Case Report
Secondary Angle Closure Glaucoma and Malignant Hypertension: A Rare Association
Rengaraj Venkatesh* and Srinivasan Kavitha
Aravind Eye Hospital, India
*Corresponding author: Rengaraj Venkatesh, Aravind Eye Hospital, Pondicherry, 605007, India
Published: 02 Dec, 2016
Cite this article as: Venkatesh R, Kavitha S. Secondary
Angle Closure Glaucoma and Malignant
Hypertension: A Rare Association. Ann
Clin Case Rep. 2016; 1: 1194.
Abstract
Malignant hypertension often presents with end organ damage. Eyes are usually involved in the form of papilledema and retinopathy. We report a case of secondary angle closure glaucoma associated with malignant hypertension. A previously healthy 30 year old man presented with painful loss of vision in his right eye associated with headache.He had raised intra ocular pressure and shallow anterior chamber in his right eye, and grade four hypertensive retinopathy in both eyes. His blood pressure was 260/180 mm of Hg. There was complete visual recovery with reversal of angle closure once the blood pressure was brought under control.
Introduction
Malignant hypertension is a sudden and rapid development of extremely high blood pressure. It is often associated with end organ damage including central nervous system, cardiovascular system and renal system [1]. Prompt diagnosis and management of this condition, is essential to prevent ocular and systemic morbidities. Involvement of the eye in the form of papilledema and retinopathy, is quite often associated with malignant hypertension [2]. We report a case of acute angle closure glaucoma due to malignant hypertension, which recovered completely once the blood pressure was brought under control.
Case Presentation
A previously healthy, 30 years old, man presented to us, with painful loss of vision, associated
with redness in his right eye, of 3 days duration. He also gave history of headache. He had no relevant
medical history in the past, apart from intermittent headaches.
On examination his visual acuity was counting fingers at 3 feet in his right eye and 20/20 in his
left eye. Anterior segment examination of the right eye (Figure 1) revealed, marked circum corneal
congestion, sub conjunctival haemorrhage, corneal epithelial edema, shallow anterior chamber, 4
mm pupil with sluggish pupillary reaction, and clear lens. Left eye (Figure 1) was quiet and anterior
chamber was of normal depth. Intraocular pressure (IOP), measured with applanation tonometry
was 68 mm of Hg in the right eye and 20 mm of Hg in the left eye. Gonioscopy showed closed
angles in the right eye (Figure 2) and wide open angles in the left eye. Fundus examination through
undilated pupil, in the left eye revealed disc edema, splinter haemorrhages, and hard exudates in the
macula. Undilated fundus evaluation of the right eye, through a hazy media, showed disc edema and
splinter haemorrhages in the right eye. Ultra-sonogram, B scan of the right eye revealed choroidal
effusion. His blood pressure reading was 260/180 mm of Hg.
With this picture, a diagnosis malignant hypertension with grade four hypertensive retinopathy
in both eyes and secondary angle closure glaucoma in the right eye, due to posterior push mechanism
was made. We started him on topical antiglaucoma medication, a fixed combination of beta blocker
and alpha agonist. Since the renal status of the patient was not known, oral acetazolamide and
intravenous mannitol were avoided. He was immediately shifted to emergency department, of local
government hospital. He was admitted in the intensive care unit and was started on medications to
lower his blood pressure. Complete systemic evaluation was done by the internist.
He reviewed with us 4 weeks from the initial visit. He was on beta blocker, calcium channel
blocker and angiotensin II-receptor blocker. His renal parameters were found to be normal. He
was diagnosed to have malignant hypertension, resulting from primary/essential hypertension, by
the internist. His blood pressure reading was 130/80. His best corrected visual acuity was 20/30 in
his right eye and 20/20 in his left eye. Anterior segment evaluation was found to be normal in both
eyes. Anterior chamber was of normal depth in the right eye with wide open angles on gonioscopy (Figure 3). His IOP was 14 and 18 mm of Hg, in his right and left eye
respectively. Dilated fundus evaluation showed completely resolved
disc edema in both eyes (Figure 4). The cup to disc ratio was 0.3 in
the right eye and 0.2 in the left eye. Right eye showed nerve fibre
layer defects in the superotemporal quadrant, few hard exudates,
elschnig spots. Left eye showed haemorrhages, cotton wool spots,
hard exudates. He was advised to stop the topical antiglaucoma
medication, and his IOP was found to be normal, on follow up visit, 4
weeks after stopping the medication.
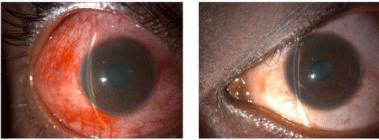
Figure 1
Figure 1
Right eye showing ciliary congestion, sub conjunctival
haemorrhage, corneal edema, shallow anterior chamber, and left eye
showing normal anterior chamber depth.
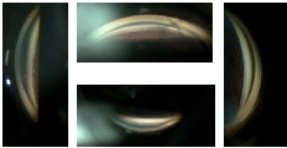
Figure 2
Figure 2
Gonioscopy of the right eye showing closed angles. The view was
hazy because of corneal edema.
Figure 3
Figure 4
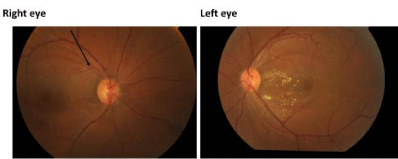
Figure 4
Fundus photo taken at 4 weeks review visit showing resolution of
disc edema. Right eye showing nerve fibre layer defects in the superotemporal
quadrant (black arrow), few hard exudates and retinal pigment epithelial
changes macula. Left eye showing hard exudates and cotton wool spots.
Discussion
Malignant hypertension is a life threatening condition.
Diagnosing this condition, in a previously normal patient, based
on the fundus picture is not a rare phenomenon [3]. However acute
angle closure glaucoma associated with malignant hypertension has
not been reported so far. Our patient showed a complete recovery
with reversal of angle closure once the blood pressure was normalised.
The probable cause of acute angle closure in this patient is a
posterior push mechanism, as revealed by choroidal effusion in the
B scan. Interference with the venous drainage, leading to choroidal
effusion, swelling and anterior rotation of the ciliary body might have
caused acute angle closure. Differential diagnosis considered were
posterior scleritis, angle closure associated with central retinal vein
occlusion (CRVO) and acute primary angle closure (APAC). Ultrasonogram,
B scan was not consistent with posterior scleritis. Once the
corneal edema cleared, fundus picture was very well co-related with
the features of malignant hypertension, ruling out CRVO. The visual
recovery was good, consistent with previous case report on malignant
hypertension [4]. Examination of the fellow eye helped us to rule out
APAC.
This case report highlights the importance of examination of the
fellow eye, which helped us not only to rule out APAC, but also made
us to think of malignant hypertension. Baseline systemic evaluation
is a must, in all the patients presenting with such high intraocular
pressure. Often we tend to bring down the IOP, with all the available
antiglaucoma medications including intravenous mannitol and
oral acetazolamide. Administering intravenous mannitol and
acetazolamide might be fatal in such patients, since they can have
impaired renal function [5]. Malignant hypertension has very poor
prognosis in the absence of treatment. It needs to be managed by
concerned specialist to limit the consequences.
Conclusion
To conclude, malignant hypertension should be considered as one of the differential diagnosis in patients presenting with acute secondary angle closure.Conservative management and control of hypertension will be sufficient to reverse the angle closure.
References
- Cremer A, Amraoui F, Lip GY, Morales E, Rubin S, Segura J, et al. From malignant hypertension to hypertension MOD: a modern definition for an old but still dangerous emergency. J Hum Hypertens. 2016; 30: 463-466.
- Rodiguez MA, Kumar SK, De Caro M. Hypertensive crisis. Cardiol Rev. 2010; 18:102-107.
- Iqbal Tajunisah, Dinesh Kumar Patel. Malignant hypertension with papilledema. The J Emergency medicine 2013; 44: 164-165.
- D Shukla, Asif Y Virani. Reversible loss of vision in malignant hypertension. N Engl J Med. 2016; 374; 1368.
- Priya V, Edward K Massin, Thomas D. Dubose JR. Mannitol induced acute renal failure. J Am Soc Nephrol. 1997; 8: 1028-1033.