Case Report
Trevor Disease: At Lower Tibia with Literature Review
Karuppal R1*, Somasundaran S2 and V Raman RV3
1Department of Orthopaedics, Govt. Medical College, India
2Department of Ophthalmology, Govt. Medical College,India
3Department of Radiology, Govt. Medical College, India
*Corresponding author: Raju Karuppal, Department of Orthopaedics, Govt. Medical College, Kozhikode, 673008, Kerala, India
Published: 17 Jun, 2016
Cite this article as: Karuppal R, Somasundaran S, V
Raman RV. Trevor Disease: At Lower
Tibia with Literature Review. Ann Clin
Case Rep. 2016; 1: 1015.
Abstract
Background: Trevors Disease is a rare developmental bone disorder of childhood. The bones of the ankle joint are most commonly affected. Of them Tibial involvement is less common as compared
with tarsal involvement. We present a localized form Trevors Disease of lower tibial epiphysis.
Methods: A 9 year old who previously does not had any history of trauma presented with bony
swelling from the anteromedial aspect of the lower tibial epiphysis with limitation of ankle
dorsiflexion. The patient underwent radiological imaging followed by surgical excision and tissue
biopsy for establishing the diagnosis. Additionally we collected all the reports of Trevor disease.
Results: At one year follow up there is no recurrence, restriction of movements or ankle joint
dysfunction in our case.
Conclusions: The present study reports a case of localized form Trevors Disease at the lower tibial
epiphysis with one year follow-up. A detailed review of Trevor disease was also performed regarding
the treatment, prognosis, long term function and the areas affected.
Keywords: Ankle; Tibia; Epiphysis; Dysplasia epiphysealis hemimelica; Trevor disease
Introduction
Dysplasia epiphysealis hemimelica (DEH), also known as Trevor disease is a rare skeletal
development disorder of childhood. It characterized by asymmetrical abnormal growth of epiphyseal
cartilage particularly of the lower limbs. The knee and ankle joints are most commonly affected, apart
from the bones of foot. The upper limbs involvement is extremely rare. Clinically and pathologically
Trevor disease has much resemblance with epiphyseal osteochondroma. Mouchet and Belot was
first described this condition in 1926, they called it tarsomegaly [1]. Later Trevor recognized this
condition in 1950, who described 10 cases and put them into one distinct group, naming it tarso
epiphysary aclasia [2]. Then Fairbank renamed Trevor disease as Dysplasia epiphysealis hemimelica
to avoid confusions of the previous unsuitable designations. Trevor is characterized by the presence
of irregular cartilage overgrowth occurs either in the lateral or medial part of the bone (hemimelic)
usually medial. It may be a localized form (affect a single bone, classical form (multiple bones in a
single limb) or generalized form (an entire limb) [3]. The ossification centers develop during growth
period being individually or together. It results in a bone mass as asymmetrical epiphysis resembling
exostoses [4]. The aim of our study was to perform a detailed review of this challenging disease, even
though it is rare.
Case Report
A 9year old boy presented with pain and a swelling and limitation of dorsiflexion of right ankle
in January 2015. He was walking normally except for uphill due to reduced ankle dorsiflexion. Other
than this he was very healthy and there was no history of trauma. Physical examination showed
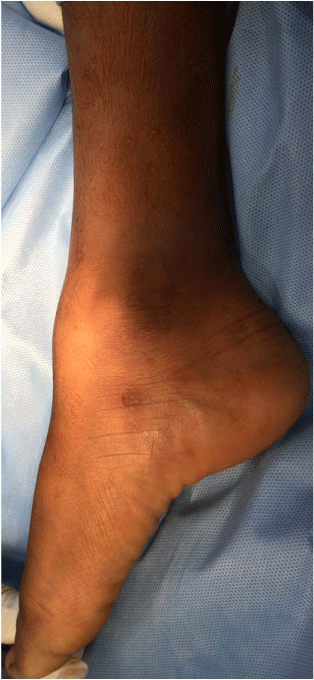
bony hard swelling on the anterior aspect of right ankle joint which was blocking the dorsiflexion
(Figure 1). There were no ankle or foot deformities.
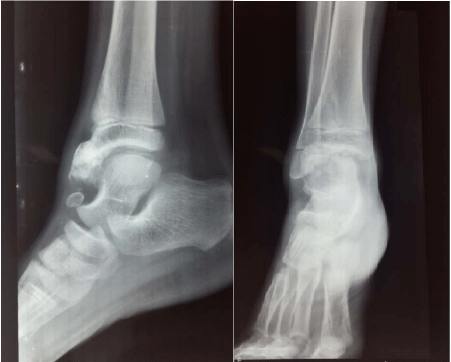
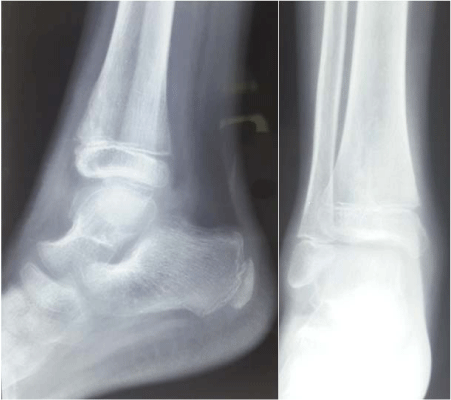
Plain X ray of the right ankle joint shows irregular cartilaginous mass with dense areas similar
to osteochondroma arising from the anterior part of the tibial epiphysis (Figure 2). The fibula, the
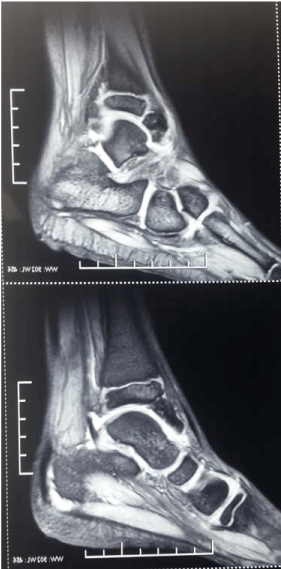
talus, and the other foot were normal. MRI shows bony lesion from the anteroinferior part of lower
tibial epiphysis with epiphyseal irregularity consistent with Trevor disease (Figure 3).
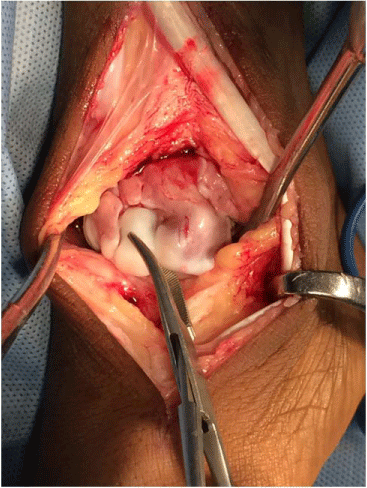
Since the clinical and radiologic findings were corroborative with Trevor's disease and the
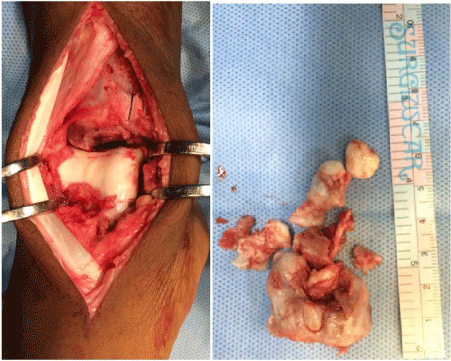
swelling was blocking dorsiflexion, patient underwent surgical procedure through the anterior approach, under general anaesthesia and tourniquet (Figure 4).
The lesion was removed using a broad osteotome from the
anterior and antero medial part, near to the medial malleolus (Figure
5). There was a cartilaginous loose body obtained near to the tibialis
anterior tendon.
Intraoperative dorsiflexion and plantar flexion were checked and
found to be perfectly normal. Articular surfaces were also intact.
The histopathological examination report of the removed
osteochondral fragments was consistent with benign osteochondroma.
Mitotic figures or cellular changes of malignant transformation were
absent.
In the post operative period weight bearing was prohibited for 4
weeks, followed by physiotherapy. No intra-operative or immediate post-operative complications were noted. At 1 year follow-up, the
boy presented with no pain, no disease recidivism and complete joint
function (Figure 6).
Figure 1
Figure 2
Figure 2
X ray right ankle joint AP and Lateral view shows irregular
cartilaginous mass with dense areas arising from the anterior part of the tibial
epiphysis.
Figure 3
Figure 3
MRI shows bony lesion from the anteroinferior part of lower tibial
epiphysis with epiphyseal irregularity.
Figure 4
Figure 5
Figure 5
5a: Per operative view after the excision from the anterior and antero
medial part.
5b: Removed cartilaginous mass.
Figure 6
Discussion
The etiology of Trevor disease is still unclear. Insult during the
formation of the limb bud was the reason as reported by David Trevor's [2]. Faulty growth of a part of the epiphysis or "a true dysplasia" itself was the aetiology believed by Fairbank [5].
It results from an abnormal control of cell proliferation from
the affected epiphysis. The irregular cell proliferation occurs in the
superficial zone of articular cartilage which causes changes in apical
development button of lower limb and blood epiphysary vessel
arrangements [2,5]. It also causes an imbalance between proliferation
and cellular death mechanism. [2] There are changes in fetal limb
apical ectoderm, resulting in pre or post-axial disorders [2].
Hence there is overgrowth with a cartilage cap that projects into
the adjacent joint [6]. Even though Trevor disease belongs to the
group of skeletal osteochondromas its incidence is rare. The reported
incidence of it is 1: 1,000,000 [7]. Apart from a single report of familial
incidence by Hensinger, Trevor disease is considerd neither as genetic
nor any common environmental factor in its aetiology [6,8]. It is
believed to affect the limb bud in early fetal life. Generally it affects
children of 2 and 14 years and is most frequent in boys.
The descending order occurrence in the bones are distal tibia and fibula (22%), talus and calcaneus (22%), distal femur (21%),
proximal tibia (11%), navicular, cuboid, cuneiforms, (10%), scaphoid
(2%) and scapula (1%)[5]. Hemimelic denomination came due to its
involvement only in one limb. Medial epiphyseal involvement is two
times more than the lateral [5].
Trevor disease is characterised by an asymmetrical limb deformity
because of the localized overgrowth of cartilage. Histologically it
resembles osteochondroma. Ankle or knee regions are the most
commonly affected areas and it always confined to a single limb. This
usually involves only the lower extremities and on medial side of the
epiphysis as in our case. Painless mass or swelling on one side of an
affected joint, particularly the medial side with mechanical limitation
of movement is the most common symptom. Pain usually occurs at
a later stage of the disease. Additional symptoms in each child vary
depending on the size and location of the cartilage mass, like joint
deformity, limb length discrepancy, locking of the joint and muscle
wasting, which often results limping. After the epiphyseal closure, the
disease stops its progression.
In untreated case the cartilage mass in the joint will increase in
size and undergo ossification to form a osteocartilaginous mass and
ultimately results degenerative arthritis. Degenerative findings are
more common in older patients and children usually present with
pain, edema and joint stiffness in Fairbank findings [5].
Several epiphyseal diseases are presenting with the same
radiological findings so final diagnosis of HED without more specific
examinations is difficult. Irregular and multicentric epiphyseal
opacities are common for both. Normal bone mass covered by
abundant cartilaginous foci of endochondral ossification, resembling
osteochondroma is the histological finding. Histological it is not
possible to differentiate Trevor disease from osteochondroma [5].
Genetic expression analysis of EXT1, EXT2 genes are very much
helpful. These genes are within normal ranges in Trevor disease,
while they are lower in ostechondroma (owing to a mutation) [9].
Since these genetic tests are expensive, the diagnosis is often made
on clinical and radiological findings. The differential diagnosis of
Trevor disease includes posttraumatic osseous fragments, synovial
chondromatosis, ostechondroma, or anterior spur of ankle [9].
Synovial chondromatosis can be ruled on the basis that it occurs
in much older age group [9]. Multiple epiphyseal changes can be
produced by other conditions like punctate epiphyseal dysplasia,
achondroplasia and aseptic necrosis which is also comes in the
differential diagnosis. Osteochondroma and carpotarsal dominant
osteochondromatosis are the articular calcifying tumors which
most resemble Trevor disease [10]. There is no report of malignant
transformation in the literature [11].
Computed tomography-scan is an excellent modality to define
the boundary between pathological and normal bone tissues. It is
very much helpful in the surgical planning [12]. Magnetic resonance
imaging offer better soft tissue delineation and helps to identify the
degree of soft tissues and epiphysis involvement. It has a great role in
differentiating from other tumoral diseases [13]. Eventhough bone
scintigraphy shows nonspecific findings; it can identify several HED
affected loci.
The treatment of Trevor disease is not clearly described. It
depends on the location, evolvement intensity and degree of
functional incapacity. Asymptomatic patients are just followed up
since malignant transformation is nonexistent [14]. Most reported cases of Trevor disease in the literature have been treated surgically.
Surgical excision is indicated in cases of pain, articular deformity or
incongruence, or limitation of motion. Simple excision of the mass
and correction of the deformity if present, while preserving the
integrity of the affected joint surface as much as possible is considered
as the standard treatment [9]. Acquaviva et al. [15] classified the
injuries in Trevor disease as extra or intra-articular. A simple excision
of extra-articular lesions offers good results than intra-articular
lesions. A study done by Kuo et al. [14] concludes poor outcomes
in intra-articular tumors. Arthrosis was a frequent complication
in such patients. Complete excision of the lesion is mandatory for
the prevention of tumor recidivism. Therefore, Irrespective of the
anatomopathological type, it is essential to follow-up the patient until
complete skeletal maturity [14].
Conclusion
Trevor disease is a rare developmental bone disorder
characterized by an osteocartilaginous tumor arising from the
epiphysis of long bones in children. Involvement of lower tibia is even
rarer. Even though there is no gold standard treatment described in
the literatures, the general conclusion is surgical treatment as the best.
We have described a case of Trevor disease of lower tibia in a
9 year old boy who was treated by simple surgical excision with a
general review of this uncommon disease to help the orthopedic
surgeon on the Trevor disease management.
References
- Mouchet A, Belot J. La tarsomegalie. J Radiol Electrol. 1926; 10: 289–293.
- Trevor D. Tarso-epiphysial aclasis; a congenital error of epiphysial development. J Bone Joint Surg Br. 1950; 32-B: 204–213.
- Azouz EM, Slomic AM, Marton D, Rigault P, Finidori G. "The variable manifestations of dysplasia epiphysealis hemimelica". Pediatric Radiology. 1985; 15: 44–49.
- Carlson DH, Wilkinson RH. Variability of unilateral epiphyseal dysplasia (dysplasia epiphysealis hemimelica)Radiology. 1979; 133: 369–373.
- Fairbank TJ. Dysplasia epiphysealis hemimelica (tarsoepiphyseal aclasis). J Bone Joint Surg Br 1956; 32: 237-257.
- Connor JM, Horan FT, Beighton P. "Dysplasia epiphysialis hemimelica. A clinical and genetic study". Journal of Bone and Joint Surgery Br. 1983; 65: 350–354.
- Robbin MR, Murphey MD. "Benign chondroid neoplasms of bone". Seminars in Musculoskeletal Radiology. 2000; 4: 45–58.
- Hensinger RN, Cowell HR, Ramsey PL, Leopold RG. Familial dysplasia epiphysealis hemimelica, associated with chondromas and osteochondromas. Report of a kindred with variable presentations. J Bone Joint Surg Am. 1974; 56: 1513–1516.
- Gökkus K, Aydin AT. "Dysplasia epiphysealis hemimelica: a diagnostic dilemma for orthopedic surgeons and a nightmare for parents". Journal of Postgraduate Medicine. 2014; 60: 1–2.
- Maroteaux P, Merrer LM, Bensahel H, Freisinger P. Dominant carpotarsal osteochondromatosis. J Med Genet. 1993; 30: 704–706.
- Bhosale SK, Dholakia DB, Sheth BA, Srivastava SK. Dysplasia epiphysealis hemimelica of the talus: Two case reports. J Orthop Surg (Hong Kong). 2005; 13: 79–82.
- Gerscovich EO, Greenspan A. Computed tomography in the diagnosis of dysplasia epiphysealis hemimelica. Can Assoc Radiol J. 1989; 40: 313–315.
- Iwasawa T, Aida N, Kobayashi N, Nishimura G. MRI findings of dysplasia epiphysealis hemimelica. Pediatr Radiol. 1996; 26: 65–67.
- Kuo RS, Bellemore MC, Monsell FP, Frawley K, Kozlowski K. Dysplasia epiphysealis hemimelica: Clinical features and management. J Pediatr Orthop. 1998; 18: 543–548.
- Acquaviva A, Municchi G, Marconcini S, Mazzarella F, Occhini R, Toti P, et al. Dysplasia epiphysealis hemimelica in a young girl: Role of MRI in the diagnosis and follow-up. Joint Bone Spine. 2005; 72: 183–186.