Case Report
Emergency Department Thoracotomy for Intra-abdominal Exsanguination: A Case Report of Inferior Vena Cava Injury
Kuuskne M1*, Barbic D1*, Azzam MH2 and Nemeth J3
1McGill University Health Centre, Emergency Medicine Residency Program, Canada
2McGill University Health Centre, Critical Care Fellowship Program, Canada
3Department of Emergency Medicine, McGill University Health Centre, Canada
*Corresponding author: Martin Kuuskne, McGill University Health Centre, Emergency Medicine Residency Program Montreal, Canada, David Barbic, McGill University Health Centre, Emergency Medicine Residency Program Montreal, Canada
Published: 12 Aug, 2016
Cite this article as: Kuuskne M, Barbic D, Azzam MH,
Nemeth J. Emergency Department Thoracotomy for Intra-abdominal Exsanguination: A Case Report of Inferior Vena Cava Injury. Ann Clin Case Rep. 2016; 1: 1078.
Abstract
Background: Emergency department thoracotomy (EDT) is a rare and potentially lifesaving
procedure. Although the survival rate for EDT is generally low, there exist guidelines containing
specific indications for its use in a subset of patients with penetrating traumatic injuries. Injury to
the inferior vena cava and subsequent intra-abdominal exsanguination due to penetrating trauma
is associated with a high mortality rate however the use of EDT for such injuries remains to be
adequately investigated.
Objectives: To review the indications for and use of EDT, especially in relation to penetrating
abdominal injuries, and to discuss the natural history and progression of injuries to the inferior
vena cava.
Case Report: A 28-year-old male presented to the Emergency Department after sustaining a stab
to the thoracoabdominal region. A focused assessment with sonography for trauma (FAST) was
positive for intra-abdominal free fluid. The patient was found to be persistently hypotensive despite
aggressive fluid resuscitation and massive transfusion. An EDT was preformed for suspected intraabdominal
exsanguination and the patient was transferred to the operating room where he was
treated for an extensive inferior vena cava laceration. After a complicated intensive care unit course,
the patient ultimately survived with full preservation of neurologic function.
Conclusion: The use of EDT is associated with a low rate of survival in penetrating abdominal
trauma but its appropriate and timely use by emergency physicians can be lifesaving.
Keywords: Emergency department thoracotomy; Inferior vena cava injury; Penetrating trauma
Introduction
Penetrating trauma is a relatively infrequent presentation to the Emergency Department
(ED) and those patients presenting with penetrating injuries requiring resuscitative emergency
department thoracotomy (EDT) are even less common [1]. The American College of Surgeons (ACS)
Committee on Trauma recommends that EDT be utilized for patients with penetrating cardiac,
thoracic or abdominal injuries who experience traumatic arrest or unresponsive hypotension. This,
however, must include observed or objectively measured signs of life upon arrival in the ED or
short transport times [2]. Despite current guidelines, a recent retrospective analysis completed at a
Canadian level 1 trauma centre revealed that approximately one half of EDTs were completed for
inappropriate indications [1].
While variations exist, the overall survival rates for EDT performed for penetrating and blunt
trauma are 11% and 1.6%, respectively [2]. The mechanism of injury, the location of the injury,
and the presence or absence of signs of life on arrival to the hospital all determine and account for
a wide range in survival [3]. There is a paucity of evidence within the medical literature of patients
surviving after EDT performed for massive abdominal hemorrhage [4] and even less evidence for
patients surviving EDT for penetrating injuries to the inferior vena cava (IVC) [5,6].
Case Report
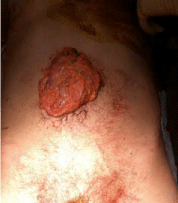
A 28 year-old male was transported to the ED via ambulance after sustaining a stab wound to the anterior thoracoabdominal region. On arrival, the patient was responsive but lethargic, diaphoretic and had bowel evisceration from the wound site (Figure 1). His initial blood pressure (BP) was 74/47 with a heart rate of 93 and an oxygen saturation of 93% on a 100% non-rebreather mask with a respiratory rate of 24. The patient’s airway was secured with endotracheal intubation. A focused assessment with sonography for trauma (FAST) was positive for intra-peritoneal fluid within Morrison’s Pouch. The sub-xiphoid cardiac, spleno-renal and suprapubic view were negative for pericardial fluid and intra-peritoneal fluid, respectively. After the initiation of our massive transfusion protocol and receiving the first unit of packed red blood cells (pRBCs) via a level 1 rapid infuser, the patient’s BP was 67/42. The patient was noted to be exceptionally challenging to bag ventilate and, subsequently, bilateral tube thoracostomies were undertaken with no spontaneous return of blood. The patient had received 4 units of pRBCs and had a blood pressure of 40/31 with a pulse of 50 when the attending emergency physician decided to perform an ED thoracotomy for suspected intra-abdominal exsanguination. A left antero-lateral thoracic incision followed by a vertical pericardiotomy revealed no active bleeding within the left hemi-thorax or blood within the pericardium. A naso-gastric tube was inserted and the thoracic aorta was identified and then cross-clamped which resulted in an immediate improvement of the patient’s hemodynamic status; his BP was 100/69 with a pulse of 62. The patient was transported immediately to the operating room (OR) where the massive transfusion protocol was continued. He received a total of 26 units of pRBCs, 25 units of platelets, 21 units of fresh frozen plasma and 20 units of cryoprecipitate. The patient was surgically treated for an extensive inferior vena cava laceration and lacerations of the gastric pylorus, liver and gallbladder. The patient was defibrillated with intrathoracic paddles twice for cardiac arrest intraoperatively. After surgical stabilization the patient was transferred to the ICU with a packed and open abdomen on norepinephrine, vasopressin and epinephrine intravenous drips and having received tranexamic acid. In the subsequent weeks, the patient returned to the OR on multiple occasions for attempted abdominal closure and was successfully weaned from vasopressors. After a two-month course in the intensive care unit, complicated by an external high-output duodenal fistula and IVC thrombosis, the patient was eventually weaned from mechanical ventilation after further surgical treatment of his intra-abdominal injuries. He was successfully discharged from the ICU to a regional hospital closer to the city of his residence for continued rehabilitation with no neurological impairment.
Figure 1
Discussion
Traumatic injuries to the IVC are notoriously lethal. Whether caused by blunt or penetrating mechanisms, approximately 50% of patients with IVC wounds die before reaching the hospital [7]. In terms of penetrating trauma, gunshot wounds (GSW) produce a much more destructive pattern of IVC avulsion in contrast to the typical linear lacerations inflicted by stab wounds. As with our patient, the majority of penetrating trauma causing IVC injury is accompanied by injury to other abdominal organs, major vessels, or both [8]. It is due to the additional injury of surrounding structures that would otherwise contain the low-pressure IVC hemorrhage that allows caval injuries to cause major hemorrhage and exsanguination. Also, the pattern of injury determines the extent that the IVC may self-tamponade; a phenomenon more likely to occur with oblique GSW and linear stab wounds [7]. While it is common for patients with IVC injury and initial hemodynamic compromise to improve with intravenous fluid resuscitation [9] failure to respond to attempts at volume repletion indicates continued active bleeding and exsanguination. Our case-report demonstrates the utility and effectiveness of EDT in penetrating abdominal trauma with suspected intra-abdominal exsanguination. The rationale of EDT in penetrating abdominal trauma is to ensure adequate cerebrovascular and cardiovascular perfusion while decreasing distal hemorrhage by cross-clamping the thoracic aorta. This principle applies to exsanguination due to both venous and arterial sources of hemorrhage. A meta-analysis by Rhee et al. demonstrated a survival rate of 7.4% after EDT preformed for penetrating abdominal trauma with intra-abdominal exsanguinations [10]. The authors find this survival rate significant enough to consider performing EDT in similar conditions. Our case also highlights the role that the emergency physician plays in the initial treatment of a time sensitive injury with an exceedingly low survival rate before the involvement of a designated surgical trauma service. However, the procedure should only be considered in a centre with adequate and established trauma surgery services.
Conclusion
Penetrating abdominal injuries with persistent hypotension despite fluid resuscitation is suggestive of ongoing intra-abdominal hemorrhage. We presented the case of a 28-year-old man with a penetrating abdominal injury and suspected intra-abdominal exsanguination secondary to an inferior vena cava laceration in whom an EDT proved pivotal to his survival. Although a rare procedure in the emergency department, it is essential that emergency physicians become familiar with the ACS recommended indications for EDT as well as its utility is suspected intra-abdominal exsanguination due to penetrating abdominal trauma.
References
- Passos EM, Engels PT, Doyle JD, Beckett A, Nascimento B, Rizoli SB, et al. Societal Costs of Inappropriate Emergency Department Thoracotomy. J Am Coll Surg. Elsevier Inc. 2012; 214: 18–25.
- Working Group, Ad Hoc Subcommittee on Outcomes, American College of Surgeons. Committee on Trauma. Practice management guidelines for emergency department thoracotomy. Working Group, Ad Hoc Subcommittee on Outcomes, American College of Surgeons-Committee on Trauma. J Am Coll Surg. 2001; 193: 303–309.
- Seamon MJ, Chovanes J, Fox N, Green R, Manis G, Tsiotsias G, et al. The use of emergency department thoracotomy for traumatic cardiopulmonary arrest. Injury. 2012; 43: 1355–1361.
- Cothren CC, Moore EE. Emergency department thoracotomy for the critically injured patient: Objectives, indications, and outcomes. World J Emerg Surg. 2006; 1: 4.
- Huerta S, Bui TD, Nguyen TH, Banimahd FN, Porral D, Dolich MO. Predictors of mortality and management of patients with traumatic inferior vena cava injuries. Am Surg. 2006; 72: 290–296.
- Burch JM, Feliciano DV, Mattox KL, Edelman M. Injuries of the inferior vena cava. Am J Surg. 1988; 156: 548–552.
- Buckman R, Pathak A, Badellino M, Bradley K. Injuries of the Inferior Vena Cava. Surgical Clinics or North America. 2001; 81: 1431-1437.
- Bricker DL, Morton JR, Okies JE, Beall AC Jr. Surgical management of injuries to the vena cava: Changing patterns of injury and newer techniques of repair. J Trauma. 1971; 11: 725-735.
- Feliciano DY, Bitondo CG, Mattox KL, Burch JM, Jordan GL, Beall AC, et al. Civilian trauma in the 1980s: A one-year experience with 456 vascular and cardiac injuries. Ann Surg. 1984; 199: 717-724.
- Rhee PM, Acosta J, Bridgeman A, Wang D, Jordan M, Rich N. Survival after emergency department thoracotomy: review of published data from the past 25 years. J Am Coll Surg. 2000; 190: 288–298.