Case Report
Solitary Fibrous Tumour of the Mesorectum: About a Case with Review of the Literature
Haydar A. Nasser1*, Chalhoub D2, Mendes VM1, Gomez M1 and Bouazza F1
1Department of Surgical Oncology, Jules-Bordet Institute, Belgium
2Department of General and Digestive Surgery, Hotel Dieu de France, Lebanon
*Corresponding author: Haydar A. Nasser, Department of surgical oncology, Jules-Bordet Institute, Brussels, Belgium
Published: 08 Jun, 2016
Cite this article as: Nasser HA, Chalhoub D, Mendes VM,
Gomez M, Bouazza F. Solitary Fibrous
Tumour of the Mesorectum: About a
Case with Review of the Literature. Ann
Clin Case Rep. 2016; 1: 1017.
Abstract
Solitary Fibrous Tumours (SFTs) are rare entities that are most commonly seen in the pleura. However, SFTs could affect different organs and tissues. Pelvic SFTs are rarely reported in the literature and para-rectal ones are even rarer. We present here a case of a 43 –year-old lady with continuous nonspecific pelvic pain and fullness. Para clinical investigations were consistent with a well-demarcated mass in the perirectal region. Despite some radiologic features that were consistent with a GIST, however the diagnosis was unsure. After successful laparoscopic resection, histopathology was consistent with SFT.
Keywords: Spindle cell tumors; Solitary fibrous tumours
Introduction
SFT can be seen in different locations throughout the human body, that could extend from the Head and neck [1] to the ischio-anal fossa [2,3]. These spindle cell tumours were reported firstly in the pleura in 1931 [4]; extrathoracic SFTs were identified later on [1,5,6]. Inrathoracic and extrathoracic SFTs could metastasize or recur. Pelvic SFTs including anorectal ones, are very rare. Preoperative diagnosis is difficult, and only in few cases paraclinical investigations have led to accurate diagnosis [7-9].
Case Presentation
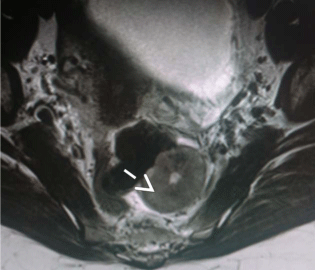
A 43-year-old lady presented with six months history of pelvic pain and heaviness. Axial T2
weighted MRI showed a well demarcated left Para-rectal mass about 5 cm × 4.5 cm, 12 cm from
the anal verge (Figure 1). There were no signs of necrosis or local extension. Thoracoabdominal
CT-scan showed no evidence of metastasis. Endoscopic ultrasound showed an oval shaped mass
developing just beneath the muscular layer of the rectum. The FNA analysis was not contributive.
After discussing the case during the Digestive Oncology meeting, we decided to perform an
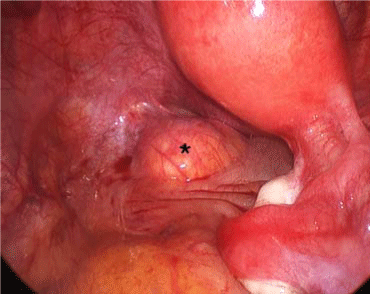
exploratory laparoscopy with an attempt to excise the mass. At laparoscopy, the mass was situated
in the sub peritoneal space, just at the level of the cul de sac of Douglas (Figure 2). It was just
below the peritoneal reflection, at the level of the upper part of the rectum, situated at the left side
of the rectum. Laparoscopic excision was done successfully and sent for pathology analysis. The
rectum was kept intact. On gross pathology, the tumor sized 4 x 2 x 2 cm, of white colour with some
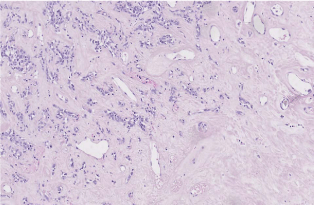
areas of calcifications. Histopathologically, it consisted of spindle
cells, arranged arbitrarily within hypocellular and hypercellular areas
(Figure 3). Vascularization was abundant with hemangiopericytoma
features. Cells showed poor mitotic activity. Resection margins were
free of disease. The post-operative course was uneventful and the
patient is asymptomatic after one year of follow-up.
Figure 1
Figure 2
Figure 2
T2 weighted axial MRI, showing a well circumscribed oval mass
(white arrow) with central hyperintensity zone.
Figure 3
Discussion
SFTs were first described in the thoracic pleura in 1931 [4];
however many other sites have been reported in the literature. SFTs
are rare, with an incidence of 0.2/100000/year [9]. Pelvic SFTs are
even rarer, with only about 34 cases available on PubMed database
(using the search terms "solitary fibrous tumour", "pelvis") [2,3,7-25].
The 1st reported case of pelvic SFT occurred in the bladder and was
published in 1997 [7]. Other pelvic structures included: Seminal
vesicles [1], mesorectum [19], perianal space [2,3,8] and other nonwell
specified pelvic areas [13-18]. Radiologic findings are non specific
for GIST [18], and they are often misdiagnosed with GIST.
Accurate preoperative diagnosis was evoked in 3 reported cases,
where biopsy was performed in 2 cases [7,8], and [7] F-FDG PET/CT
with ultrasound guided biopsy were performed in one case [9]. Some
authors have described obstructive symptoms, such as pollakiuria
[22], urinary retention [8] and constipation [19]. It's Noteworthy to
mention that in 3 reported cases, hypoglycaemia was the alarming
symptoms and was secondary to IGF-2 secreting cells. SFTs generally
show benign behaviour. A recent large retrospective study, where 110
SFT cases were reviewed, 10 year metastasis free rate was 55% [26].
Predictive signs of malignity include: necrosis, high mitotic activity,
cellular atypia and large tumors. Even though, the absence of these
features would not preclude metastasis or recurrence [24]. Surgery
with curative intent is the best treatment option [26]. While Liver
SFTs are treated with 1 cm negative margin resection [27], surgery
with curative intent would be also the best treatment option for pelvic
SFTs [2,3,7-25,27].
In some cases, neoadjuvant chemoradioterapy preceded surgical
resection. To the best of our Knowledge, none of the previously
reported anorectal cases were treated laparoscopically. In one case,
excision was carried out during laparotomy, and in another one
trans-sacral resection was adopted. Yan et al. [11] described recently
FDG PET/CT utility in determining the metabolic activity of such
tumors, and subsequently what treatment regimen should be used
[9]. Dxorubicin may also be proposed as adjuvant therapy [9,25].
Conclusion
Only 3 cases of anorectal SFTs were previously reported, one in
the pararectal area [19], one in the ischioanal fossa [3] and one with
perianal location [2].
Biopsy is not always diagnostic in SFTs, because spindle cells are
arranged haphazardly within the tumor bulk [13]. Since recurrence
and metastasis are of possibility with SFTs, even in the absence of
aggressive signs, thus surgical excision should be mandatory in order
to establish the diagnosis, and to assess the degree of cellular atypia
and mitotic index.
References
- Srinivasan VD, Wayne JD, Rao MS, Zynger DL. Solitary Fibrous Tumor of the Pancreas: Case Report with Cytologic and Surgical Pathology Correlation and Review of the Literature. JOP: Journal of the Pancreas. 2008; 9: 526-530.
- Demicco EG, Park MS, Araujo DM, Fox PS, Bassett RL, Pollock RE, et al. Solitary fibrous tumor: a clinicopathological study of 110 cases and proposed risk assessment model. Mod Pathol. 2012; 25: 1298-1306.
- Perini MV, Herman P, D'Albuquerque LA, Saad WA. Solitary fibrous tumor of the liver: Report of a rare case and review of the literature. Solitary fibrous tumor of the liver: Report of a rare case and review of the literature. International Journal of Surgery. 2008; 6: 369-399.
- Boe J, Chimpiri AR, Liu CZ. Solitary fibrous tumor originating in the pelvis: a case report. J Radiol Case Rep. 2010; 4: 21-28.
- Dudkiewicz M, Deschênes JL, Bloom C, Gordon PH. Solitary fibrous tumor of the ischioanal fossa: report of a case and review of the literature. Dis Colon Rectum. 2004; 47: 535-537.
- Mitsuaki S, Kaku Y, Keiko M, Suzuki K, Dambara T, Uekusa T, et al. Solitary fibrous tumor of the pleura: Ultrasonographic ?imaging findings of 3 cases. Respiratory Investigation. 2013; 51: 200-204.
- Lau SK, Weiss LM, Chu PG. Myxoid solitary fibrous tumor: a clinicopathologic study of three cases. Virchows Arch. 2009; 454: 189-194.
- Wagner S, Greco F, Hamza A, Hoda RM, Holzhausen HJ, Fornara P. Retroperitoneal malignant solitary fibrous tumor of the small pelvis causing recurrent hypoglycemia by secretion of insulin-like growth factor 2. Eur Urol. 2009; 55: 739-742.
- Hata T, Tsuruta Y, Takamori S, Shishikura Y. Non-islet cell tumor hypoglycemia at the second recurrence of malignant solitary fibrous tumor in the retroperitoneum and pelvis: a case report. Case Rep Oncol. 2012; 5: 420-427.
- Shoji S, Nakano M, Yamamoto S, Okada N, Nagata Y, Sekido Y, et al. Surgical resection using retroperitoneal approach for solitary fibrous tumor in the pelvis. Oncol Lett. 2011; 2: 675-677.
- Yan J, Jones RL, Lewis DH, Eary JF. Impact of (18) F-FDG PET/CT imaging in therapeutic decisions for malignant solitary fibrous tumor of the pelvis. Clin Nucl Med. 2013; 38: 453-455.
- Bainbridge TC, Singh RR, Mentzel T, Katenkamp D. Solitary fibrous tumor of urinary bladder: report of two cases. Hum Pathol. 1997; 28: 1204-1206.
- Vallat-Decouvelaere AV, Dry SM, Fletcher CD. Atypical and malignant solitary fibrous tumors in extrathoracic locations: evidence of their comparability to intra-thoracic tumors. Am J Surg Pathol. 1998; 22: 1501- 1511.
- Westra WH, Grenko RT, Epstein J. Solitary fibrous tumor of the lower urogenital tract: a report of five cases involving the seminal vesicles, urinary bladder, and prostate. Human Pathology. 2000; 31: 63-68.
- Ishikawa T, Kawabata G, Terakawa T, Kamidono S, Fujisawa M. Solitary fibrous tumor in the pelvic space. Urol Res. 2004; 32: 49-50.
- Nagase T, Adachi I, Yamada T, Murakami N, Morita K, Yoshino Y, et al. Solitary fibrous tumor in the pelvic cavity with hypoglycemia: report of a case. Surg Today. 2005; 35: 181-184.
- Trastour C, Piche M, Bafghi A, Checchi-Guichard C, Bongain A. Solitary fibrous tumor of the pelvis. Eur J Obstet Gynecol Reprod Biol. 2006; 124: 254-255.
- Joe BN, Bolaris M, Horvai A, Yeh BM, Coakley FV, Meng MV. Solitary fibrous tumor of the male pelvis: findings at CT with histopathologic correlation. Clin Imaging. 2008; 32: 403-406.
- Wat SY, Sur M, Dhamanaskar K. Solitary fibrous tumor (SFT) of the pelvis. Clin Imaging. 2008; 32: 152-156.
- Gessmann J, Seybold D, Helwing M, Muhr G, Schildhauer TA. [Solitary fibrous tumor of the pelvis: a rare extrathoracic manifestation]. Orthopade. 2009; 38: 626-631.
- Katsuno H, Maeda K, Hanai T, Sato H, Masumori K, Koide Y, et al. Transsacral resection of a solitary fibrous tumor in the pelvis: report of a case. Surg Today. 2011; 41: 1548-1551.
- Sueblinvong T, Judson PL, Downs LS, Argenta PA. Solitary fibrous tumors arising from the female pelvis. Obstet Gynecol. 2011; 118: 470-474.
- Tsushimi T, Yagi T, Tomozawa N, Ohnishi H. Retroperitoneal solitary fibrous tumor of the pelvis with pollakiuria: a case report. BMC Res Notes. 2012; 5: 593.
- Baldi GG, Stacchiotti S, Mauro V, Dei Tos AP, Gronchi A, Pastorino U, et al. Solitary fibrous tumor of all sites: outcome of late recurrences in 14 patients. Clinical Sarcoma Research. 2013; 3: 4.
- Hosaka S, Katagiri H, Wasa J, Murata H, Takahashi M. Solitary fibrous tumor in the pelvis: induced hypoglycemia associated with insulin like growth factor II. Journal of Orthopedic Science. 2013.
- Yoshida R, Takada H, Iwamoto S, Uedono Y, Kawanishi H, Yoshioka K, et al. A Solitary Fibrous Tumor in the Perianal Region with a 13-Year FollowUp: Report of a Case. Surgery Today. 1999; 29: 642-645.
- Elbuluk O, Abemayor E, Sepahdari AR. Solitary fibrous tumor of the larynx: case report demonstrating the value of MRI in guiding surgical management. Clin Imaging. 2013; 37: 1119-1121.