Case Report
Large Intracranial Hemorrhage after Dobutamine Stress Echocardiography
Adam Khan1, Sujit Bhimireddy2, Ahmad Issawi2, Michail Vasilakis2, Sarah Parker3 and Dzung Dinh2*
1Department of Medical School, University of Michigan, USA
2Department of Neurosurgery, University of Illinois-Peoria College of Medicine, USA
3Department of Neurology, University of Illinois-Peoria College of Medicine, USA
*Corresponding author: Khan A, Bhimireddy S, Issawi A, Vasilakis M, Parker S, Dinh D. Large Intracranial Hemorrhage after Dobutamine Stress Echocardiography. Ann Clin Case Rep. 2016; 1: 1127.
Published: 12 Sep, 2016
Cite this article as: Hornibrook J, Wells S, Finnis N, Gibbs
D. Late Metastatic Pontine Melanoma
Presenting as Ataxia. Ann Clin Case
Rep. 2016; 1: 1171.
Abstract
We report the case of a fatal intracranial hemorrhage after dobutamine stress echocardiography for chest pain in a 63-year-old female with no previous vascular risk factors. The patient experienced severe headache during stress testing and became clinically unresponsive 2-3 hours afterward. Imaging demonstrated a large 7.9 cm × 6.7 cm intracerebral hemorrhage (ICH) with subfalcine herniation. This is the first reported of a fatal ICH after dobutamine infusion. In large reviews of dobutamine use for cardiac stress testing, the agent has been proven to have a generally safe risk profile. However dobutamine may rarely produce life-threatening events in susceptible patients. Physicians should be aware of cerebrovascular complications, due to agent’s hypertensive effects, as another rare, but possible complication of dobutamine infusion.
Keywords: Dobutamine; Echocardiography; Intracerebral hemorrhage
Case Presentation
We report the case of a fatal intracranial hemorrhage after a dobutamine stress echocardiography.
The patient was a 63-year-old female who initially presented to our institution for acute-on-chronic
back pain unrelated to her eventual vascular pathology. She had a multi-year history of back pain
exacerbated by a recent episode where she fell on her back while walking. She was admitted for control
of her low back pain radiating to left lower extremity. Her low back pain and left S1 radiculopathy
remained refractory to high dose narcotic pain medication, epidural steroid injection, and physical
therapy. The patient, therefore, was scheduled for left L5-S1 hemilaminectomy and discectomy later
that week. However, on the morning of her scheduled surgery, the patient experienced substernal
chest pressure. The pressure was aggravated by anxiety and relieved spontaneously within minutes.
Although cardiac enzymes and the EKG were within normal limits the hospitalist service deemed her
to be at intermediate risk for the surgery due to the episode and her history of mitral regurgitation.
They requested the surgery to be postponed until a stress test could be performed and she was
started on aspirin and metoprolol.
The patient underwent pharmacologic dobutamine stress echocardiography the following
day. Before initiation of the test, the patient had no neurological symptoms, such as headache. The
test lasted for approximately 12 minutes and 7.1 mg of Dobutamine was administered. Patient’s
baseline heart rate and blood pressure were 78 bpm and 141/85 mmHg, respectively. The patient
reached a peak heart rate of 148 bpm, and a peak blood pressure during the exam of 190/32 mmHg.
During testing, the patient developed a severe headache upon initiation of infusion, which she
rated 10/10. On discontinuation of dobutamine, the headache mildly improved to an 8/10. The test
demonstrated no significant findings for cardiac disease or abnormal segmental wall motion. Upon
returning to her room, the patient continued to complain of headache and was given hydrocodone
and hydromorphone for pain relief. The pain was mildly alleviated by the pain medication. As the
patient was in general medicine floor as opposed to a general neurology unit, the neurosurgery team
was not informed of the headache and so a thorough evaluation was not performed.
Within three hours, the patient was found unresponsive, obtunded in her bed, and incontinent.
On exam, she was unable to open her eyes, was non-verbal, and produced no motor response,
thus, demonstrating a Glasgow Coma Scale (GCS) of 3. On exam, the patient had asymmetric
pupils with a dilated right pupil of 7 mm in size and the left pupil measuring 1mm. The patient also demonstrated upward bilateral Babinski responses. She was
emergently intubated and underwent computed tomography (CT)
scan which demonstrated an acute 7.9 cm x 6.7 cm hematoma
extending from the right frontal lobe with multiple foci of loculated
hemorrhage, and a significant right-to-left subfalcine herniation of
2.3 cm (Figure 1). An aneurysmal rupture was thought to be less likely
as there was no blood in the subarachnoid spaces and the basilar
cisterns (Figure 2). She was hypertensive with blood pressure of
220/110 mm Hg requiring multiple doses of labetalol and hydralazine
for management of her acute hypertensive crisis. She was immediately
taken to the operating room for an emergent right frontal craniotomy
and hematoma evacuation within 1 hour since the neurological
decline was noted. Post-operative CT of the head showed improved
mass-effect with decrease subfalcine herniation now measuring 0.7
cm (Figure 3).
The patient’s clinical condition did not improve after surgery
except for her pupils became equal 3mm and briskly reactive. Her
highest post-operative GSC score was 4; she remained non-verbal,
was unable to open her eyes, and her greatest level of motor activity
consisted of decerebrate posturing of her upper and lower extremities
to pain. Subsequent post-operative CT scans demonstrated reduction
of transfalcine herniation from 2.3 cm to 1.5 cm and changes
consistent with hematoma evacuation and resection cavity measuring
5 cm x 8 cm. Over the next five days, the patient’s post-operative CT
did not show any significant changes. Additionally, a craniectomy was
performed the fifth day after the initial craniotomy for progressively worsening edema and further subfalcine herniation. The patient
remained comatose without any clinical improvement. At the request
of the patient’s family, she was placed on comfort measures over the
subsequent days and transferred to hospice where she eventually
passed away on post-operative day 10.
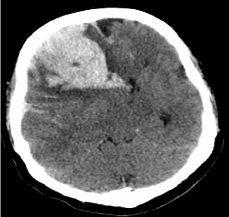
Figure 1
Figure 1
A non-contrast axial CT head showing a right frontal hematoma
measuring 7.9 cm in the AP dimension and 6.7 cm in the transverse
dimension with a 2 cm leftward transfalcine herniation.
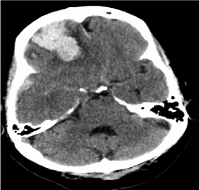
Figure 2
Figure 2
A non-contrast axial CT head at the level of the basilar cisterns
showing no subarachnoid hemorrhage to indicate the hemorrhage was
caused by a ruptured aneurysm.
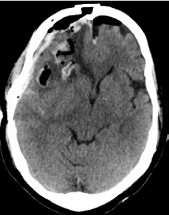
Figure 3
Figure 3
A non-contrast axial CT head on post-operative day 1 showing the evacuation of hematoma as well as improved transtentorial herniation now measuring 0.7 cm.
Discussion
Pharmacologic stress echocardiography is a commonly used
method of evaluation for coronary artery disease in patients who do
not tolerate or are unable to perform exercise stress echocardiography.
Dobutamine is a synthetic catecholamine that binds to β-1 and β-2
receptors, causing augmentation of both heart rate and contractility,
resulting in increased myocardial oxygen demand [1]. Multiple
studies have demonstrated a very low reported rate of life-threatening
complications. This case is the second reported instance of intracranial
hemorrhage as a complication of the dobutamine stress test, and is
the first reported case of dobutamine stress echocardiography leading
to intraparenchymal hemorrhage and eventual death.
Complications from dobutamine stress test are rare. An early study
from Indiana University reviewing the safety profile of dobutamine
stress echocardiography in 1118 patients, detailed noncardiac side
effects to include nausea in 8%, anxiety in 6%, headache in 4%, and
tremor in 4% of the study population [1]. Among methods commonly
used for stress echocardiography, dobutamine infusion causes the
highest rate of life-threatening events [2]. A multi-center registry of
35,103 studies of dobutamine stress echocardiography documented
fatal or near-fatal events in 63 patients, equaling an event rate of 1 in
557 [2]. These events included ventricular tachycardia or fibrillation,
myocardial infarction, severe hypotension, asystole, cardiac rupture,
stroke, and death [2]. No previous reports in the literature have listed
intraparenchymal hemorrhage as a life-threatening complication
from dobutamine infusion.
In a small proportion of patients, dobutamine has been noted
to induce a marked hypertensive response [3]. The risk of severe
hypertension, defined as systolic blood pressure >200 mm Hg and/
or diastolic blood pressure >110 mm Hg, has ranged from 0.8% - 2%
in multiple studies [4,5]. Although, our patient did not meet this
definition of severe hypertensive response, her blood pressure was markedly elevated during testing, coinciding with the development of
severe headache. Furthermore, dobutamine has been demonstrated to
augment arterial pressure and middle cerebral artery flow velocity in a
small study among septic patients [6]. When comparing patients with
hypertensive response from dobutamine stress echocardiography to
those without a hypertensive response, the former were more likely
to have a history of systemic hypertension and to be on β blocker
medication at the time of the test [3]. Our patient had neither of these
risk factors.
To our knowledge, there has been only one case report in the
literature of intracranial hemorrhage subsequent to dobutamine
stress test. In that report, the patient did not have any predisposing
risk factors for hemorrhage, but did have a supratherapeutic INR
at the time of hemorrhage. Additionally, the patient in that report
demonstrated three small foci of intraparenchymal hemorrhage and
was eventually discharged from the hospital with no neurologic deficit
at 1 month follow-up. This is in stark contrast to our healthy patient
who presented with a large hemorrhage requiring decompression via
craniotomy and eventually expired due to her illness.
According the International Classification of Headache Disorders
(ICHD) 3rd edition guidelines, identification of the etiology of
headache and associated neurologic symptoms requires only clinical
signs. As per the ICHD guidelines, when attributing a headache to
an underlying vascular condition, assessing the temporal relationship
between events is crucial [7]. The absence of other possible sources
of headache and the timing of the patient’s symptoms support
dobutamine infusion to be the immediate cause of our patient’s
acute neurologic change. The patient was without any neurological
symptoms before the initiation of dobutamine administration,
and the headache initiated with dobutamine infusion and slightly
dissipated only after discontinuation. Generally, in cases of nontraumatic
intracerebral hemorrhage, headaches present usually in
acute onset accompanied by focal neurological signs. In this patient,
the headache was the only initial symptom. No focal neurological
defecits were noted by the bedside nurse untill the patient was found
unresponsive.
In summary, dobutamine is a commonly used pharmacologic
agent used to perform stress echocardiography with a low documented risk profile. Large studies of dobutamine stress echocardiography have
documented rare life-threatening events to occur in patients. This
paper introduces the possibility of intracranial hemorrhage as a very
rare complication of dobutamine stress echocardiography mediated
through a hypertensive response. We would also like to emphasize
the importance of close neurological monitoring in patients who
complain of severe headache after undergoing dobutamine stress
echocardiography.
Acknowledgment
We sincerely thank Dr. Stanca Iacob and Mrs. Joanna Fleckenstein for their help in preparing this manuscript.
References
- Mertes H, Sawada SG, Ryan T, Segar DS, Kovacs R, Foltz J, et al. Symptoms, adverse effects, and complications associated with dobutamine stress echocardiography. Experience in 1118 patients. Circulation. 1993; 88: 15-19.
- Varga A, Garcia MA, Picano E, International Stress Echo Complication Registry. Safety of stress echocardiography (from the International Stress Echo Complication Registry). Am J Cardiol. 2006; 98: 541-543.
- Lee CY, Pellikka PA, Shub C, Sinak LJ, Seward JB. Hypertensive response during dobutamine stress echocardiography. Am J Cardiol. 1997; 80: 970- 971.
- Secknus MA, Marwick TH. Evolution of dobutamine echocardiography protocols and indications: safety and side effects in 3,011 studies over 5 years. J Am Coll Cardiol. 1997; 29: 1234-1240.
- Shah SP, Muqtada Chaudhry G. Intracranial Hemorrhage as a Complication of Dobutamine Stress Echocardiography: Case Report and Review of the Literature. Echocardiography. 2012; 29: E119-E121.
- Berré J, De Backer D, Moraine JJ, Vincent JL, Kahn RJ. Effects of dobutamine and prostacyclin on cerebral blood flow velocity in septic patients. J Crit Care. 1994; 9: 1-6.
- Headache Classification Committee of the International Headache Society (IHS): The International Classification of Headache Disorders, 3rd edition (beta version). Cephalalgia Int J Headache. 2013; 33: 629-808.