Case Report
Does Weighted Kypho-Orthosis (wko) Reduce Risk of Fall in Women With Osteoporosis?: A Preliminary Study
Leyla Sedighipour*, Seyed Ahmad Raeissadat, Seyed Mansoor Rayegani , Mahsdis Hashemi, Safura Pournajaf and Mohammad Hasan Bahrami
Department of Physical Medicine & Rehabilitation, Shahid Beheshti University of Medical Sciences, Iran
*Corresponding author: Leyla Sedighipour, Physical Medicine and Rehabilitation, Physical medicine and Rehabilitation Research Center, Shahid Beheshti University of Medical Medical sciences, Tehran
Published: 02 Dec, 2016
Cite this article as: Sedighipour L, Raeissadat SA,
Rayegani SM, Hashemi M, Pournajaf
S, Bahrami MH. Does Weighted
Kypho-Orthosis (wko) Reduce Risk of
Fall in Women With Osteoporosis?: A
Preliminary Study. Ann Clin Case Rep.
2016; 1: 1198.
Abstract
Background: The aim of the present study was to determine the effects of weighted kyphorthosis on improving dynamic balance tests in women with osteoporosis.
Methods: In this randomized controlled clinical trial, twenty three patients with osteoporosis were
included. The patients were assigned into two groups: 1) control group who received 4-week homebased
daily exercise program and 2) intervention group (weighted kyphorthosis) who performed
exercises and wore weighted kyphorthosis for one hour twice a day. Patients were assessed using
computerized balance tests by Balance Master (NeuroCom) (Limits of Stability, Step Quick Turn,
Sit to Stand and Walk across tests) before and 4 weeks after start of treatment.
Results: Speed in walk across test was improved significantly in both groups compared to baseline
from (77.6±25 cm/s to 91.57±30 cm/s and from 72.60±20cm/s to 88.73±18 cm/s) in intervention
and control groups respectively. Improvement in right turn time in step quick turn, end point
excursion and mean of excursion parameters of Limits of Stability was more significant in orthosis
group in comparison with control group (P <0.05).
Conclusion: Applying WKO together with exercise program improved some computerized
balance tests in women with osteoporosis.WKO can be suggested as an effective intervention in
postmenopausal women in order to reduce the risk of falling.
Keywords: Osteoporosis; Balance tests; Weighted KyphOrthoris; Posture training support
Introduction
Osteoporosis is a common disorder characterized by reduced bone mass and by deterioration
of the micro architecture of the bone tissues, thereby leading to increased bone fragility. It affects
around 55% of the population over the age of 50 years in the United States [1-3]. Among common
clinical consequences are back pain [4], hyperkyphosis, limitations of physical functioning and impaired health-related quality of life in osteoporotic patients [4-6]. It is characterized by low bone
mass and micro-architectural changes of bone tissue, leading to increase in fracture risk [1,2,7].
Vertebral fractures can occur in spinal osteoporosis and constitute a major public health burden.
The incidence of spine fracture can be as high as 20% in postmenopausal women [4]. The weakness
of paraspinal extensor muscles in osteoporosis accompanied by repetitive vertebral micro fracture
results in hyperkyphosis, in osteoporotic patients [8-10]. Changes in spinal alignment would displace
the Center Of Pressure (COP) closer to the limit of stability, thereby making it easier to lose balance,
with consequent falls in elderly women with osteoporosis [6]. This postural changes and vertebral
fractures can impose physical stress on vertebral bodies leading to acute and chronic back pain
[5]. Furthermore, osteoporosis is associated with deficits of gait and balance, all together resulting
in an increased risk of falls [7]. Falls among the elderly, especially for those with osteoporosis, are
associated with high morbidity and mortality and are responsible for hip fracture and are the sixth
cause of death among elderly [11].
There are studies indicating that almost one third of falls followed by detrimental consequences
are preventable [12]. Apart from environmental modifications and pharmaceutical and physical
rehabilitative measures including muscle reeducation and resistance exercises leading to
improvements in static and dynamic posture and balance training are among most precious
preventive strategies for reducing the risk of falls and subsequent fractures [13-15].
Assessment of postural control and stability in osteoporotic patients through posturography is a promising and sensitive measurement approach for early detection or
pre clinical changes in the postural control system [16].
Previous studies have shown that wearing a spinal orthosis
such as osteomed, spinomed and weighted kyphorthosis result in
improvements of posture and back extensor strength. Weighted
kyphorthosis [WKO] is among the most known orthosis in
osteoporotic patients. In 2005, Sinaki indicated the positive effects
of WKO together with spinal proprioceptive extension exercise on
balance, gait, and risk of fall assessed by computerized dynamic
posturography [17].
In our previous work ,wearing WKO accompanied by back
extensor strengthening exercises lead to significant improvement in
functional balance tests including Functional Reach (FR) and Time
up and Go(TUG) tests in WKO group compared to exercise group
[18].
The purpose of the present study is to assess the effects of wearing
WKO together with spinal exercises on balance via performing
computerized dynamic balance tests including Sit to Stand, Walk
Across and LOS, by Neurocom tests in women with osteoporosis.
These tests, performed by Neurocom device, are dynamic and much
more functional and similar to daily activities compared to clinical
balance tests used in our previous work. Considering these facts, they
can better evaluate the risk of falling in the elderly.
Case Presentation
This study was conducted between during 2013 in Shahid
Modarres hospital, Tehran, Iran. The protocol of this clinical trial was
approved by Shahid Beheshti University of Medical Sciences, Human
Ethics Research Committee. This study was designed as randomized
clinical trial.
Patients voluntarily referred to physical medicine and
rehabilitation clinic were entered the study. Patients were screened
initially by an expert physiatrist to determine whether they met the
inclusion criteria.
Inclusion criteria were as follows: Women with osteoporosis
diagnosed based on low bone mineral densitometry at spine
(T-score of <-2.5), aged between 50-75 years old, thoracic kyphosis
angle between 35-55 degree (Cobb’s angle of thoracic kyphosis was
calculated from lateral radiograph of spine).
The patients with the following criteria were excluded from the
study:
The presence of secondary osteoporosis due to metabolic
diseases (such thyroid disease, etc) evaluated by clinical laboratory
tests, the presence of neuromuscular disorders, vertebral fracture in
last 6 months, history of spinal or lower limb surgical interventions
including arthroplasty, vertebroplasty or discectomy.
Serum level of Ca, P, alkaline phosphatase, 25 HO vitD3,
thyroid function tests, Renal function tests, parathyroid hormone
were evaluated in osteoporotic patients. The patients with low level
of vitamin D and secondary causes of osteoporosis were treated
appropriately but excluded from this study.
Patients who met the above mentioned criteria were assigned to
two groups (orthosis (intervention) and control groups). At the same
clinic, like intervention group, matched controls of comparable age
and weight and height were enrolled in the study as control group.
Randomization and Patients' Enrollment
Simple random sampling was used for this study. All patients
included in the study received a number then by using random
number table they were allocated to two groups (Control and
intervention groups).
Equal allocation between groups was performed. Hence, the
patients were classified randomly in control and intervention groups.
Random allocation sequence, who enrolled patients to interventions
were performed by one physician.
Blinding
The assessors supervised and performed NeuroCom balance
tests, as well as the statistician were blinded to the group assignment.
Patients in both groups received medications including 1000
mg calcium carbonate and 400 IU vitamin E daily and sodium
alendronate 70 mg weekly.
Patients in both groups were also instructed to have 30 minutes
of daily walking.
All Patients were followed via telephone calls to home to get sure
that they were sticking to the exercises correctly as prescribed for
them.
Control group: No orthosis was prescribed for this group; but
patients were taught to perform daily back extensor strengthening
exercises at home according to professor Sinaki program in Mayo
clinic [19] as follows:
1. In supine position, the patient flexes the knees and then abducts
and adducts the shoulders while the elbows are extended and upper
limbs are in contact with the floor.
2. In the supine position, the patient flexes the knees and put
hands over the head. By contracting abdominal muscles the patient
tries to draw the low back to the floor and keep this position for
10seconds.
3. In the prone position, the patient puts a pillow under the lower
abdomen and gently raises the head and shoulders from the floor as
much as possible and keeps this position for 10 seconds.
4. The patient sits on a chair and puts the hands behind the head.
Then he/she moves the elbows behind the head while inhaling. The
patient will do the opposite while exhaling.
5. Sitting on a chair, the patient flexes the elbows while keeping
the arms near to the trunk and then moves the arms back to reduce
thoracic kyphosis.
All of the exercise programs were taught by an experienced
physical therapist. Also, an illustrated pamphlet describing each
exercise was presented to each participant. A paper with a table was
given to each patient and she was asked to specify every day if she
would do the exercises and bring it on follow up visits. The patients
were called by a physical therapist every week to assess exercise
performance and associated problems. After 4 weeks, patients were
called to return to hospital for re-evaluations.
Intervention group (Orthosis group)
Patients in this group were taught to perform the same home
exercises as control group.
Weighted kyphorthosis was also administered for the patients in
this group.
Weighted kyphorthosis (WKO)
Weighted kypho-orthosis is an especially designed orthosis (made
by Cybernetics Company) with a harness and a 2-pound pouch,
which centers its weight on the posterior of the spine at T10 to L4.
The patients were guided to place the weighted kyphosis orthosis
over the thoracic spine and adjust the straps such that the bottom of
the pouch is located at the waistline.
Patients were instructed to wear the device when ambulating for
one hour a day (30 minutes at the morning and the evening) for 4
weeks. During this 4 week, patients were followed by telephone calls
to assure that they were using the orthosis correctly.
An experienced orthotist instructed the patient regarding the
proper usage of orthosis.
Measures
Dual X-ray absorptiometery (DXA) was used for measuring
bone mineral density of spine or hip. All patients were referred to
one imaging center for bone mineral densitometry. Then DXA scan
was carried out using the Hologic QDR-4500 machine (Hologic,
Waltham, MA) to determine BMD values of the femur and lumbar
vertebrae. The accuracy of a DXA, a monthly calibration measurement,
according to the manufacturer’s instructions, was performed.
Precision was defined as the reproducibility and the ability of
densitometric systems to detect changes in BMD over time. Precision
error of the machine and the technologist kept below 1 % in the center
we referred our patients for bone densitometry.
The cobb’s angle of kyphosis was calculated from perpendicular
lines drawn on a standard thoracic spine radiograph (lateral view):
a line extends through the superior endplate of the vertebral body,
marking the beginning of the thoracic curve and the inferior endplate
of the vertebral body, marking the end of the thoracic curve.
An experienced radiologist ruled out osteoporotic fractures via
assessing associated X- rays.
Dynamic balance tests: The NeuroCom Equitest Long Force Plate
(NeuroCom International, Clackamas, Oregon) was used to assess
the participants’ performance on functional tasks. The Long Force
Plate was used to objectively evaluate balance and postural stability
under dynamic tests [20]. The Sit to Stand, Walk Across, Step/
Quick Turn and Limits of stability were selected from the Functional
Limitation Assessment Battery due to their ability to target functional
characteristics pertaining to lower body strength, flexibility, and
balance. These areas of interest were chosen due to their impact on
independent Function. All participants performed each task three
times and the mean score was used in the analyses.
Subjects were allowed one practice trial for familiarization with
the procedure of the test.
Testing Protocols
Before starting protocol, each participant received a verbal
explanation of the protocols.
Sit to stand test (STS): During the measurements subjects were
positioned on the platform facing the monitor with barefoot. The
starting position before each trial was standardized by placing knees
at 90 degree flexion by adjusting foot placement.
Subjects were instructed to stand up as quickly as possible when start sign appeared on the monitor. They were not allowed to use arms or hands to push off their legs or the seated surface. Subjects
were asked to remain stationary until the test was completed (< 5 sec
after they rose).
The parameters of this test are as follows:
a. Weight transfer (in seconds): time elapsed until the
moment of rising,
b. Rising index (percentage of the body weight): is the
percentage of weight bearing (% body weight), which is the ratio of
the amount of weight borne on both legs to the patient’s total body
weight during the rising phase.( Amount of force exerted on the
platform during the rising phase),
c. Center of gravity (COG) sway velocity (in degrees per second):
postural sway velocity during upright posture,
d. Left/right weight symmetry (percentage of body weight):
symmetry of the body weight distribution on the lower extremities
during the rising phase.
Walk Across (WA): —Participants were positioned in front of a
force plate and were instructed to “Go,” via an audible prompt. Three
gait cycles were completed across the force plate, while outcome
measures included Step Width (lateral distance in centimeter),
Step Length (longitudinal distance in centimeters), and Step Speed
(velocity in centimeters/second)
Step/quick turn (SQT): The patient is instructed to take two
forward steps on command, and then quickly turn 180˚ to either the
left or right and return to the starting point.
Limits of stability (LOS): The NeuroCom LOS test required
participants to transfer their COG, while standing on stable force
plates, toward 8 targets in a sequential clockwise direction spaced at
45° intervals around the body’s COG, as represented on a computer
monitor. Before testing, subjects were informed that the on-screen
COG cursor (i.e., visual biofeedback) moved in response to the
movements of their body COG.
During the test, subjects were required to stand with their arms
by their sides and to maintain their feet in the standardized foot
position. A reference grid superimposed on the force plate allowed
for careful monitoring of the feet during the testing procedures. They
were instructed to keep their body in a straight line, using their ankle
joints at the primary axis of motion and to move toward each target
as directly and quickly as possible.
Outcomes include: reaction time, sway velocity, directional
control, endpoint excursion and maximum excursion. Endpoint
excursion and maximum excursion are calculated as percentages of
the subject’s theoretical 100% limit of stability that is a function of
their height.
The test was repeated three times and the average values of the
measurements were documented.
Data analysis: SPSS-18 was used for data analysis. Kolmogorovsmirnov
was used for testing normality of variable distribution.
Independent T-test and Man whitney tests were conducted to
determine if there was a statistically significant change in demographic
characteristics between the two groups and improvement in balance
tests after therapy. Wilcoxon-signed rank test was conducted to
determine the significant change in balance tests within each group
after therapy.
Ethics: The patients were enrolled after providing informed
consent as approved by the institutional review board of Shahid
Beheshti Medical University. The written consent form was signed or
fingerprinted by the patient.
Table 1
Table 1
Demographic characteristics including age, height, weight and body
mass indices compared between two groups.
Table 2
Table 2
The scores of Step quick turn parameters compared between two groups before and after study.
Table 3
Table 4
Table 4
The scores of Step quick turn parameters compared between two groups before and after study.
Table 5
Table 5
The scores of Limits of Stability (LOS) parameters compared between two groups before and after study.
Figure 1
Results
The patients’ characteristics at the start of study were depicted
in Table 1. There were no between-group differences at the baseline
in demographic characteristics and dynamic balance variables (Table 1-5).
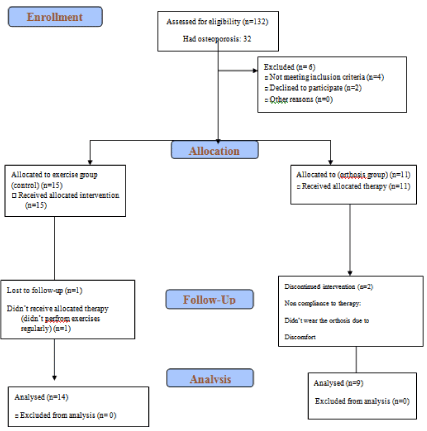
At the beginning of the study, 132osteoporotic patients (hip
and/or spine) were assessed for eligibility to enter the study. From
32 patients with osteoporosis at spine, 26 patients met the inclusion
criteria and accepted to participate in the study, and 23 people stayed
at the program during the follow up(two persons from orthosis and
one person from control group were dropped out of the study due to incomplete exercises and not wearing the orthosis completely). The results of 23 patients (14 patients in control and 9 patients in Orthosis
group) who remained in the study were analyzed. (CONSORT flow
chart, Figure 1).
Primary outcomes
Step Quick Turn: As it can be read from the Table 2, there was
no statistically significant difference in this test scores between the
two groups at the start of study. At the end of study, the parameters of
this test didn’t change significantly in control group. However, only
in intervention group, Rt turn time improved significantly compared
to baseline (P=0.02).
Sit to Stand: There was no statistically significant difference in
this test scores between the two groups at the start of study. At the
end of study, there was no statistically significant improvement in the
parameters of this test in both control and intervention group (Table 3).
Walk across: There was no statistically significant difference in
this test scores between the two groups at baseline.
In both control and intervention groups, significant improvement
in speed was noticed at the end of the study, there was no significant
difference between two groups regarding speed improvement
(P=0.85)(Table 4).
LOS: There was no statistically significant difference in this test
scores between the two groups at baseline.
In intervention group, significant improvement in mean of EPE
(P=0.01) and mean of MXE (P=0.00) were noticed after intervention.
No significant change was noticed in control group at the end of the
study (Table 5).
Secondary outcomes
Patient’s compliance: One patient stopped wearing orthosis in
the intervention group after one week due to discomfort. One patient
in each control and intervention group didn’t perform exercises
regularly. Their results excluded from final analysis.
Patient’s satisfaction: All patients completed the study were
satisfied with the treatment (both orthosis and exercises).
Adverse events: No adverse events were noticed during the study.
Secondary discussion
Based on the results of the present study, improvement in
balance was noticed in patients with osteoporosis after wearing
weighted kyphorthosis for 4 weeks. According to walk across test,
speed improvement was noticed in both groups with no significant
between group differences. Right turn time decreased significantly
only in WKO group. Two parameters of LOS including the mean of
End Point Excursion and Maximal Excursion increased significantly
in WKO but not in control group.
Improvement in the above mentioned parameters can be
translated as better postural stability in intervention group. Postural
stability has been defined as the ability to control the body’s COG
within a given base of support. The understanding of postural
stability control (i.e., balance) is essential for performing activities of
daily Living and decrease in fall rate [21].
In practice, the actual LOS of a person may be defined as the
distance the patient is willing and able to move without losing balance
and taking a step [22]. As with the Functional Reach (FR) test, the
LOS test has been shown to provide reliable scores that are predictive
of fall risk [22].In our previous work [18] WKO lead to improvement
in FR. In essence, LOS should measure similar components of
balance as FR. However, Wallmann reports that there is no significant relationship between FR measures and anterior displacement on the LOS test [23].
Decrements in dynamic postural control have been attributed
to both age and pathologic changes in parameters associated with
movements of the COG. Compared with healthy older adults,
osteoporotic patients exhibit smaller voluntary COG excursions,
reach maximal lean more slowly, and exhibit less postural control
once they have reached maximum lean [22].
The LOS test provides spatial and temporal measures (e.g.,
movement velocity, maximum excursion, directional control) of
COG movements as a person volitionally leans to various positions
in space [22]. LOS test measures one aspect of balance utilized in
daily life, and is a measure of improvement in balance resulting from
rehabilitation. Considering the high efficiency of LOS test in early
identification of falls in elderly, high reliability of its parameters, high
test-retest reliability while measured by NeuroCom and its ease of
execution, it is popular and confident in global measures of balance
[21,24].
Previous studies suggested that postural control among
individuals with osteoporosis is different from general elderly
population. Individuals with osteoporosis are more likely to present
higher sway velocities and greater maximum shift of the COG [25].
Azadinia [26] evaluated the effects of two spinal orthoses
on balance in the elderly with thoracic Kyphosis. Patients were
allocated to two groups (Spinomed orthosis and the posture-training
support groups). In both groups, significant changes were observed
in the studied balance parameters. Authors concluded that both
interventions may improve balance in the elderly in a similar manner.
The ability to transfer from sit to stand (STS) is another most
commonly performed tasks of daily living. Accurate control of COG position is critical in controlling the rise movement, as well as to maintain postural stability. Ideally, COG sway velocity during the
rise should be minimal. Increased sway velocity can be caused by
weak trunk extension or inability to keep the COG movement to a
minimum in the elderly. However in our study, no significant change
was noticed in this balance parameter.
In normal aging, step length and speed decreased, turn time
increased substantially with aging.
Slow gait speed is associated with falls in aged people. Therapeutic
exercises to improve gait speed and step length in osteoporotic elderly
can reduce the risk of fall [27,28]. In our study, step speed improved
in both control and intervention group which can be contributed to
extension exercises administered for patients in both groups.
In the present study, another balance parameter changed in
intervention group was right turn time. The ability to make a rapid
turn in walking is very crucial and sensitive to dynamic balance
problems [29].
There are few studies evaluating the beneficial impacts of spinal
orthosis on gait balance [9,29,32].
In 2005, Sinaki [32] conducted a study to determine the outcome
of intervention with a spinal weighted kypho-orthosis (WKO) and a
spinal proprioceptive extension exercise dynamic (SPEED) program
on the risk of fall in osteoporotic patients. After 4 week of intervention,
balance, gait, and risk of falls assessed by computerized dynamic posturography improved significantly with SPEED program.
The role of exercise in the treatment of osteoporosis is to improve
axial stability through improvement of muscle strength and axial
posture [33].
In our study, wearing WKO lead to improvement in turn quick
test, mean of excursion and end point excursion. WKO promotes
improvement in posture and increased back extensor strength by
two mechanisms: first, the device produces a posterior force below
the inferior angle of scapula and reduces anterior compressive
forces exerted on the kyphotic spine [10]. Second, application of the
WKO increases a patient’s perception of spinal joint position, which
plays an important role in static and dynamic posture. It creates a
preprioceptive input and enhances the patient's ability to sense the
position of the spine [32]. WKO also promotes muscle re-education
and decreases painful contractions of the erector spine muscles in
kyphosis [33].
Besides WKO, there are some studies investigating other types
of spinal orthoses in osteoporosis. A trial was conducted in 2012
evaluating the influence of ThämertOsteo-med spinal orthosis on
gait and physical functioning in osteoporotic women. At a 6-month
follow up, the study demonstrated that wearing a spinal orthosis
reduced double support time associated with improvement on gait
stability [33]. Pfeifer et al. [31] evaluated the efficacy of two spinal orthoses in patients with osteoporotic vertebral fractures. Wearing
the orthosis Spinomed in that study was associated with increase in back extensor and abdominal flexor strength, decrease in the angle of kyphosis and body sway, also decrease in average pain [31].
In all above mentioned studies, spinal orthosis had positive effects
on postural balance which is in agreement with the results of our
studies indicating improvement in LOS, step quick turn and speed
in WKO group.
In conclusion, applying WKO together with back extensor
strengthening exercises in women with osteoporosis leads to
improvement in dynamic balance tests evaluated by NeuroCom
which can be translated to decreased risk of fall in real life in this
population.
The limitations of our study were the relatively small number of
cases included and short term follow ups evaluations. Absence of a
control group receiving no intervention was another limitation of this
study; however, due to ethical considerations we had to consider the
least routine interventions including exercise and medications for all
patients.
We encourage more randomized controlled clinical trials with
larger sample size evaluating the effect of WKO on risk of fall in
long term via applying clinical functional and para clinical tests in
the elderly with osteoporosis. Future studies can also consider power
calculation to determine adequate sample size that yielded improved
power and effect size which was lacking in the present study.
References
- Lin JT, Lane JM. Rehabilitation of the older adult with an osteoporosisrelated fracture. Clin Geriatr Med. 2006; 22: 435-447.
- Renno AG, RN Driusso P. Effects of an exercise program or respiratory function, posture and on quality of life in osteoporotic women: a pilot study. Physiotherapy. 2005; 91: 113-118.
- Nordstrom A, Tervo T, Hogstrom M. The effect of physical activity on bone accural, osteoporosis and fracture prevention. The open bone journal. 2011; 3: 11-21.
- Fechtenbaum J, Cropet C, Kolta S, Horlait S, Orcel P, Roux C. The severity of vertebral fractures and health-related quality of life in osteoporotic postmenopausal women. Osteoporos Int. 2005; 16: 2175-2179.
- Miyakoshi N, Itoi E, Kobayashi M, Kodama H. Impact of postural deformities and spinal mobility on quality of life in postmenopausal osteoporosis. Osteoporos Int. 2003; 14: 1007-1012.
- Martin AR, Sornay-Rendu E, Chandler JM, Duboeuf F, Girman CJ, Delmas PD. The impact of osteoporosis on quality-of-life: the OFELY cohort. Bone. 2002; 31: 32-36.
- Kanis JA, McCloskey EV, Johansson H, Cooper C, Rizzoli R, Reginster JY. European guidance for the diagnosis and management of osteoporosis in postmenopausal women. Osteoporosis international: a journal established as result of cooperation between the European Foundation for Osteoporosis and the National Osteoporosis Foundation of the USA. 2013; 24:23-57.
- Sinaki M. Prevention treatment of osteoporosis. In: Braddom R, editor. Physical medicine and rehabilitation. 3 ed: Saunders Elsevier. 939-50.
- Kaplan RS, Sinaki M, Hameister MD. Effect of back supports on back strength in patients with osteoporosis: a pilot study. Mayo Clin Proc. 1996; 71: 235-241.
- Sinaki M. Correction of Back Extensor strength With Thoracic Kyphosis and Lumbar Lordosis Deficient Women. American Journal Of Physical medicine and Rehabilitation. 1996; 75: 370-374.
- Madureira MM, Takayama L, Gallinaro AL, Caparbo VF, Costa RA, Pereira RM. Balance training program is highly effective in improving functional status and reducing the risk of falls in elderly women with osteoporosis: a randomized controlled trial. Osteoporos Int. 2007; 18: 419-425.
- Vaapio SS, Salminen MJ, Ojanlatva A, Kivela SL. Quality of life as an outcome of fall prevention interventions among the aged: a systematic review. Eur J Public Health. 2009; 19: 7-15.
- Gunendi Z, Ozyemisci-Taskiran O, Demirsoy N. The effect of 4-week aerobic exercise program on postural balance in postmenopausal women with osteoporosis. Rheumatol Int. 2008; 28: 1217-1222.
- Hongo M, Itoi E, Sinaki M, Miyakoshi N, Shimada Y, Maekawa S, et al. Effect of low-intensity back exercise on quality of life and back extensor strength in patients with osteoporosis: a randomized controlled trial. Osteoporos Int. 2007; 18: 1389-1395.
- Raeissadat S, Mojgani P, Pournajaf S. Short-term Effect of Back Extensor Strengthening exercises on the Quality of Life of patients with Primary Osteoporosis. Life Sci J. 2013; 10: 1060-1065.
- Jbabdi M, Boissy P, Hamel M. Assessing control of postural stability in community-living older adults using performance-based limits of stability. BMC Geriatr. 2008; 8: 8.
- Sinaki M, Brey RH, Hughes CA, Larson DR, Kaufman KR. Significant reduction in risk of falls and back pain in osteoporotic-kyphotic women through a Spinal Proprioceptive Extension Exercise Dynamic (SPEED) program. Mayo Clin Proc. 2005; 80: 849-855.
- Raeissadat SA, Sedighipour L, Pournajaf S, Vahab Kashani R, Sadeghi S. Effect of Posture Training with Weighted Kypho-Orthosis (WKO) on Improving Balance in Women with Osteoporosis. J Aging Res 2014; 2014: 427903.
- Sinaki M. Prevention treatment of osteoporosis. In: R B, editor. Physical medicine and rehabilitation: Saunders Elsevier. 2007; 939-50.
- www.neuro.com
- Pickerill ML, Harter RA. Validity and reliability of limits-of-stability testing: a comparison of 2 postural stability evaluation devices. J Athl Train. 2011; 46: 600-606.
- Clark S, Iltis PW, Anthony CJ, Toews A. Comparison of older adult performance during the functional-reach and limits-of-stability tests. J Aging Phys Act. 2005; 13: 266-275.
- Wallmann HW. Comparison of elderly nonfallers and fallers on performance measures of functional reach, sensory organization, and limits of stability. J Gerontol A Biol Sci Med Sci. 2001; 56: M580-583.
- Juras G, Stomka K, Fredyk A, sabota G, Bacik B. Evaluation of the limits of stability(los) balancr test. Journal human kinetics. 2008; 19: 39-52.
- Burke TN, Franca FJ, Menes SR, Cardoso VI, Pereira RM, Danilevicius CF, et al. Postural control among elderly women with and without osteoporosis: is there a difference? Sao Paulo Med J. 2010; 128: 219-224.
- Azadinia F, Kamyab M, Behtash H, Maroufi N, Larijani B. The effects of two spinal orthoses on balance in elderly people with thoracic kyphosis. Prosthet Orthot Int. 2013; 37: 404-410.
- Lopopolo RB, Greco M, Sullivan D, Craik RL, Mangione KK. Effect of therapeutic exercise on gait speed in community-dwelling elderly people: a meta-analysis. Phys Ther. 2006; 86: 520-540.
- Hausdorff JM, Rios DA, Edelberg HK. Gait variability and fall risk in community-living older adults: a 1-year prospective study. Arch Phys Med Rehabil. 2001; 82: 1050-1056.
- Vogt L, Hubscher M, Brettmann K, Banzer W, Fink M. Postural correction by osteoporosis orthosis (Osteo-med): a randomized, placebo-controlled trial. Prosthetics and orthotics international. 2008; 32: 103-110.
- Schmidt K, Hubscher M, Vogt L, Klinkmuller U, Hildebrandt HD, Fink M, et al. [Influence of spinal orthosis on gait and physical functioning in women with postmenopausal osteoporosis]. Der Orthopade. 2012; 41: 200-205.
- Pfeifer M, Kohlwey L, Begerow B, Minne HW. Effects of two newly developed spinal orthoses on trunk muscle strength, posture, and qualityof- life in women with postmenopausal osteoporosis: a randomized trial. American journal of physical medicine & rehabilitation / Association of Academic Physiatrists. 2011; 90: 805-815.
- Sinaki M, Brey RH, Hughes CA, Larson DR, Kaufman KR. Balance disorder and increased risk of falls in osteoporosis and kyphosis. Osteoporos Int. 2005; 16: 1004-1010.
- Sinaki M. Musculoskeletal Rehabilitation in Patients with Osteoporosis- Rehabilitation of Osteoporosis Program-Exercise (ROPE). Mineralstoffwechse. 2010; 17: 60-65.