Case Report
Cerebral Epithelioid Haemangioendothelioma
Helen Kavnoudias1*, Philip Chan1, Mark Schoenwaelder1, Sarah Saxon2, Catriona Mc Lean2 and Jeffrey Rosenfeld3
1Department of Radiology, The Alfred Hospital, Australia
2Department of Pathology, The Alfred Hospital, Australia
3Department of Neurosurgery, The Alfred Hospital, Australia
*Corresponding author: Helen Kavnoudias, Philip Chan, Department of Radiology, 1/F Philip Block, The Alfred hospital, 55 Commercial Road, Melbourne, Vic 3004, Australia
Published: 03 Oct, 2016
Cite this article as: Kavnoudias H, Chan P, Schoenwaelder
M, Saxon S, Mc Lean C,
Rosenfeld J. Cerebral Epithelioid
Haemangioendothelioma. Ann Clin
Case Rep. 2016; 1: 1154.
Abstract
Epithelioid haemangioendothelioma (EHE) is a rare tumour of endothelial cell origin that arises
from soft tissue, liver, lungs and rarely, the brain.
We present a case of cerebral EHE in a 43 year old previously well female, who suffered two
generalised tonic-clonic seizures. Contrast enhanced CT and MRI brain showed a left frontal
lobe vividly enhancing intra-axial lesion at the grey-white junction. Pathological examination
revealed a circumscribed lesion with spindled to epithelioid cells, some exhibiting cytoplasmic
vacuoles, within a myxoid stroma. Tumour cells demonstrated immunoreactivity with CD31
and patchily with epithelial membrane antigen. These findings were consistent with epithelioid
haemangioendothelioma. Follow up MRIs showed no recurrence at 28 months post surgery.
Cerebral EHEs frequently display imaging features that correlate with the underlying pathology and
cystic degeneration. Tumours are hypervascular, with a variable pattern of enhancement, but the
degree of enhancement is usually vivid, best shown on angiography. Large intralesional large flow
voids and rCBV elevation are common.
EHE exhibits malignant potential intermediate between benign haemangiomas and conventional
angiosarcoma, and is differentiated histologically. “Malignant EHE” describes tumours exhibiting
greater nuclear atypia, tumour cell spindling, necrosis and excessive mitotic activity. These atypical
features, present in approximately 33%, correlate with propensity for metastasis.
Current standard of treatment is total surgical excision. Adjuvant and neoadjuvant therapy remain
controversial.
Cerebral EHE should be considered a differential if imaging features demonstrate a hypervascular
lesion.
Introduction
Epithelioid haemangioendothelioma (EHE) is a rare tumour of endothelial cell origin that arise from soft tissue, liver and lungs [1,2]. Intracranial EHE’s are extremely rare, accounting for <0.02% of all brain tumours. The clinical presentation is often non specific and imaging features may mimic other more common entities. The definitive diagnosis is made by pathological examination. It is important to recognise this entity as some may be described as “malignant epithelioid haemangioendothelioma”, which correlate with propensity for metastasis. We present a case of cerebral EHE in a 43 year old previously well female.
Case Presentation
A 43 year old previously well female presented to emergency with two episodes of generalised
tonic-clonic seizure with no post ictal neurological deficit.
CT brain (Figure 1) demonstrated a solitary 18 mm intra-axial left frontal lobe lesion located at the grey-white junction, hypoattenuating pre-contrast and vividly and homogenously enhancing.
There was associated perilesional vasogenic oedema with moderate mass effect.
Contrast enhanced MR brain (Figure 2) showed the lesion to be T2 hyperintense, T1 hypointense
with vivid enhancement and associated vasogenic oedema. Flow voids were not identified within the
lesion.
At surgery, a pink gelatinous lobulated tissue was found 2 mm beneath the cortex. Post operative course was unremarkable.
Microscopic examination (Figure 3a) showed a well circumscribed
lesion comprised of spindled to epithelioid cells, some exhibiting
cytoplasmic vacuoles, arranged within a myxoid stroma. There was
no significant nuclear atypia. Mitotic figures were not identified. The
cells were arranged about a prominent fine calibre vasculature lined
by plump endothelial cells. Necrosis was not a feature.
Tumour cells showed immunoreactivity with antibodies against
the vascular endothelial marker CD31 (Figure 3b) and patchy
immunoreactivity of weak to moderate intensity with antibodies
against epithelial membrane antigen (EMA). Immunohistochemistry
with antibodies against glial fibrillary acidic protein (GFAP),
neurofilament, S100 and Melan-A was negative.
Tumour morphology and immunoprofile were in keeping with a
diagnosis of epithelioid haemangioendothelioma.
The patient was recurrence free on MRI brain 28 months post
discharge.
Figure 1
Figure 2
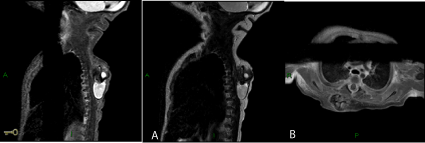
Figure 2
Magnetic resonance imaging of the thorax.
(a) Sagittal T1 WI F. (b) T2 WI of the back showing a complex mass with cystic component and a solid component with fat and calcifications and heterogeneous
enhancement following Gadolinium injection.
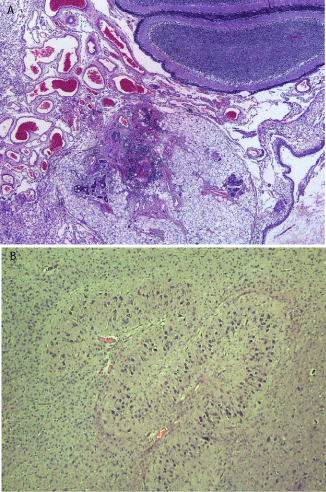
Figure 3
Figure 3
(a) Histology of back mass: the figure shows cerebellar tissue
and skin appendages with mature eccrine glands. (b) Glial tissue with basal
nucleus-like structure.
Discussion
EHE, first described by Enzinger and Weiss et al. [1] in 1982, is a rare tumour of endothelial cell origin, most often arising in
the superficial or deep soft tissue of the extremities, but also well
documented in bone, liver and lungs [1,2] Cerebral examples are
extremely rare, accounting for <0.02% of all brain tumours [3-5].
Intracranial EHE may affect individuals of any age, although case
reports have demonstrated a bimodal distribution, with a peak in
younger children < 1 year of age and another in adults. There is a
slight male predilection 1.6:1 in all age populations, although a higher
male predominance of 9:2 is observed in the paediatric cohort.
Intra-cranial EHE’s display non specific imaging features that
correlate with the underlying pathology [6]. On non contrast CT,
the lesion is isodense or hyperdense with variable homogeneity. On
MRI, it may be hypointense or isointense on T1 and hyperintense
on T2. Cystic components are frequently present due to cystic
degeneration. These tumours demonstrate hypervascularity on
imaging, with variable pattern of enhancement – homogenous or
heterogenous, tumoural or nodular – and the degree of enhancement
is usually vivid. Large intralesional large flow voids [7-9] and rCBV
elevations are common findings, although the latter was not present
in our case. Haemorrhage may occur, with subsequent hemosiderin
deposits [6]. Radiological differential diagnoses of intra-axial EHE
include primary neoplasm such as glioma or lymphoma, metastases,
infection or haemorrhage. Extra-axial EHE are often misdiagnosed
as meningioma.
Angiography often demonstrates a highly vascular tumour with
variable single or multiple arterial supply [3,4,8,10-13].
EHEs exhibit a malignant potential intermediate between that
of benign haemangiomas and conventional angiosarcoma [1,2]. The
tumour is characterised by a recurrent t(1;3) translocation resulting in
a WWTR1-CAMTA1 fusion gene [14-16]. More recently, an alternate
YAP1-TFE3 fusion gene has been described in a small subset of EHE,
occurring in young adults and showing some distinct morphological
features [17]. Approximately 50% of tumours demonstrate origin
within or adjacent to a vessel, usually a small vein [2,18]. The
primitive vascular differentiation demonstrated in EHE distinguishes
it from benign haemangiomas and the conventional angiosarcomas
[19]. “Malignant epithelioid haemangioendothelioma” has been used
to describe those tumours that exhibit greater nuclear atypia, tumour
cell spindling, necrosis and mitotic activity exceeding 1 per 10 high
power fields. These atypical features, seen in approximately one third
of tumours, correlate with propensity for metastasis [2].
Current standard of treatment is total surgical excision.
Recommendation for adjuvant and neoadjuvant chemoradiotherapy
remains controversial.
Conclusion
Epithelioid haemangioendothelioma is an extremely rare brain tumour of intermediate grade that can exhibit certain imaging characteristics, particularly large flow voids and vivid enhancement. These features should raise the possibility of the diagnosis.
References
- Weiss SW, Enzinger FM. Epithelioid Hemangioendothelioma: A Vascular Tumor Often Mistaken for a Carcinoma. Cancer. 1982; 50: 970- 981.
- Tancredi A, Puca A, Carbone A. Multifocal Cerebral Hemangio- Endothelioma. Case Report and Review of the Literature. Acta Neurochir. 2000; 142: 1157-1161.
- Kubota T, Sato K, Takeuchi H, Handa Y. Successful removal after radiotherapy and vascular embolization in a huge tentorial epithelioid hemangioendothelioma: a case report. J Neurooncol. 2004; 68: 177-183.
- Taratuto AL, Zurbriggen G, Sevlever G. Epithelioid hemangioendothelioma of the Central Nervous System. Immunohistochemical and Ultrastructural Observations of a Pediatric Case. Pediatr Neurosci. 1988; 14: 11-14.
- Zheng J, Liu L, Wang J, Wang S, Cao Y, Zhao J. Primary intracranial epithelioid hemangioendothelioma: a low-proliferation tumor exhibiting clinically malignant behavior. J Neurooncol. 2012; 110: 119-127.
- Chan YL, Ng HK, Poon WS, Cheung HS. Epithelioid haemangioendothelioma of the brain: a case report. Neuroradiology. 2001; 43: 848-850.
- Zheng J, Li P, Ma S, Geng M. Epithelioid hemangioendothelioma of the meninges mimicking metastatic carcinoma: a case report. Clin Neuropathol. 2013; 32: 324-327.
- Golash A, Strang FA, Reid H. Intracranial haemangioendothelioma mimicking a meningioma. Br J Neurosurg. 1999; 13: 594-597.
- Joo M, Lee GJ, Koh YC, Park YK. Hemangioendothelioma of the Sphenoid Bone: A Case Report. J Korean Med Sci. 2001; 16: 241-244.
- Zhang J, Wang Y, Geng D. Intracranial epithelioid hemangioendothelioma: an unusual CTA finding in one case. Br J Neurosurg. 2010; 24: 294-295.
- Salinas-Lara A, Rembao-Bojorquez D, Tena-Suck ML, Malagon D. Sellarparasellar epithelioid hemangioendothelioma. J Neurol Sci Turk. 2006; 23: 231.
- Pearl GS, Takei Y, Tindall GT, O’Brien MS, Payne NS, Hoffman JC. Benign Hemangioendothelioma Involving the Central Nervous system: “Strawberry nevus” of the Neuraxis. Neurosurgery. 1980; 7: 249-256.
- Puca A, Meglio M, Rollo M, Zannoni GF. Intracranial Epithelioid Hemangioendothelioma: Case Report. Neurosurgery. 1996; 38: 399-401.
- Fletcher CDM, Unni KK, Mertens F. Pathology and Genetics of Tumours of Soft Tissue and Bone. IARC Press, Lyon. 2002.
- Mendlick MR, Nelson M, Pickering D, Johansson SL, Seemayer TA, Neff JR, et al. Translocation t(1;3)(p36.3;q25) Is a Nonrandom Aberration in Epithelioid Hemangioendothelioma. Am J Surg Path. 2001; 25: 684-687.
- Tanas MR, Sboner A, Oliveira AM, Erickson-Johnson MR, Hespelt J, Hanwright PJ, et al. Identification of a disease-defining gene fusion in epithelioid hemangioendothelioma. Sci Transl Med. 2011; 3: 98ra82.
- Errani C, Zhang L, Sung YS, Hajdu M, Singer S, Maki RG, et al. A novel WWTR1-CAMTA1 gene fusion is a consistent abnormality in epithelioid hemangioendothelioma of different anatomic sites. Genes Chromosomes Cancer. 2011; 50: 644-653.
- Antonescu CR, Le Loarer F, Mosquera JM, Sboner A, Zhang L, Chen CL, et al. Novel YAP1-TFE3 fusion defines a distinct subset of epithelioid hemangioendothelioma. Genes Chromosomes Cancer. 2013; 52: 775-784.
- Mentzel T, Beham A, Calonje E, Katenkamp D, Fletcher CD. Epithelioid hemangioendothelioma of skin and soft tissues: clinicopathologic and immunohistochemical Study of 30 Cases. Am J Surg Path. 1997; 21:363- 374.