Case Report
Heterotopic Pregnancy: A Case Report
Martin William* and Roumpf Steven
Department of Emergency Medicine, Indiana University Health, USA
*Corresponding author: Martin William, Department of Emergency Medicine, Indiana University Health, USA
Published: 01 Nov, 2016
Cite this article as: William M, Steven R. Heterotopic
Pregnancy: A Case Report. Ann Clin
Case Rep. 2016; 1: 1139.
Abstract
Objective: We report an extremely rare case of a heterotopic pregnancy in a 24 year old female that had a spontaneous conception and no use of assisted reproductive technologies (ART).
Methodology: Case Report and review of related literature.
Results: The patient was worked up for her abdominal pain. An intrauterine pregnancy (IUP) was
confirmed at bedside by ultrasound and a formal ultrasound demonstrated an ovarian mass, thought
initially to be a hemorrhagic cyst. The patient was taken urgently to the OR where the diagnosis of
a heterotopic pregnancy was made and confirmed by surgical pathology. The patient recovered well
and continues to have a healthy IUP.
Conclusions: Heterotopic pregnancy is a very rare diagnosis, even more so in the absence of ART.
However, the diagnosis should not be ignored as it is a surgical emergency and requires surgical
resection.
Introduction
Heterotopic pregnancy is rare. In today’s world with assisted reproduction techniques the incidence is approximately 1 in 3900. In patients without ART, the incidence is thought to be much lower, approximately 1 in 30,000 pregnancies. Factors that increase a patients risk include tubal disease, high levels of estradiol/progesterone and high numbers of transferred embryos as can be seen in IVF. Over 90% of heterotopic pregnancies are found in the fallopian tube [1-3]. If ruptured, the treatment is surgical, often a laparoscopic salpingectomy and the condition itself carries a significant rate of spontaneous abortion of the viable IUP.
Case Presentation
In June 2016, a 24 year old, 11 week pregnant, otherwise healthy African American female
presented to our emergency department with right-sided abdominal pain that radiated from the
lower to upper quadrant. The pain was described as sharp and the patient had associated nausea
and vomiting. She had a similar pain (less intense) about a month ago and was treated for cystitis.
The patient denied any vaginal bleeding and had no history of reproductive medications and/or
procedures. She was G3P1 (spontaneous vaginal delivery x1 and spontaneous, abortion x1).
Her exam was significant for diffuse abdominal tenderness, especially in the RUQ, with no
rebound tenderness and a blood pressure of 98/58 and heart rate of 98. Initial work up included
a cmp, cbc w/diff, lipase, EKG, urinalysis and UPT followed by a bedside ultrasound. Labs were
significant for a hgb of 10 (only previous was 11.4 from five days prior) and sodium of 133. Otherwise
all labs were within normal limits. Bedside ultrasound demonstrated an IUP with HR of 180 (Figure
1). Initial management included intravenous normal saline (to which the patient responded well), as
well as pain and nausea medicine. After all initial labs were back, formal ultrasounds of the kidneys,
uterus and appendix were ordered due to concern for other causes of right sided abdominal pain
such as appendicitis, cholecystitis, ovarian torsion, and nephrolithiasis. They were significant for
free fluid and an ill-defined 4 cm right adnexal vascular structure (Figure 2).
Obstetrics was consulted and the decision was made to admit the patient for serial exams for
the initial concern of a ruptured ovarian cyst and to obtain an abdominal MRI. While still in the ED
fluid resuscitation and pain management was continued and the patient remained hemodynamically
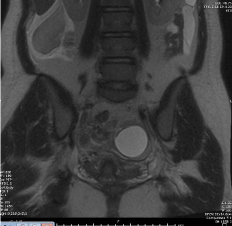
stable. The abdominal MRI (Figure 3) was significant for 2 cysts of the left ovary, likely right
hemorrhagic cyst and lobular mass on the right side of the abdomen within the peritoneal fluid. The
patient experienced worsening pain and a drop in hgb to 7.3. Obstetrics then decided to perform a
diagnostic laparoscopy in the OR.
During the diagnostic laparoscopy, obstetrics found approximately
500 ml of blood and clot in the abdomen with bright red blood filling
in evacuated spaces concerning for active hemorrhage. The right
fallopian tube was visualized and an ectopic pregnancy was visualized
and found to be actively hemorrhaging. The ectopic pregnancy
was removed via a right laparoscopic salpingectomy. The tissue
was sent to pathology, which confirmed the diagnosis of an ectopic
tubal pregnancy, which in this patients setting made the diagnosis
a heterotopic pregnancy. The patient was stabilized and discharged
later that evening and continues to have a healthy IUP in her second
trimester at the time of this submission.
Figure 1
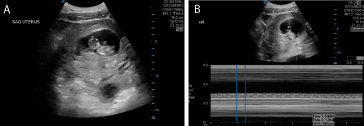
Figure 1
(a) Bedside ultrasound demonstrating an healthy IUP. (b) Bedside ultrasound demonstrating an intrauterine fetus heart rate of approx 180.
Figure 2
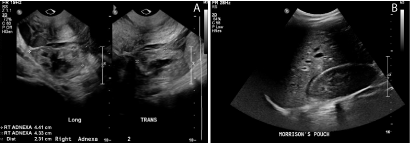
Figure 2
(a) Right adenxal mass seen on formal transvaginal ultrasound in longitudinal and transverse views. (b) Free fluid seen in Morrison’s pouch on formal renal ultrasound.
Figure 3
Discussion
Heterotopic pregnancy refers to an intrauterine and extrauterine
pregnancy. Most commonly these locations are the uterus and
fallopian tube, but this is not always the case, with some cases reporting
the ectopic pregnancy in other areas such as the abdomen. Before
the age of assisted reproductive technology (ART), the incidence of
heterotopic pregnancy was approximately 1 in 30,000. Since ART
however, that incidence has become much less, around 1 in 3900. If
the patient is undergoing ART the incidence is approximately 1.5 in
1000 pregnancies [1-3].
The patient’s symptoms are often very similar to an ectopic
pregnancy and they typically present with abdominal pain that may
be localized or diffuse. On pelvic exam the physician may feel an
adnexal mass or an enlarged uterus. Vaginal bleeding can also be
present. Depending on the stage of illness the patient may also be
peritoneal and hypotensive. There are no physical exam/lab findings
that are specific for heterotopic pregnancy but this diagnosis should
be considered in any hypotensive pregnant patient with abdominal
pain and an IUP identified on bedside ultrasound, especially in the
setting of free fluid on ultrasound and/or history of ART [4].
The differential of abdominal pain in pregnancy is wide. Once
an IUP has been confirmed, diagnoses of appendicitis, kidney stone (especially if infected), pyelonephritis, gallbladder disease,
ovarian torsion, endometritis, and heterotopic pregnancy should
be considered as these could all have high morbidity/mortality for
patients if not diagnosed. The diagnosis of heterotopic pregnancy is
especially difficult, as it cannot be easily determined by serial β-HCG.
Some literature has suggested ultrasound for the diagnosis, but
various case reports, including this one, continue to demonstrate its
low overall sensitivity. This may be partially due to the confirmation
of an IUP often giving a sense of false security, which can lead to the
misdiagnosis of the patient’s abdominal pain. Because of this, late
diagnosis and rupture is common in the diagnosis of heterotopic
pregnancy [5-6]. Nearly half of the cases present with rupture,
hemorrhage, and emergency intervention. Despite this, patients
presenting with a viable IUP have a 70% chance of producing a living
child if the diagnosis is made and treated appropriately [7].
Treatment for heterotopic pregnancy typically involves
laparoscopy and, most often a salpingectomy or salpingostomy.
However, if the patient demonstrates hemodynamic instability, a
laparotomy would then be indicated. Due to the inherent IUP that
is viable, systemic methotrexate plays no role in the treatment of a
heterotopic pregnancy. There have been some case reports of use of
local injection of potassium chloride and methotrexate as well as case
reports of expectant management but there seems to be a high rate
of failure and there is little evidence to suggest these interventions
currently [8-12].
Conclusion
Heterotopic pregnancy is a rare diagnosis, especially in a patient without any ARF history. The diagnosis can also be difficult and has a high risk of misdiagnosis given the presence of an IUP. Correct diagnosis and immediate intervention, often with laparoscopic surgery can be life saving for both the mother and the intrauterine pregnancy.
References
- Chadee A, Rezai S, Kirby C, Ekaterina Chadwick, Sri Gottimukkala, Abraham Hamaoui, et al. Spontaneous Heterotopic Pregnancy: Dual Case Report and Review of Literature. Case Rep Obstet Gynecol. 2016; 2016: 214593.
- Reece EA, Petrie RH, Sirmans MF, Finster M, Todd WD. Combined intrauterine and extrauterine gestations: a review. Am J Obstet Gynecol. 1983; 146: 323-330.
- Pisarska MD, Casson PR, Moise KJ Jr, DiMaio DJ, Buster JE, Carson SA. Heterotopic abdominal pregnancy treated at laparoscopy. Fertil Steril. 1998; 70: 159-160.
- Damario, Ectopic Pregnancy. In: Rock Jr, Jones III. Te Linde’s Operative Gynecology. 10th ed. Philadelphia, PA: Lippincott Williams and Wilkins; 2011. 794-795.
- Jeon H S, Shin H J, Kim I H, Chung DY. A case of spontaneous heterotopic pregnancy presenting with heart activity of both embryos. Korean J of Obstet Gynecol. 2012; 55: 339–342.
- Li XH, Ouyang Y, Lu GX. Value of transvaginal sonography in diagnosing heterotopic pregnancy after in-vitro fertilization with embryo transfer. Ultrasound in Obstetrics & Gynecology. 2013; 41: 563-569.
- Rojansky N, Schenker JG. Heterotopic pregnancy and assisted reproduction--an update. J Assist Reprod Genet. 1996; 13: 594-601.
- Bedaiwy MA, Volsky J, Lazebnik N, Liu J. Laparoscopic single-site linear salpingostomy for the management of heterotopic pregnancy: a case report. J Reprod Med. 2014; 59: 522–524.
- Li JB, Kong LZ, Yang JB, Niu G, Fan L, Huang JZ, et al. Management of heterotopic pregnancy: experience from 1 tertiary medical center. Medicine. 2016; 95: e2570.
- Deka D, Bahadur A, Singh A, Neena Malhotra. Successful management of heterotopic pregnancy after fetal reduction using potassium chloride and methotrexate. J Hum Reprod Sci. 2012; 5: 57-60.
- Baxi A, Kaushal M, Karmalkar H, Sahu P, Kadhi P, Daval B. Successful expectant management of tubal heterotopic pregnancy. J Hum Reprod Sci. 2010; 3: 108-110.
- Goldstein JS, Ratts VS, Philpott T, Dahan MH. Risk of surgery after use of potassium chloride for treatment of tubal heterotopic pregnancy. Obstet Gynecol. 2006; 107: 506-508.