Case Report
Hyperglycemia Induced Reversible Hemiballismus as the Main Presentation of Newly Diagnosed Diabetes Mellitus
Tahir H*, Alkilani WZ, Gibb N, Ullah S and Vinod NR
Department of Internal Medicine, Temple University, USA
*Corresponding author: Hassan Tahir, Department of Internal Medicine, Temple University/ Conemaugh Memorial Hospital, Johnstown, PA 15905, USA
Published: 24 Aug 2016
Cite this article as: Tahir H, Alkilani WZ, Gibb N, Ullah S,
Vinod NR. Hyperglycemia Induced
Reversible Hemiballismus as the Main
Presentation of Newly Diagnosed
Diabetes Mellitus. Ann Clin Case Rep.
2016; 1: 1097.
Abstract
Objective: Diabetes Mellitus commonly presents as polyuria, polydipsia, fatigue and polyphagia, though patients presenting with acute complications at the time of diagnosis are not uncommon. Stroke and
neuropathies are the most common neurological complications of diabetes. Movement disorder
like chorea and hemiballismus are very rarely associated with diabetes mellitus. Primary care
physicians should be aware of these rare and complicit presentations of diabetes. We present a case
of nonketotic hyperglycemic hemiballismus (NHH) with no acute abnormality seen on MRI brain.
Keywords: Hemiballismus; Hyperglycemia; Non-ketotic hemichorea hemiballismus
Introduction
Diabetes Mellitus is the most common endocrine disorder, which presents mainly as polyuria, polydipsia and polyphagia. However, it can rarely present initially with acute complications like diabetic ketoacidosis and nonketotic hyperosmolar coma. Stroke and neuropathies are one of the most common neurological complications of diabetes, which usually occur after long term uncontrolled diabetes. Movement disorders like chorea, athetosis and hemiballismus have many causes but are rarely seen in uncontrolled diabetes mellitus. We present a case of 59-year-old male who presented with hemiballismus as the chief complaint of new onset diabetes mellitus.
Case Presentation
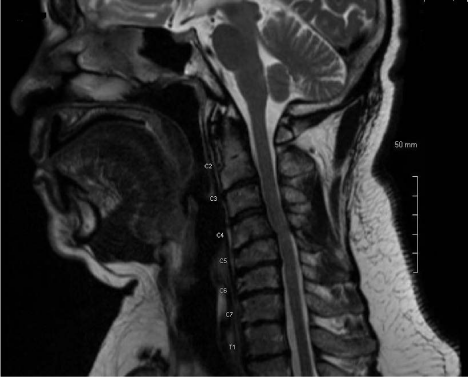
A 59-year-old African American male with the past history of hyperlipidemia and cervical
radiculopathy presented to the emergency department(ED) with new onset involuntary left upper
extremity movements. He had presented to emergency a couple of days ago for evaluation of neck
and left arm pain when he was found to have multilevel cervical degenerative disc and mild cord
compression at C4-5 on MRI (Figure 1). He was discharged on painkillers and steroids with the
recommendation to follow up with neurosurgery on outpatient basis. He came to ED two days
later with worsening involuntary movements of left upper extremity. These episodes of involuntary
movements started to happen more frequently and to last for longer periods, approximately 20
minutes each .He had to hold his arm down so that it would not move erratically. He also reported
difficulty ambulating, slurred speech and blurred vision occurring during the episodes.
He was hemodynamically stable when he came to ED. On neurological exam, he was found to
have rapid involuntary wide flailing movements of left arm, which lasted for few minutes and were
non suppressible. Pupils were equal and reactive to light; and Cranial nerves 2-12 were intact. Power
was 5/5 in all extremities and sensations were intact bilaterally. Cerebellar testing showed marked
dysmetria on finger-to-nose and heel-to-shin testing on the left side of the body. He had CT scan of
head in ED, which did not show any acute intracranial pathology. Baseline investigations showed
glucose level of 598 mg/dl and beta hydroxybutyrate level of 2.27. No acidosis was found on ABGs
and rests of the labs were unremarkable. Patient did not have any history of diabetes, though he did
have family history of diabetes in mother. He was experiencing polyuria and polydipsia for 2 weeks
prior to presentation which had worsened since he had been started on the dexamethasone 2 days
ago for his cord compression. He was given IV fluids and started on insulin.
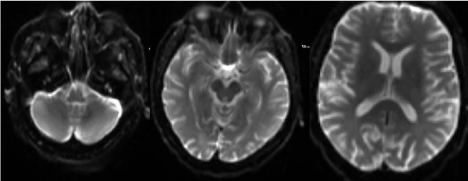
He had extensive work up to find the cause of hemichorea/hemiballismus. He underwent MRI
and MRA of brain that were unremarkable (Figure 2). Prolactin, TSH, liver function, urine drug screen and ESR were all normal. EEG was also done to rule out seizure, which came back normal
with no epileptical focus. Echocardiography showed LV EF 60-65% with normal systolic function.
Carotid Doppler showed mild stenosis of the right and left internal carotid arteries in the range of
1-40%. For his recent diagnosis of mild cord compression, neurosurgery was consulted that did not feel that his symptoms in the left upper extremity were related to the findings in his cervical MRI. In the mean time, hyperglycemia was
treated with insulin and subsequently a level of 200-300 was achieved
throughout hospital stay. HBA1c was found to be 15%. Surprisingly
his symptoms improved with less frequent episodes in next 24 hours
and with complete resolution of symptoms in 2 days. His blurred
vision and slurred speech episodes also resolved completely. Repeat
neurological examination revealed normal motor/sensory system and
cerebellar functions. He was discharged on metformin and insulin.
He did not have any more symptoms on follow up in clinic.
Figure 1
Discussion
Hemichorea-hemiballism (HCHB) is a hyperkinetic disorder
characterized by continuous, non patterned, proximal, involuntary
movements on one side of the body, resulting from involvement of
the contralateral basal ganglia and particularly the striatum. HCHB
can be manifested as the first presentation or a complication of
DM [1]. It is the main presenting symptom in this reported case.
HCHB can be classified into primary or acquired; each contains a
long list of etiologies. Hypoglycemia, hypernatremia, hyponatremia,
hypomagnesemia, and hypocalcemia also represent some of metabolic
portion of acquired etiologies [2]. It can also be a manifestation of
hypoglycemia [3].
Nonketotic hyperglycinemia can present with multiple
neurological symptoms including hyperosmolar coma, seizures and
hemichorea/hemiballismus. Other manifestations can be delirium,aphasia, hemiparesis, hemisensory loss, nystagmus, and hemianopia
[4].Nonketotic hyperglycinemia is a rare cause of chorea/ballism
and bright basal ganglia on MRI that is reported most frequently
in elderly Asian females with type II DM, although it occurs in
other patient population [5,6]. Underlying pathophysiology is not
fully understood yet. Peticheal hemorrhage, microcalcifications,
edema, reactive astrocytic, and interneuronal responses have been
studied as possible etiologies. Ischemic events, blood brain barrier
disruption and neuronal apoptosis all have been also implicated in
the pathophysiology of this condition [7]. MRI is the mainstay to
pick putamen and/or caudate changes. Hyperintensity of T1 is the
most consistent finding. Other findings include hypointensity on T2/
flair and restricted diffusion on DWI. Subtle hyperdensity in striatal
region can also be seen on CT scan. These imaging findings resolve
but slower than clinical improvement, which can explain some cases
of positive imaging findings without clinical manifestations. MRI
without acute changes is also reported in non-ketotic hyperglycemic
HC-HB [8].In contrast, acute basal ganglia changes on MRI are noted
in some cases of asymptomatic non-ketotic hyperglycemia [9].
Control of patient symptoms can be readily achieved by serum
glucose level normalization, although radiographic evidence may
take up to 6 months to resolve [10]. In refractory and severe cases,
haloperidol, risperidone and possibly topiramate and benzodiazepines
can be used among other agents mainly atypical antipsychotics [4,5].
Generally, prognosis is excellent with prompt identification and
management.
In our case, symptoms described were typical for hemiballismus/
hemichorea in the setting of nonketotic hyperglycemia secondary to
newly diagnosed DM augmented by steroid use. Control of patient
symptoms was gradually obtained by controlling hyperglycemia.
Extensive work up was done to find the cause of movement disorder.
All laboratory and radiological investigation were unremarkable.
Spinal cord compression was not a likely cause of our patient
symptoms as he was also having slurred speech, blurry vision and
signs of cerebellar dysfunction during episodes of abnormal arm
movement. His symptoms in the presence of hyperglycemia that got
resolved with insulin treatment led to the diagnosis of hyperglycemia
induced reversible hemiballismus. Interestingly, hemiballismus was
the main presenting symptom of DM. Although there were no acute
changes on radiographs that would suggest NHH but the presentation
was typical as hemiballismus resolved almost 24 hours after initiation
of insulin therapy.
Conclusion
1. Non ketotic hyperglycemic hemiballismus is a rare presentationof diabetes mellitus which should be considered in any patient wit sudden onset movement disorder.
2. Severe hyperglycemia can cause a variety of acute neurological
complications such as cerebellar dysfunction and movement disorders.
Brain imaging may be normal in such cases. These complications are
most of the times reversible with correction of hyperglycemia.
3. Primary care physicians should be aware of rare presentations
of diabetes.
Figure 2
References
- Sayantan Ray, Sukharanjan Howlader, Sumit Chakraborty, Partha Pratim Chakraborty, Sujoy Ghosh. Hemichorea-Hemiballism as the First Presentation of Type 2 Diabetes. Clin Dia. 2015; 33: 87-89.
- Bhidayasiri R, Truong DD. Chorea and related disorders. Postgrad Med J. 2004; 80: 527–534.
- Hefter H, P Mayer, R Benecke. Persistent Chorea after Recurrent Hypoglycemia. Eur Neurol. 2008; 33: 244-247.
- Mary Kate McCullen, Jeffrey Miller, Serge Jabbour, Kevin Furlong, Monika Shirodakar, IntekhabAhmed, Steven Mandel. Expert Opinion: Chorea in the Setting of Hyperglycemia: A case report and review of literature. Pract Neurol. April 2010.
- Dewey RB Jr, Jankovic J. Hemiballism-hemichorea: clinical and pharmacologic findings in 21 patients. Arch Neurol. 1989; 46: 862–867.
- Wilson TJ, Than KD, Stetler WR, Heth JA. Non-ketotic hyperglycemic chorea-hemiballismus mimicking basal ganglia hemorrhage. J Clin Neurosci. 2011; 18: 1560-1561.
- Yeting Zhou, Guangsheng Wang, Xiaodong Chen, Tonghui Yang, Yuanwei Wang, Chunhong Chang, et al. Hemichorea in nonketotic hyperglycemia: Putamenal and cerebellum lesion on MR imaging. World J Neuro sci. 2012; 2: 138-140.
- D Branca, O Gervasio, E le Piane, C Russo, U Aguglia. Chorea induced by non-ketotichyperglycaemia: a case report. Neurological Sci. 2005; 26: 275–277.
- Barry G. Hansford, Dara Albert, Edward Yang. Classic neuroimaging findings of nonketotic hyperglycemia on computed tomography and magnetic resonance imaging with absence of typical movement disorder symptoms (hemichorea-hemiballism). J Radiol Case Rep. 2013; 7: 1-9.
- Damani A, Ghoshal A, Salins N, Deodhar J, Muckaden MA. Management of HemichoreaHemiballismus Syndrome in an Acute Palliative Care Setting. Ind Jour of Palliative Care. 2015; 21: 72-75.