin, CDX2, Thyroglobulin, WT1, ER, uroplakin.
Well differentiated morphology, a strong cytoplasmic thyroglobin and
nuclear TTF-1expression confirmed metastatic PTC in our case. The
modality of spread of tumor to the posterior wall of the oropharynx
in the current case could have been through lymphatic route or
through hematogenous spread. Minute dissection of 22 neck-halves
(11 adult cadavers) was undertaken by Saito et al. [22] to determine
the location and topographical relationships of the lymphatics of
the pharynx. Saito et al. [22] reported that Lymphatic drainage from
the hypopharynx was multidirectional with the pathways being
classified as follows: ascending pathway to the lateral pharyngeal and
lateral retropharyngeal nodes, lateral pathway to the internal jugular
chain, and descending pathway connecting to the uppermost vessels
ascending from the recurrent laryngeal nerve chain. The treatment
of oral metastases of thyroid carcinoma has varied extensively from
palliative to various combinations of surgical resection, radioactive
iodine treatment, radiotherapy, and/or chemotherapy. It has been
recommended that surgical resection of the metastatic tumor in
conjunction with total thyroidectomy, followed by radioactive iodine
treatment and/or external-beam radiation may afford better survival.
Nonetheless, the treatment decision depends on various factors,
including the operability of the metastatic lesions and the presence of
a solitary metastatic focus versus multiple metastasis. In widespread
metastatic disease, treatment is usually palliative. In our case,
patient had partial thyroidectomy 13 years back and now palliative
tracheostomy has been done. In conclusion, metastatic deposit of
PTC presenting as oropharyngeal mass has rarely been described.
Such a presentation can pose a diagnostic challenge to pathologists in
identifying the lesion as metastatic and locating the primary cancer.
IHC expression of TTF1 in tumor cell nuclei and thyroglobulin in the
cytoplasm confirms origin of tumor.
References
- Piattelli A, Fioroni M, Rubini C. Gingival metastasis from a medullary thyroid carcinoma: case report. J Periodontol. 2000; 71: 112-116.
- Shaha AR, Ferlito A, Rinaldo A. Distant metastases from thyroid and parathyroid cancer. ORL J Otorhinolaryngol Relat Spec. 2001; 63: 243-249.
- Nixon IJ, Whitcher MM, Palmer FL, Tuttle RM, Shaha AR, Shah JP, et al. The impact of distant metastases at presentation on prognosis in patients with differentiated carcinoma of the thyroid gland. Thyroid. 2012; 22: 884- 889.
- Larsen PR, Davies TF, Hay DI. The thyroid gland. In: Wilson JD, Foster DW, Kronenberg HM, Larsen PR, William’s textbook of endocrinology. 9th ed. W.B. Saunders Company. Philadelphia. 1998; 487.
- McCaffrey TV, Bergstralh EJ, Hay ID. Locally invasive papillary thyroid carcinoma: 1940-1990. Head Neck. 1994; 16: 165-172.
- Hirshberg A, Shnaiderman-Shapiro A, Kaplan I, Berger R. Metastatic tumours to the oral cavity - pathogenesis and analysis of 673 cases. Oral Oncol. 2008; 44: 743-752.
- Hirshberg A, Leibovich P, Buchner A. Metastatic tumors to the jawbones: analysis of 390 cases. J Oral Pathol Med. 1994; 23: 337-341.
- Thiele OC, Freier K, Bacon C, Flechtenmacher C, Scherfler S, Seeberger R. Craniofacial metastases: A 20-year survey. J Craniomaxillofac Surg. 2011; 39: 135-137.
- Nikitakis N, Polmeris A, Polymeri A, Sklavounou A. Metastatic papillary thyroid carcinoma to maxilla: Case report and literature review. Head Neck Pathol. 2012; 6: 216–223.
- Whitaker B, Robinson K, Hewan-Lowe K, Budnick S. Thyroid metastasis to the oral soft tissues: case report of a diagnostic dilemma. J Oral Max Surg. 1993; 51: 588–593.
- Siddique I, Chengot P, Frewer J, Walker D. A rare case of gingival metastases from papillary thyroid carcinoma. Int J Surg Case Rep. 2015; 7: 82–84.
- Nawale Kundan Kisanrao, Monika Vyas, Shubhada Kane, Asawari Patil. Metastatic tumors in the jaw bones: A retrospective clinicopathological study of 12 cases at Tertiary Cancer Center. J Oral Maxillofac Pathol. 2016; 20: 252–255.
- Tomoda C, Matsuzuka F, Miyauchi A. Parapharyngeal metastasis from papillary thyroid carcinoma: a case diagnosed by thyroglobulin measurement in peroral fine-needle aspiration of a cystic metastatic lymph node. J Laryngol Otol. 2005; 119: 155-157.
- Xue YL, Qiu ZL, Song HJ, Luo QY. Value of ¹³¹I SPECT/CT for the evaluation of differentiated thyroid cancer: a systematic review of the literature. Eur J Nucl Med Mol Imaging. 2013; 40: 768-778.
- Hakeem AH, Pradhan SA, Bhele S, Tubachi J. Metastasis of papillary thyroid cancer to the larynx and pharynx: unusual case report. Eur Arch Otorhinolaryngol. 2012; 269: 2585-2587.
- Goffredo P, Sosa JA, Roman SA. Differentiated thyroid cancer presenting with distant metastases: a population analysis over two decades. World J Surg. 2013; 37: 1599-1605.
- Hong-Jun Song, Yan-Li Xue, Yan-Hong Xu, Zhong-Ling Qiu, Quan-Yong Luo. Rare metastases of differentiated thyroid carcinoma: pictorial review Endocrine-Related Cancer. 2011; 18: 165-174.
- Hofmann V, Kösling S, Thanh PN, Holzhausen HJ, Bloching M. [Papillary thyroid carcinoma in a thyroglossal duct cyst: primary tumor or metastasis?]. HNO. 2009; 57: 719-724.
- Kennedy TL, Riefkohl WL. Lingual thyroid carcinoma with nodal metastasis. Laryngoscope. 2007; 117: 1969-1973.
- Khari Lewis, A Gulati. Multiple Synchronous Primary SCC of the Oral Cavity with Undiagnosed Papillary Thyroid Carcinoma. 2016; Washington State Convention Center, Seattle, WA.
- Alhanafy AM, Al-Sharaky D, Abdou AG, Abdallah RA. Metastatic Collision Tumour (Papillary Thyroid Carcinoma and Squamous Cell Carcinoma) in Cervical Lymph Nodes: An Immunohistochemical Analysis. J Clin Diagn Res. 2016; 10: 11-13.
- Saito H, Sato T, Yamashita Y, Amagasa T. Topographical analysis of lymphatic pathways from the meso- and hypopharynx based on minute cadaveric dissections: possible application to neck dissection in pharyngeal cancer surgery. Surg Radiol Anat. 2002; 24: 38-49.