Case Report
Pancreatic IPMN Cancer: A Rare Case of Bone Metastases
Bouddabous S* and Farracho L
Department of Imaging and Medical Information Sciences, Geneva University Hospital, Switzerland
*Corresponding author: Sana Boudabbous, Department of Imaging and Medical Information Sciences, Division of Radiology, Geneva University Hospital, Genève, Rue Gabrielle-Perret-Gentil 4, 1211 Genève 4, Switzerland
Published: 13 Sep, 2016
Cite this article as: Bouddabous S, Farracho L. Pancreatic
IPMN Cancer: A Rare Case of Bone
Metastases. Ann Clin Case Rep. 2016;
1: 1131.
Abstract
We report a case of a 70-year-old male with1-month history of 9 kg weight loss and abdominal pain. Physical examination was normal and hepatic tests revealed a cholestasis. CT scan showed a pancreatic head mass associated with biliary ducts dilatation and an echo-endoscopic-guided fine needle aspiration of this lesion suggested an intraductal papillary mucinous neoplasm (IPMN) with mild dysplasia. A duodenopancreatectomy of the head of the pancreas was performed and histological images have shown a mixed adenocarcinoma with endocrine differentiation developed over an IPMN with one ganglion metastasis and negative resection margins. Subsequently, the patient received a treatment with 6 cycles of gemcitabine. A pulmonary metastasis appeared after one year of follow up and it was resected with success. Three years after the 4th lumbar vertebrae presented a lytic pattern and was treated with cementoplasty, but lumbar pain got worse. Lumbar vertebrae magnetic resonance imaging (MRI) showed a multi-lobulated lesion with peripheral enhancement in this vertebrae and a pseudocollection along the subcutaneous and bone path of the cementoplasty’s needle. A percutaneous biopsy was performed and revealed a metastatic disease. The patient presented later multiple bone cystic lesions in the pelvis and spine. This case illustrates a rare feature of IPMN bone metastases, rarely described on literature. This diagnosis should be considered when a history of cystic pancreatic tumour is known and an invasive procedure like biopsy is required to confirm the diagnosis.
Keywords: Pancreatic cancer-IPMN-cystic; Bone metastases
Introduction
IPMN of the pancreas are a pancreatic neoplasm originating from the mucinous epithelium
of the pancreatic duct. There are three classifications of IPMN disease among cystic pancreatic
tumours, according to their localization and extension within deduct system as main duct (MD),
branch duct (BD) or mixed.
IPMN are classified as benign or malignant (parenchymal invasive adenocarcinoma) according
to their degree of dysplasia. Some prognostic factors for malignancy include their localization, size,
histology subtype, positive margins, nodal metastases, vascular and perineural invasion [1,2]. Main
duct involvement as intestinal or biliopancreatic pathological phenotype means a higher risk of
malignancy [1].
The outcome of a cystic pancreatic carcinoma, as well as pancreatic adenocarcinoma, once
invasive is poor [3]. IPMN malignancy can occur in 30 to 88% of patients, as in situ or invasive
carcinomas. In situ carcinoma is considered when confined to the ductal structure, while invasive
carcinoma is suggested when it infiltrates the pancreatic parenchyma [1]. IMPN metastases are very rare and bone metastases have been rarely described.
The pattern of metastases may be unusual mimicking abscess, which makes the diagnosis
challenging in imaging methods.
Case Presentation
A 70-year-old male diagnosed with IPMN with mild dysplasia underwent a
duodenopancreatectomy of the pancreas’s head. Histological images showed a mixed adenocarcinoma
with endocrine differentiation developed over a mixed localisation, main (MD) and branch ducts
(BD). The margins were negative but there was one nodal metastasis. The pathological phenotype was intestinal and biliopancreatic. Subsequently, the patient received
a treatment with 6 cycles of gemcitabine.
During follow up, one year after the end of the chemotherapy,
a hypermetabolic pulmonary lesion was diagnosed and treated with
inferi or right lobe resection.
Two years after, the patient presented with backache in lumbar
region and a lumbar CT scan revealed one single lytic lesionin the
fourth lumbar vertebrae treated with cementoplasty, without release
of the pain. An MRI was performed and showed a multi-lobulated
lesion with peripheral enhancement in the vertebra and a pseudocollection
along the subcutaneous and bone path of the needle of
cementoplasty (Figure 1). There was no modification of the disc sign
or endplate of the adjacent vertebrae. A percutaneous biopsy was
performed and showed a metastatic spread of the disease with cystic
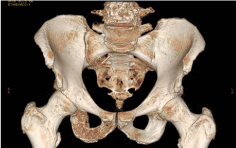
pattern, similar to the pancreatic tumour. The patient presented later
multiple bone cystic lesions in the pelvis and the spine (Figures 2 and
3).
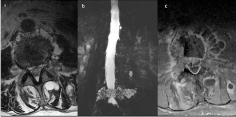
Figure 1
Figure 1
MRI examination, axial T2 (a) myelo-MR on coronal view (b) and
axial T1 fat saturation after contrast injection (c) cystic pattern of vertebral
metastases with paravertebral and posterior multiple cysts and peripheral
enhancement mimicking abscess after cimentoplasty.
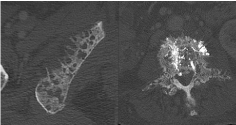
Figure 2
Figure 2
CT examination on bone kernel showing ischium and vertebral
involvement by metastases with multiple “holes”, a specific feature due to the
initial nature of pancreatic tumour.
Figure 3
Discussion
Cystic lesions of the pancreas are increasingly recognized. While
some lesions show benign behaviour (serous cystic neoplasm),
others have an unequivocal malignant potential as mucinous cystic
neoplasm, IPMN involving the pancreatic duct and solid pseudopapillary
neoplasm.
Partial resection with intra-operative frozen section examination
of the transaction margin is recommended for treatment [3]. Eight
per cent of the patients have recurrence even with negative margins
and a yearly follow-up with preferably non-radiating imaging (e.g. MRI or EUS) is suggested. The liver, the chest and the peritoneum are
the most frequent sites of metastases in the majority of patients who
recurred with invasive IPMN [1]. This case is unusual because the
bone metastases of IPMN are rarely described.
Concerning to the differential diagnosis of bone cystic lesions,
abscess and primitive lesions as unicameral bone cysts (UBC) and
aneurysmal bone cysts (ABC) may be considered in case of unique
localisation.
Unicameral bone cysts are common benign non-neoplastic bony
lesions, seen mainly in childhood, typically in the metaphysis of long
bones as humerus and femur. UBC's can be rarely seen in adults, and
when present is in unusual locations such as in the talus, calcaneus
or iliac wing. MR signal characteristics are T1 low signal and T2 high
signal, with no fluid-fluid levels unless there has been a complication
with haemorrhage.
ABC are also benign lesions and are mostly diagnosed in children
and adolescents, typically located in long bones of lower limb, spine
and sacrum. MRI demonstrates the characteristic fluid-fluid levels
with a solid component.
In conclusion, bone metastases in case of IPMN are really rare,
and in our knowledge this is the first case illustrating the multi-cystic
pattern of IPMN metastases. That entity should be considered when a
patient as a history of IPMN and a cystic pattern is seen in the bone.
References
- Vullierme MP, d'Assignies G, Ruszniewski P, Vilgrain V. Imaging IPMN: take home messages and news, Clin Res Hepatol Gastroenterol. 2011; 35: 426-429.
- Joanna Y, Martha B Pitman, Theodore S Hong. Intraductal Papillary Mucinous Neoplasm: Clinical Surveillance and Management Decisions. Semin Radiat Oncol. 2014; 24: 77-84.
- SG Pneumaticos, C Savidou, DS Korres, SN Chatziioannou. Pancreatic cancer's initial presentation: back pain due to osteoblastic bone metastasis. Eur J Cancer Care. 2010; 19: 137-140.
- Del Chiaro M, Verbeke C, Salvia R, Klöppel G, Werner J, McKay C, et al. European experts consensus statement on cystic tumours of the pancreas. Dig Liver Dis. 2013; 45: 703-711.
- Tanno S, Nakano Y, Nishikawa T, Nakamura K, Sasajima J, Minoguchi M, et al. Natural history of branch duct intraductal papillary – mucinous neoplasms of the pancreas without mural nodules: long-term follow-up results. Gut. 2008; 57: 339-343.