Case Report
Metastasis of Follicular Thyroid Carcinoma to the Vertebra: A Case Report
Kuşaslan R1, Vartanoğlu T1, Hepgül G1, Altınel Y1, Yigitbas H1, Öncü M2, Menekşe S3, Çelik A1, Çelebi F1 and Gulcicek OB1*
1Department of General Surgery, Bagcilar Training andResearchHospital, Turkey
2Department of Radioloji, Bagcilar Training andResearchHospital, Turkey
3Department of MedicalOncology, Bagcilar Training andResearchHospital, Turkey
*Corresponding author: Jeremy Hornibrook, Department of Otolaryngology-Head and Neck Surgery, Christchurch Hospital, 2 Riccarton Avenue, Christchurch 8410 8410 New Zealand
Published: 30 Aug, 2016
Cite this article as: Hornibrook J, Wells S, Finnis N, Gibbs
D. Late Metastatic Pontine Melanoma
Presenting as Ataxia. Ann Clin Case
Rep. 2016; 1: 1171.
Abstract
We report a un usual case of 45-year-old man was admitted to the neurosurgery clinic with the complaint of back pain for 5 months. A tumor was detected at the corpus of L2 vertebra by the lumbar MRG and the lumbar BT. The histopathological result was compatible to the metastasis of follicular thyoid carcinoma. The patient underwent total thyroidectomy and the pathological result was verified as FTC. These attempts were followed by ablation with 150 mCi radioactive iodine (131I).
Keywords
Follicular thyroid carcinoma; Metastasis; Vertebrae
Introduction
Thyroid nodules are a common clinical problem, and differentiated thyroid cancer is becoming
increasingly prevalent [1]. Thyroid carcinoma includes 5 histological subtypes: papillary thyroid
carcinoma, follicular thyroid carcinoma (FTC), medullary thyroid carcinoma, undifferentiated
carcinoma and poorly differentiated carcinoma. Papillary thyroid carcinoma is a major differentiated
subtype that has slow growing characteristics and a good prognosis. Follicular thyroid carcinoma is
another differentiated subtype that compared to papillary thyroid carcinoma has a greater tendency
to distant metastasis to such organs as lung and bone.
Follicular thyroid carcinoma (FTC) accounts for 10–20 % of differentiated thyroid carcinomas
(DTCs), and it is the second most common malignant tumor originating from the follicular cells of
the thyroid [2,3]. In iodine-deficient areas, the relative rate of FTC tends to be higher, up to 40 %
of all cases of DTC [4]. Female to male ratio is 3/1. The incidence increases with age 50 and over.
When FTC is diagnosed, 25% of them show the extra-thyroidal invasion, 5-10% of them show the
metastasis of locally lymph nodes, and 10-20% of show distant metastasis such as lung and bone.
According to the World Health Organization (WHO) classification of thyroid tumors, FTC is
defined by the presence of capsular and/or vascular invasion and by the absence of nuclear features
typical of papillary thyroid carcinoma (PTC) [5]. FTC is more likely to metastasize to distant organs
rather than to regional lymph nodes because of its tendency to invade blood vessels thus resulting
in hematogenous dissemination [6].
Metastatic disease is the primary cause of cancer mortality for most solid tumors including
thyroid cancer [7].
Distant metastatic disease is present at presentation in only 3-15% of patients with thyroid
cancer, but develops later in 6-20% of patients [8]. Distant metastasis is relatively uncommon in
thyroid cancer and when it occurs, long-term stable disease is the typical clinical course. Metastatic
tumors are the most common tumors of the spine, accounting for 98% of all spine lesions.
Spinal cord compression as the initial presentation of metastatic occult follicular carcinoma
without any thyroid enlargement is unusual and relatively rare. Because of this rarity, we aimed to
present this case.
Case Presentation
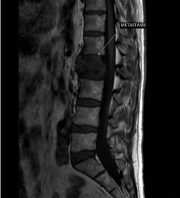
A 45-year-old man was admitted to the neurosurgery clinic with the complaint of back pain for 5 months. Neurological examination was unremarkable. Routine blood tests and thyroid function tests were also within normal limits. The patient’s bladder and bowel habit was normal, with no known co-morbidities. The patient had no history of hypertension, diabetes mellitus, bronchial asthma, tuberculosis, jaundice or any neck swelling. The patient had no history of smoking or alcohol intake. A tumor was detected at the corpus of L2 vertebra by the lumbar MRG and the lumbar BT. There was no motor dificency. Laseuge’s sign was negative. There were hipoesthesia at the left side of L1-2. True-cut biopsy was done from L2 (Figure 1) and the histopathological result was the metastasis of carcinoma. Tumoral excision was done by the neurosurgeons. Expandable cage was used for L2 total corpectomy and stabilization. The histopathological result was compatible to the metastasis of follicular thyroid carcinoma. In blood test, the patient was euthyroid and before thyroidectomy, thyroglobulin level was >500 IU/mL, like after the thyroidectomy operation. The patient underwent an operation of total thyroidectomy 20 days later and the pathological result was verified as FTC. These attempts were followed by ablation with 150 mCi radioactive iodine (131I). External beam irradiation or targeted therapy were not be applied. Patient made an uneventful recovery. The patient has still received the radioiodine therapy.
Discussion
Follicular thyroid carcinomas (FTC) are subtypes of thyroid
cancers which are slow growing tumors and are associated with a
favorable prognosis except when they present with distant metastasis
[9]. Lung and bone are the two most favored sites of metastases [10]. Bone metastases from FTC tend to be multiple and more often to the
ribs, vertebra and sternum [11].
While the 10-year survival rate is 80-95% for patient
with differentiated thyroid carcinoma, survival rate decreases
approximately 40% for patients with distant metastasis. In the 25% of
FTC patient over the age 40, distant tumoral metastasis is detected. The
treatment algorithm for primary thyroid carcinomas includes nearly
total or total thyroidectomy, followed by oral administration of 131I
and TSH suppression [9] Combined use of current multi-disciplinary
treatment option is expected to provide the better prognosis even
in the distant metastasis of thyroid carcinomas. Early diagnosis and
initiation of the treatment should promise a good prognosis for a patient with metastatic vertebra. But, vertebral metastasis of occult
follicular carcinoma without any thyroid enlargement or without any
thyroid related symptoms is unusual and relatively rare metastasis to
the bone, specifically to the vertebral column, may present as bone
pain, pathological fracture, or cord compression and is frequently a
surgical issue. The literature review showed most of the metastatic
follicular carcinoma had obvious thyroid swelling and many cases
had previous thyroid surgery.
Figure 1
Conclusion
In conclusion, metastatic thyroid carcinoma should be considered in the differential diagnosis of every patient with new onset spinal cord compression.
Acknowledgement
Present case was presented in 20th National Surgery Congress, Antalya 2016. (poster presentation).
References
- Cooper DS, Doherty GM, Haugen BR, Kloos RT, Lee SL, Mandel SJ, et al. Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid. 2009; 19: 1167–1214.
- Asari R, Koperek O, Scheuba C, Riss P, Kaserer K, Hoffmann M, et al. Follicular thyroid carcinoma in an iodine-replete endemic goiter region: a prospective collected, retrospectively analyzed clinical trial. Ann Surg. 2009; 249: 1023–1031.
- Ito Y, Hirokawa M, Masuoka H, Yabuta T, Fukushima M, Kihara M, et al. Distant metastasis at diagnosis and large tumor size are significant prognostic factors of widely invasive follicular thyroid carcinoma. Endocr J. 2013; 60: 829–833.
- De Crea C, Raffaelli M, Sessa L, Ronti S, Fadda G, Bellantone C, et al. Actual incidence and clinical behavior of follicular thyroid carcinoma: an institutional experience. Sci World J. 2014. article ID 952095.
- DeLellis RA, Lloyd RV, Heitz PU, et al. World Health Organization classification of tumors: pathology and genetics of tumors of endocrine organs. Lyon: IARC Press; 2004. 64–66.
- Kim HJ, Sung JY, Oh YL, Kim JH, Son YI, Min YK, et al. Association of vascular invasion with increased mortality in patients with minimally invasive follicular thyroid carcinoma but not widely invasive follicular thyroid carcinoma. Head Neck. 2014; 36: 1695-1700.
- Kitamura Y, Shimizu K, Nagahama M, Sugino K, Ozaki O, Mimura T, et al. Immediate causes of death in thyroid carcinoma: clinicopathological analysis of 161 fatal cases. J Clin Endocrinol Metab. 1999; 84: 4043-4049.
- Nixon IJ, Whitcher MM, Palmer FL, Tuttle RM, Shaha AR, Shah JP, et al. The impact of distant metastases at presentation on prognosis in patients with differentiated carcinoma of the thyroid gland. Thyroid. 2012; 22: 884- 8889.
- Cobin RH, Gharib H, Bergman DA, Clark OH, Cooper DS, Daniels GH, et al. AACE/AAES medical/surgical guidelines for clinical practice: management of thyroid carcinoma. American Association of Clinical Endocrinologists. American College of Endocrinology. Endocr Pract. 2001; 7: 202-220.
- Schlumberger M, Tubiana M, De Vathaire F, Hill C, Gardet P, Travagli JP, et al. Long-term results of treatment of 283 patients with lung and bone metastases from differentiated thyroid carcinoma. J Clin Endocrinol Metab. 1986; 63: 960-967.
- Zettinig G, Fueger BJ, Passler C, Kaserer K, Pirich C, Dudczak R, et al. Long-term follow-up of patients with bone metastases from differentiated thyroid carcinoma -- surgery or conventional therapy? Clin Endocrinol (Oxf). 2002; 56: 377-382.