Case Report
Psoriasiform Keratosis: Report of a Rare Case and Literature Review
Mohammadreza Mortazavi1* and Somaia Ahmed Saad El-Din2
1Department of Dermatology, Al-Hayat International Hospital, Oman
2Department of Pathology, Ain Shams University, Egypt
*Corresponding author: Mohammadreza Mortazavi, Department of Dermatology, Al-Hayat International Hospital, Al-Ghubra, P.O. Box 1037, Postal Code 131, Muscat, Oman
Published: 23 May, 2016
Cite this article as: Mortazavi M, Saad El-Din SA. Psoriasiform Keratosis: Report of a Rare Case and Literature Review. Ann Clin Case Rep. 2016; 1: 1003.
Abstract
Psoriasiform keratosis is a rare, recently described entity, characterized by a solitary keratotic or scaly papule or plaque similar to seborrheic or actinic keratosis or other epidermal proliferations, but with the histopathological features that mimic psoriasis.The etiology and pathogenesis of psoriasiform keratosis remain unknown. Most of the reported lesions were located on the extremities. We here in report a 32-year-old man presented with a solitary asymptomatic keratotic papule on the right side of the neck. The histopathology of the excised lesion was consistent with psoriasiform keratosis.
Results: The abdominal pain had settled and the patient was discharged 10 days postoperatively. Conclusion: Ectopic pancreatic tissue of gastrointestinal tract is a rare condition and may presents as an acute abdomen.
Keywords: Acanthoma; Keratosis; Psoriasis; Psoriasiform keratosis
Introduction
The term psoriasiform keratosis was coined by Walsh et al. [1] in 2007 as a provisional appellation until determination of its nature as a lesion sui generis or a rudimentary presentation of psoriasis. They described it as an uncommon entity, characterized by a solitary, erythematous, scalyor keratotic papule or plaque located mostly on the extremities [1]. The clinical appearance of the reported lesions resembles seborrheic keratosis, Bowen disease, basal cell carcinoma (BCC), squamous cell carcinoma (SCC), actinic keratosis, acanthoma variants, etc [1-5]; but the histopathology of all lesions mimics psoriasis, with acanthosis, hyperkeratosis, parakeratosis, intracorneal and/or intraepidermal collections of neutrophils (in some cases) andvascular dilatation and lymphocytic infiltration in superficial dermis [1-5].
Case Report
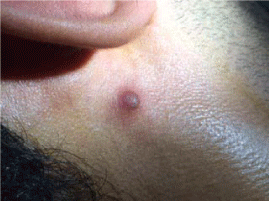
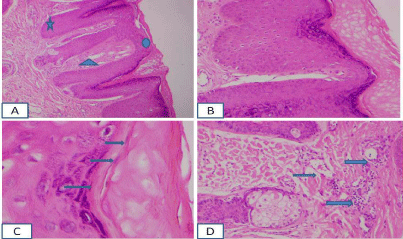
A 32-year-old male patient presented with an asymptomatic, small, red lesion on the right side of his neck, just below the ear since four months ago. He did not have any history of trauma or insect bite in that area. In physical examination, there was a solitary, darkred, firm, non-tender, roundpapule with mild scaling on the surface and anerythematous and inflamed base (Figure 1). No other significant skin or mucosal lesions were seen. He had already applied a cream containing Fusidic acid and Betamethasone valerate and then Mometasonefuroate creamfor 3 weeks without improvement. The lesion was completely excised and sent for histopathological evaluation with the clinical impressions of inflamed seborrheic keratosis, clear cell acanthoma and basal cell carcinoma. Histopathological examination revealed epidermal acanthus is with elongated rete ridges associated with thinning out of the epidermis over the dermal papillae (i.e. psoriasiform hyperplasia) (Figure 2A). Preserved granular cell layer with hyperkeratosis (Figure 2B) and few foci of mild parakeratosis (Figure 2C) were also noted. The dermal papillae and the superficial dermis showed many dilated vessels with mild perivascular collections of lymphocytes and macrophages (Figure 2D).
Figure 1
Figure 2
Figure 2
A: Epidermal acanthosis with elongated rete ridges (star) associated with thinning of the epidermis over the dermal papillae (circle) and many dilated vessels in the dermal papillae (tringle); B: Preserved granular cell layer with hyperkeratosis.
Differential Diagnosis
Despite the different clinical features of the lesion, the histopathological findings unexpectedly resembled that of psoriasis. Inflamed or irritated seborrheic keratosis was excluded by the absence of acanthosis formed by basal cells interspersed with horn cysts, squamous eddies and/or marked inflammation. The absence of the glycogen-rich clear cells and also the lack of acantholysis in the epidermis excluded clear cell acanthoma and other types of acanthoma (such as acantholytic and epidermolytic acanthomas and warty dyskeratoma), respectively. Basal cell carcinoma and other malignant or premalignant epidermal lesions were excluded in the absence of any epidermal atypia, abnormal mitosis or invasive epithelial nests with desmoplastic stromal reaction.
Discussion
Psoriasiform keratosis (PK) was described for the first time by Walsh et al. [1] in 2007 as a probably distinct clinicopathological entity. They and then Mutasim reported several cases with various clinical diagnoses such as seborrheic keratosis, Bowen disease, BCC, actinic keratosis, SCC, lichenoid keratosis, large cell acnthoma, verruca vulgaris, etc., but with similar psoriasiform histopathology [1,2]. According to the concept of unilesional presentation, they suggested that the relationship of psoriasiform keratosis to psoriasis resembles that of the benign lichenoid keratoses to lichen planus [6,7] or pagetoid reticulosis to multilesional mycosis fungoides [8,9]. Among all the reported cases of PK that had histopathological features of psoriasis, none developed the clinical evidence of disseminated psoriasis in their next follow-up visits [1-5]. The inefficacy of topical corticosteroids in treatment of the PK lesions in the cases reported by Carbone et al. [3] and Pires et al. [5] and also in our presented case, implies the fact that psoriasiform keratosis is probably a sui generis epidermal proliferation with psoriasiform histological features rather than a variant of the inflammatory disease, psoriasis.
To date, to the best of our knowledge, only 32 cases of psoriasiform keratosis (including the current case) have been reported in the literature [1-5], but its actual incidence and prevalenceremains to be determined. The etiopathogenesis of psoriasiform keratosis is still unknown, but some authors are in favor of classifying PK in the group of cutaneous acanthomas which includes clear cell acanthomas, lichenoid keratosis, seborrheic keratosis, acantholytic acanthoma and warty dyskeratoma [2]. Sezer et al. [4] detected human papilloma virus (HPV) type 6 in the tissue specimen of their reported case, using the polymerase chain reaction (PCR) technique. The role of HPV in pathogenesis of some skin neoplasms such as Bowen disease, SCC and bowenoid papulosis is well-known [10]. Recent isolation of HPV in some benign epidermal proliferations including large cell acanthoma, stucco keratosis (a variant of seborrheic keratosis) and skin tag (acrochordon) suggests the probable role of HPV in etiopathogenesis of these lesions, as well [11-13]. More extensive investigations for confirming the etiopathogenic role of HPV in development of PK are necessary.
The age of all reported cases in the literature were more than 55 years, except two patients in the first case series who were 47 and 30 years old at the time of presentation [1-5]. The mean age of patients in Walsh et al. [1] case series and in Mutasim cases were 66.8 and 73.2 years, respectively [2]. Our current case was a 32-year-old man. Regarding the gender of the reported cases, the incidence of PK in males was almost equal to females.
The lesions in the reported cases were mostly located on the upper or lower extremities. The location of the lesions in only a few cases in the first case series (and in our case) was on the other areas including scalp, trunk and neck [1-5].
Histopathological evalauation of psoriasiform keratosis in Walsh et al. [1]and Sezer et al. [4] reported cases showed regular and irregular acanthosis, focal or confluent parakeratosis with ectatic vessels in the papillary dermis and a sparse superficial perivascular lymphocytic infiltration. The majority of cases reported by Mutasim (12 out of 13 lesions) revealed psoriasiform pattern with focal rather than confluent compact parakeratosis, similar to our case. Our presented case showed well-developed granular cell layer that is not a feature of classic psoriasis but may be seen in psorisiform keratosis. Four out of 13 lesions were examined by Mutasim had well-developed granular cell layer, while all other lesions showed preserved granular cell layer with variable reduction in their thickness [2].
Some of the authors, have reported collections of neutrophils in the stratum corneum and/or intraepidermal spongiform neutrophilic pustules in most but not all of their cases [1,2,4]. Our presented case did not have significant neutrophilic infiltration in the epidermis.
In conclusion, psoriasiform keratosis is a recently described entity characterized by a solitary keratotic papular lesion with psoriasiform histology. It is still not clear that it should be considered as a unilesional presentation of psoriasis or it should be classified in the group of cutaneous acanthomas.
References
- Walsh SN, Hurt MA, Santa Cruz DJ. Psoriasiform keratosis. Am J Dermatopathol. 2007; 29: 137-140.
- Mutasim DF. Psoriasiform keratosis: a lesion mimicking psoriasis. Am J Dermatopathol. 2007; 29: 482-484.
- Carbone A, De Simone C, Valenzano F, Amerio P, Massi G. Psoriasiform keratosis. Eur J Dermatol. 2009; 19: 631-632.
- Sezer E, Böer A, Falk T. Identification of human papilloma virus type 6 in psoriasiform keratosis. Am J Dermatopathol. 2010; 32: 492-494
- Pires CA, Sousa BA, Nascimento CSS, Moutinho AT, Miranda MF, Carneiro FR. Psoriasiform keratosis - case report. An Bras Dermatol. 2014; 89: 318-319
- Prieto VG, Casal M, McNutt NS. Lichen planus-like keratosis. A clinical and histological reexamination. Am J Surg Pathol. 1993; 17: 259-263.
- Berger TG, Graham JH, Goette DK. Lichenoid benign keratosis. J Am Acad Dermatol. 1984; 11: 635-638.
- Burns MK, Chan LS, Cooper KD. Woringer-Kolopp disease (localized pagetoid reticulosis) or unilesional mycosis fungoides? An analysis of eight cases with benign disease. Arch Dermatol. 1995; 131: 325-329.
- Oliver GF, Winkelmann RK, Banks PM. Unilesional mycosis fungoides: clinical, microscopic and immunophenotypic features. Australas J Dermatol. 1989; 30: 65-71.
- Dubina M, Goldenberg G. Viral-associated nonmelanoma skin cancers: a review. Am J Dermatopathol. 2009; 31: 561–573.
- Berger T, Stockfleth E, Meyer T, Kiesewetter F, Funk JO. Multiple disseminated large-cell acanthomas of the skin associated with human papillomavirus type 6. J Am Acad Dermatol. 2005; 53: 335-337.
- Stockfleth E, Röwert J, Arndt R, Christophers E, Meyer T. Detection of human papillomavirus and response to topical 5% imiquimod in a case of stucco keratosis. Br J Dermatol. 2000; 143: 846-850.
- . Dianzani C, Calvieri S, Pierangeli A, Imperi M, Bucci M, Degener AM. The detection of human papillomavirus DNA in skin tags. Br J Dermatol. 1998; 138: 649-651.