Case Report
A White Tone Sessile Type Polyp: Submucosal Invasion Sigmoid Colon Cancer – 6mm in a Diameter
Ogawa M1*, Tomita Y2, Matai K1, Ichihara K1, Hasegawa T1 and Yoshida K1
1Department of Surgery, The Jikei University School of Medicine, Japan
2Department of Endoscopy, The Jikei University School of Medicine, Japan
*Corresponding author: Masaichi Ogawa, Department of Surgery, Katsushika Medical Center, The Jikei University School of Medicine, Tokyo 125-8506, Japan
Published: 04 Jul, 2016
Cite this article as: Ogawa M, Tomita Y, Matai K, Ichihara
K, Hasegawa T, Yoshida K. A White
Tone Sessile Type Polyp: Submucosal
Invasion Sigmoid Colon Cancer – 6mm
in a Diameter. Ann Clin Case Rep.
2016; 1: 1027.
Abstract
A 53-year-old woman received a total colonoscopy for a FOBT and detected a sessile type poly in the sigmoid colon. Colonoscopy exhibited a “somewhat of a white tone” and measured 6mm sessile type poly, with no irregular pit pattern, and suspected an adenoma. Also, endoscopic mucosal resection was done. The pathological diagnosis was a well differentiated adenocarcinoma and the depth of invasion was 1,200 micron. Submucosal invasive adenocarcinoma with 6mm, non-depressive sessile type case is very rare. Therefore, one should recommended an endoscopic mucosal resection, not observation, when the endoscopic findings was recognized a “white tone” sessile type polyp.
Case Presentation
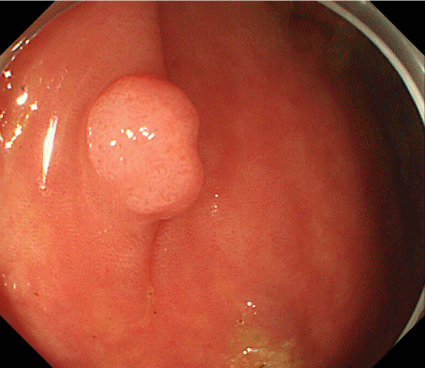
A 53-year-old woman received a total colonoscopy for a FOBT and detected a sessile type poly
in the sigmoid colon. The lesion measured 6mm and performed an endoscopic mucosal resection.
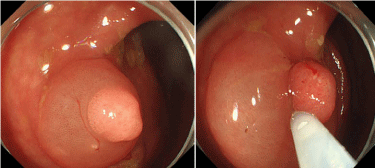
Colonoscopy exhibited a “somewhat of a white tone” sessile type poly, no irregular pit pattern was
identified, and suspected an adenoma (Figure 1 and 2).
What is your diagnosis?
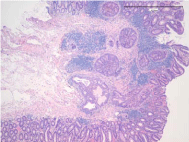
The pathological diagnosis was a well differentiated adenocarcinoma and the depth of invasion
was 1,200 micron (Figure 3). Laparoscopic-assisted sigmoidectomy was performed and the resected
specimen demonstrated no residual cancer, no lymphovascular invasion and no lymphnode
metastasis.
Discussion
There have been some reports about small depressed type colorectal cancer invading the
submucosal layer [1-3]. Predicting an increased risk of submucosal invasion on the basis of a lesion's
endoscopic appearance is now feasible for all endoscopists as a result of concomitant advances
including the following:
1. Standardized definitions of polyp descriptors (Paris classification, granularity, pit pattern).
2. Higher definition endoscopes providing sufficient visual resolution to enable accurate
classification with white-light endoscopy alone.
3. Evidence from Japanese studies that these classifications can stratify for the risk of
invasion [4,5]. Therefore, our 6mm non depressive sessile type case is very rare. Therefore, one should recommended an endscopic mucosal resection, when the endscopic findings was recognized a “white tone” sessile type polyp.
Figure 1
Figure 2
Figure 3
Figure 3
Histologic appearance of the resected specimen showing a well differentiated adenocarcinoma and the depth of invasion was 1,200 micron.
References
- Facciorusso A, Antonino M, Di Maso M, Barone M, Muscatiello N. Non-polypoid colorectal neoplasms: Classification, therapy and follow-up. World J Gastroenterol. 2015; 21: 5149-5157.
- Youk EG, Sohn DK, Hong CW, Lee SD, Han KS, Kim BC, et al. Early Outcomes of Endoscopic Submucosal Dissection for Colorectal Neoplasms According to Clinical Indications. Dis Colon Rectum. 2016; 59: 403-410.
- Shibagaki K, Amano Y, Ishimura N, Yuki T, Taniguchi H, Fujita H, et al. Magnification endoscopy with acetic acid enhancement and a narrow-band imaging system for pit pattern diagnosis of colorectal neoplasms. J Clin Gastroenterol. 2015; 49: 306-312.
- M.J. Bourke. Current status of colonic endoscopic mucosal resection in the West and the interface with endoscopic submucosal dissection. Dig Endosc. 2009; 21: 27-32.
- Moss A, Bourke MJ, Williams SJ, Hourigan LF, Brown G, Tam W, et al. Endoscopic mucosal resection outcomes and prediction of submucosal cancer from advanced colonic mucosal neoplasia. Gastroenterology. 2011; 140: 1909-1918.