Case Report
Successful Endoscopic Third Ventriculostomy in the Presence of an Intraventricular Developmental Venous Anomaly: Case Report
Morgenstern PF1* and Hoffman CE1,2
1Department of Neurological Surgery, New York-Presbyterian Hospital-Weill Cornell Medical Center, USA
2Weill Cornell Medical College, New York, New York, USA
*Corresponding author: Dilek Ertoy Baydar, Department of Pathology, Hacettepe University Hospital, Department of Pathology, Sihhiye / Ankara, 06100 Turkey
Published: 15 Jul, 2016
Cite this article as: Morgenstern PF, Hoffman CE.
Successful Endoscopic Third
Ventriculostomy in the Presence of an
Intraventricular Developmental Venous
Anomaly: Case Report. Ann Clin Case
Rep. 2016; 1: 1028.
Abstract
Cerebral cavernous malformations are commonly associated with a developmental venous anomaly. Sparing this anomaly is considered important as it frequently is part of the venous drainage of normal brain parenchyma. We present a case in which a developmental venous anomaly of the third ventricle associated with a thalamic cavernous malformation increased the degree of difficulty of successful endoscopic third ventriculostomy for management of hydrocephalus. Through a conventional approach with careful pre-operative planning we were able to successfully fenestrate the floor of the third ventricle and spare the abnormal venous complex.
Keywords: Cavernous malformation; Developmental venous anomaly; Endoscopic third ventriculostomy
Introduction
It has been well-documented that cerebral cavernous malformations (CMs) can be associated with a developmental venous anomaly (DVA), as often as 20% of the time by some estimates [1]. The DVA is typically spared at the time of surgery to avoid disruption of venous drainage of normal associated tissue. Depending on the location of the DVA, this can either be straightforward or can present significant challenges to successful operation. We present a case in which an intraventricular DVA associated with a thalamic CM increased the difficulty and influenced surgical decision making for endoscopic third ventriculostomy (ETV).
Case Presentation
History and examination
A six-year-old boy with no significant past medical history presented to the emergency
department and was admitted complaining of one week of headaches with associated nausea and
vomiting. In the 24 hours prior to admission, he became slightly lethargic and his parents noted gait
instability, which prompted the visit to the emergency department.
On admission, he was noted to be lethargic but arousable to voice without any focal neurologic
deficits. Laboratory evaluation was unremarkable, and an MRI of the brain was obtained. The MRI
demonstrated a 1.5 x 1.2 cm mass in the posterior third ventricle and a small amount of hematoma
within the aqueduct causing obstructive hydrocephalus (Figure 1). Intra-lesional hemorrhage
and a DVA identified in the left wall of the third ventricle suggested the diagnosis of a cavernous
malformation of the posterior thalamus.
An external ventricular drain (EVD) was placed on admission and the patient was taken to the
operating room for ETV on hospital day 2 based on the presence of hematoma within the aqueduct
that may not have been visualized and removed with resection of the lesion from a posterior
approach. This procedure would then be followed by resection of the lesion. In deciding to move
forward with ETV to decrease the patient’s risk for post-operative shunting, the location of the
DVA was taken into consideration to avoid injury. A more medial and anterior entry point with
frameless stereotactic navigation was therefore planned to allow for more rightward navigation and
fenestration as well as avoiding working against or directly adjacent to the anomaly.
Operation
The patient was taken to the operating room and positioned supine with the head neutral in
a skull clamp. The EVD incision on the right side was opened and the burr hole widened to accommodate the zero-degree rigid lens endoscope (Minop®, Aesculap®, USA) and to allow for a more medial and anterior entry as discussed above. The zero-degree endoscope was passed into the right lateral ventricle and continuous irrigation was initiated to facilitate insufflation of the ventricle. The ventricular anatomy was visualized and delineated. The endoscope was advanced through the Foramen of Monro into the third ventricle, and the DVA was identified overlying the left hypothalamus. A fenestration site was selected anterior and to the right of the basilar artery. The fenestration was then made in the floor of the third ventricle posterior to the infundibulum just behind dorsum sella using a biopsy forceps. This fenestration was widened using a 3-french embolectomy catheter. Widening of the fenestration was limited by the proximity of the DVA to the fenestration site as well as collapse of the third ventricle on advancing the scope and embolectomy catheter. The embolectomy catheter was withdrawn and the endoscope was advanced to the fenestration site to visualize the pre-pontine cistern. No additional obstructive arachnoid adhesions were identified, and the Membrane of Liliequist was fenestrated. The endoscope was then withdrawn, and the EVD replaced and left clamped for post-operative monitoring.
Postoperative course
The patient was taken to the pediatric intensive care unit (PICU) post-operatively and returned to the operating room on post-operative day (POD) 1 for resection of the cavernous malformation by a supracerebellar infratentorial approach. He was neurologically intact and monitored in the PICU post-operatively and the EVD was removed on POD 3, at which time the patient was discharged home.
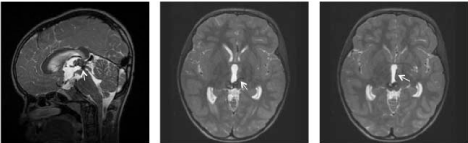
Figure 1
Figure 1
Sagittal t2-weighted MRI demonstrating posterior thalamic cavernous malformation with hemorrhage obstructing the aqueduct of sylvius (arrow, left panel). Axial T2 weighted MRI demonstrating DVA in the left wall of the third ventricle along the hypothalamus and thalamus (arrow, middle and right panels).
Discussion
Cavernous malformations are indolent, vascular lesions that most frequently present clinically with seizures or neurologic deficits associated with hemorrhage [1,2]. DVAs are thought to occur in approximately 20% of pediatric patients with CMs, and represent an independent risk factor for hemorrhage [3]. Thalamic CMs occur in fewer than 10% of all CMs and are grouped with those occurring in the brainstem as a higher risk category as hemorrhage more frequently results in permanent neurologic injury [1-6]. Furthermore, CMs of the brainstem and thalamus identified in childhood have been observed to be larger, with a higher risk for hemorrhage and recurrence than those in other locations [2]. While surgical approaches to these lesions are not without risk, many advocate definitive management when surgically feasible to avoid permanent morbidity from hemorrhage, particularly given the life expectancy of pediatric patients [6]. Surgical approaches have been well documented in the published literature, with the supracerebellar infratentorial approach favored for reaching posterior thalamic/pineal region CMs [3,6]. However, in some cases temporizing management such as CSF diversion may be needed prior to definitive management.
The CM described in this case report presented with hydrocephalus, an uncommon presentation, caused by hemorrhage resulting in obstruction of the aqueduct of Sylvius. Prior to definitive management of the CM, CSF diversion was undertaken in the form of an ETV, as this clot was not necessarily accessible via the surgical approach to the lesion. This case illustrates a situation in which a DVA associated with a CM of the posterior thalamus increased the complexity of operative planning and the technical difficulty of achieving adequate CSF diversion for obstructive hydrocephalus. The presentation of the patient, and initial management, are typical for a pineal region lesion, if not a CM [1]. Recognition of the DVA, however, was important for operative preparation. In this case, the DVA resulted in a narrowing of the interval between the bilateral hypothalami in the anterior third ventricle. The planned entry point, trajectory, and subsequent potential sites of fenestration in the floor were limited, therefore, and required preoperative consideration. Upon entering the third ventricle through the foramen of Monro with a rigid endoscope, the DVA was identified along the wall of the hypothalamus. The initial perforation was straightforward given that the entry point provided the ability to navigate laterally and anteriorly. However, dilation of the ventriculostomy using an embolectomy catheter was limited by the narrowed interval between the bilateral hypothalami due to the presence of the DVA. This limitation required additional care to be taken in expanding the ventriculostomy and necessitated leaving a smaller perforation, but had no impact on the outcome of the operation. The ETV was successful, and the patient recovered well following resection of the cavernous malformation.
We demonstrate a case in which a thalamic CM was found to be associated with a third ventricular DVA. Identification of this anomaly pre-operatively was essential in operative planning, most importantly for CSF diversion in the form of an ETV. While the presence of the anomaly increased the degree of difficulty for performing the ETV, careful preoperative planning with respect to trajectory, fenestration site into the prepontine cistern, insufflation on entering the ventricle, and modification of approach intra-operatively when creating the stoma resulted in successful completion of the procedure without complication.
References
- Gross BA, Du R, Orbach DB. The natural history of cerebral cavernous malformations in children. J Neurosurg Pediatr. 2015; 16: 1-6.
- Abla AA, Lekovic GP, Garrett M, Wilson DA, Nakaji P, Bristol R, et al. Cavernous malformations of the brainstem presenting in childhood: surgical experience in 40 patients. Neurosurgery. 2010; 67:1589-1598.
- de Oliveira JG, Lekovic GP, Safavi-Abbasi S, Reis CV, Hanel RA, Porter RW, et al. Supracerebellar infratentorial approach to cavernous malformations of the brainstem: surgical variants and clinical experience with 45 patients. Neurosurgery. 2010; 66: 389-399.
- Gross BA, Lin N, Du R, Day AL. The natural history of intracranial cavernous malformations. Neurosurg Focus. 2011; 30: E24.
- Li D, Zhang J, Hao S, Tang J, Xiao X, Wu Z, et al. Surgical treatment and long-term outcomes of thalamic cavernous malformations. World Neurosurg. 2013; 79: 704-713.
- Fleming S. Distal nephron neoplasms. Semin Diagn Pathol. 2015; 32: 114-123.
- Rangel-Castilla L, Spetzler RF. The 6 thalamic regions: surgical approaches to thalamic cavernous malformations, operative results, and clinical outcomes. J Neurosurg. 2015; 123: 676-685.